Acute Kidney Injury
Mahahalagang Punto
- Ang acute kidney injury (AKI) ay biglaang pagkawala ng kidney function sa loob ng oras hanggang araw — nababaliktad kung maagang matukoy at magamot.
- Tatlong pathophysiological categories: prerenal (nabawasang blood flow sa kidneys), intrarenal (direktang pinsala sa kidney tissue), at postrenal (urinary outflow obstruction).
- Critical lab indicators: tumataas na serum creatinine, elevated BUN, nabawasang GFR, at hyperkalemia — ang hyperkalemia ang pinakaagad na life-threatening na electrolyte implication.
- Priority nursing goal: urine output >=30 mL/hour; ang oliguria (<400 mL/day) o anuria (<50 mL/day) ay senyales ng severe impairment.
- Management: gamutin ang underlying cause, IV fluids (prerenal), alisin ang nephrotoxins, electrolyte correction, at dialysis sa severe cases.
Patopisyolohiya
Tatlong Kategorya ng AKI
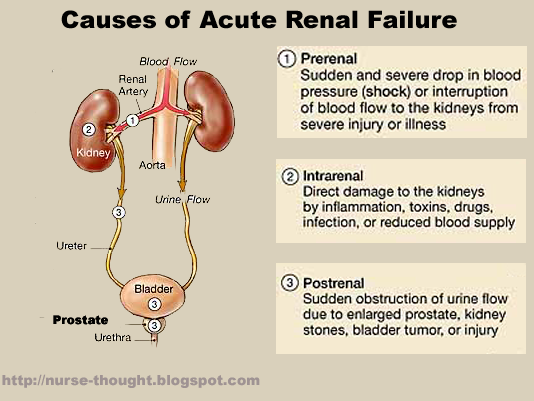 Sanggunian ng ilustrasyon: OpenRN Health Alterations Ch.8.5.
Sanggunian ng ilustrasyon: OpenRN Health Alterations Ch.8.5.
| Type | Mechanism | Examples |
|---|---|---|
| Prerenal | Nabawasang renal blood flow → nabawasang glomerular perfusion | Hypovolemia, hemorrhage, [sepsis], cardiogenic shock, severe heart-failure(heart failure), vascular obstruction |
| Intrarenal | Direktang pinsala sa renal tubules o nephrons | Prolonged ischemia, acute tubular necrosis mula sa thrombotic perfusion compromise, nephrotoxic drugs (aminoglycosides, [nsaids], contrast media), rhabdomyolysis (myoglobin), hemolysis (hemoglobin) |
| Postrenal | Mechanical obstruction ng urinary outflow → urine backflow na sumisira sa kidney | benign-prostatic-hyperplasia(Benign prostatic hyperplasia) (BPH), prostate-cancer(prostate cancer), kidney stones, urethral stricture, pelvic tumors |
Kabilang din sa prerenal causes ang severe burns at iba pang high-volume fluid-loss states. Maaaring mangyari ang intrarenal injury sa interstitial nephritis, vasculitic o malignant-hypertension vascular injury, at piling heavy-metal toxic exposure. May ilang acute tubular injury episodes na pansamantala kapag naitama agad, ngunit ang delayed recognition ay maaaring mag-iwan ng persistent renal dysfunction.
High-risk populations: older adults (natural decline sa renal reserve), clients na may CKD, diabetes, hypertension, heart failure, liver disease, autoimmune disease, dehydration, blood-loss/trauma burden, severe infection, o kamakailang exposure sa nephrotoxins o contrast dye.
Nursing Assessment
Pokus sa NCLEX
Ang hyperkalemia sa AKI ang priority electrolyte emergency — hindi kayang ilabas ng kidneys ang potassium, at ang mataas na levels ay nagdudulot ng fatal cardiac dysrhythmias. Palaging iugnay ang potassium levels sa ECG changes (peaked T waves, wide QRS, sine wave pattern).
