Stress and Anxiety
Key Points
- Stress is the body-mind response to perceived challenge; anxiety is fear or unease that can become impairing when persistent.
- Acute stress may be adaptive, but chronic stress worsens physical and psychiatric outcomes.
- Stress patterns include acute, episodic acute, chronic, eustress, and distress with different clinical implications.
- Unmanaged chronic stress can impair needs across physiologic stability, safety, belonging, esteem, and self-actualization.
- In nursing work, unmanaged distress can degrade team relationships, increase workplace errors, and accelerate burnout/turnover.
- Anxiety exists on a continuum from mild arousal to panic-level dysregulation.
- Anxiety burden is common: U.S. 12-month prevalence is near one-fifth of adults, with higher reported prevalence in females than males.
- Nursing management combines coping-skills coaching, lifestyle supports, and targeted therapies.
- In life-limiting illness, anxiety often rises around prognosis, mortality, symptom burden, and perceived loss of control.
- In pediatric hospitalization, child anxiety commonly co-regulates with caregiver emotional state and can present as separation distress, stranger distress, or temporary regression.
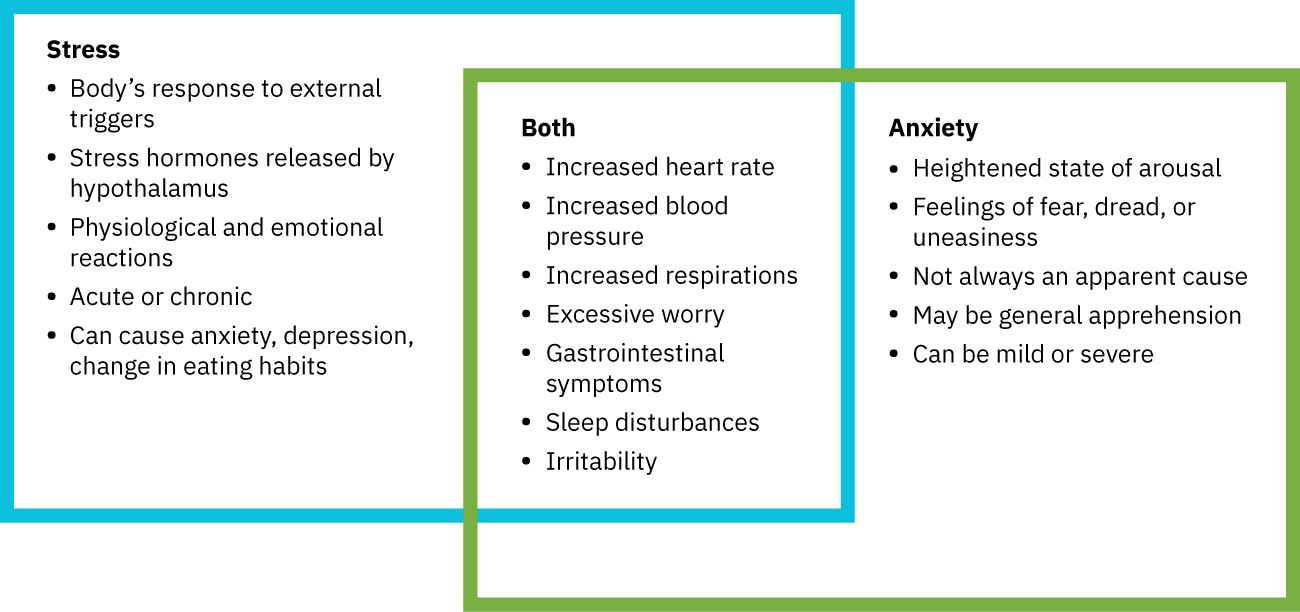 Illustration reference: OpenStax Psychiatric-Mental Health Nursing Ch.17.1.
Illustration reference: OpenStax Psychiatric-Mental Health Nursing Ch.17.1.
Pathophysiology
Stress activates sympathetic and neuroendocrine pathways (fight-or-flight), increasing heart rate, blood pressure, vigilance, and stress-hormone output. A core neuroendocrine sequence is CRH release from the hypothalamus, ACTH release from the anterior pituitary, and cortisol release from the adrenal cortex, with sympathetic catecholamine effects occurring in parallel.
Fear is usually a response to an immediate, identifiable threat, whereas anxiety more often reflects apprehension about a vague, anticipated, or uncertain threat; both can activate the same physiologic stress-response systems.
Acute stress is often time-limited and may resolve with recovery to baseline. Repeated or prolonged activation without adequate parasympathetic recovery can disrupt sleep, immune function, metabolism, mood regulation, and cognition. In bedside teaching, acute stress is usually framed as short-term exposure, whereas chronic stress reflects persistent burden lasting several months or longer.
Acute stress behavior may present as fight, flight, freeze, or fawn responses depending on threat interpretation and prior experience.
Anxiety disorders emerge when fear-processing systems remain overactive and disproportionate to actual threat. Clinically, anxiety may represent either a primary psychiatric disorder or a secondary stress symptom during acute/chronic medical illness; family-history burden can also increase vulnerability in some patients.
Appraisal also shapes response quality: the same stressor may be experienced as eustress (constructive activation) or distress (harmful burden) depending on perception, coping resources, and contextual support. Internal stressors are strongly appraisal-dependent and can vary by age, sex, prior experience, personal values, cultural or religious framework, and available resources, while external stressors arise from outside events (for example infection, injury, or urinary retention).
When chronic distress persists, physiologic strain and maladaptive behavior can reinforce each other (for example low energy worsening inactivity, poor diet, social withdrawal, or substance-related coping), accelerating long-term morbidity. Cognitive effects vary by stress phase: early alarm activation may briefly sharpen focus, while prolonged stress often impairs information processing, rational decision-making, and memory reliability.
The psychophysiological stress model emphasizes bidirectional cycling between body and mind: anxiety can begin as a stress consequence, but it can also become a new stressor that perpetuates autonomic and endocrine activation.
Classification
- Stress response domains: Physiologic, emotional, and behavioral reactions.
- Stress-duration domain: Acute stress (short-lived, recovery-capable) versus chronic stress (persistent activation and higher health burden).
- Stress subtype domains