Clinical manifestations by system:
| System | Manifestations |
|---|---|
| Renal | Oliguria (<30 mL/hr), anuria, uremia (elevated BUN/creatinine, uremic frost sa severe cases) |
| Cardiovascular | Hypertension (fluid overload), pitting edema, heart-failure(heart failure), arrhythmias mula sa hyperkalemia, pericarditis |
| Respiratory | Dyspnea mula sa pulmonary edema, Kussmaul breathing (severe metabolic-acidosis(metabolic acidosis)) |
| Neurological | Confusion, asterixis (flapping tremor), peripheral neuropathy, seizures |
| GI | Nausea, vomiting, anorexia, gastritis, GI bleeding |
| Hematologic | Anemia (↓ erythropoietin), bleeding tendencies |
| Integumentary | Pruritus, pallor, dry skin, ecchymosis, uremic frost (severe) |
| Endocrine | Hyperkalemia, hyponatremia, metabolic acidosis, insulin resistance |
Priority laboratory findings:
- Serum creatinine: elevated (primary indicator)
- BUN: elevated (nakatutulong ang creatinine:BUN ratio para ihiwalay ang prerenal vs intrarenal)
- GFR: decreased
- Potassium: hyperkalemia — pinaka-urgent
- Sodium: hyponatremia (dilutional)
- Arterial blood gas: metabolic acidosis (low pH, low HCO3)
- CBC: anemia, elevated WBC kung infection ang sanhi
- Urinalysis at renal ultrasound: suriin ang structural causes, obstruction, at infection contributors
Nursing Interventions
Tukuyin at gamutin ang underlying cause:
- Prerenal: ibalik ang circulating volume gamit ang IV fluids (isotonic crystalloids) — mapabuti ang renal perfusion
- Intrarenal: tukuyin at ihinto ang nephrotoxins; maaaring i-hold ang medications na nakaaapekto sa renal blood flow (NSAIDs, ACE inhibitors)
- Postrenal: alisin ang obstruction (urethral catheter para sa BPH, nephrostomy tube para sa stone/tumor)
Fluid at electrolyte management:
- I-monitor ang urine output bawat oras — target >=30 mL/hour; maglagay ng indwelling catheter para sa tumpak na pagsukat
- Hyperkalemia management: insulin + dextrose (inihihift ang K+ papasok sa cells), sodium bicarbonate, kayexalate (inaalis ang K+ mula sa katawan), cardiac monitoring — suriin ang ECG para sa peaked T waves, widened QRS
- Para sa severe hyperkalemia na may ECG instability, asahan ang calcium-gluconate support upang patatagin ang myocardial excitability habang isinasagawa ang potassium-lowering therapy.
- Fluid restriction kung oliguric upang maiwasan ang fluid overload
- Sodium at fluid restriction ayon sa reseta; dietary phosphorus at protein restriction sa established AKI
Dialysis indications (severe AKI): refractory fluid overload, severe hyperkalemia, symptomatic uremia, metabolic acidosis na hindi tumutugon sa paggamot — hemodialysis (acute), peritoneal dialysis, o continuous renal replacement therapy (CRRT) para sa hemodynamically unstable clients.
- Kung sinimulan ang dialysis, i-coordinate ang pre-treatment medication review dahil may ilang medications na dialyzable o maaaring magpalala ng intradialytic hypotension.
Medication safety:
- Iwasan o i-dose-adjust ang lahat ng renally cleared medications (digoxin, antibiotics, NSAIDs, contrast dye)
- I-hold ang ACE inhibitors, ARBs, diuretics sa prerenal AKI hanggang maibalik ang volume
- Kumonsulta sa pharmacy para sa renal dosing adjustments
- Tiyaking nasusukat at nadodokumento nang tumpak ang intake/output sa bawat shift at tine-trend sa loob ng 24 oras.
- I-monitor ang daily weights upang suportahan ang fluid-balance decisions (humigit-kumulang 1 lb gain ay maaaring sumalamin sa humigit-kumulang 1 L fluid accumulation), lalo na sa dialysis care windows.
Acute Oliguria
Ang urine output na <0.5 mL/kg/hour nang higit sa 6 magkakasunod na oras ay criterion para sa AKI at nangangailangan ng agarang provider notification. Huwag maghintay ng laboratory confirmation — kumilos batay sa clinical cues.
Mga Kaugnay na Konsepto
- urinary system — Naaabala sa AKI ang normal glomerular filtration at nephron function.
- kidney disease — Ang AKI bilang risk factor para sa CKD development; ihambing ang acute vs chronic presentations.
- potassium balance disorders — Hyperkalemia management bilang pinakamataas na prayoridad na AKI electrolyte complication.
- nursing management ng peritoneal at hemodialysis — Mga dialysis modalities at nursing care sa severe AKI.
- fluid volume overload-hypervolemia — Fluid overload management sa oliguric AKI.
- bladder assessment — Urine output monitoring at oliguria recognition sa AKI.
Sariling Pagsusuri
- Paano mo ihihiwalay ang prerenal mula intrarenal AKI batay sa clinical history at laboratory values?
- Ang client na may AKI ay may potassium level na 6.8 mEq/L at may peaked T waves sa ECG. Ano ang priority nursing action?
- Kailan dapat i-hold ng nurse ang IV fluid administration para sa client na may AKI, at aling assessment finding ang gagabay sa desisyong ito?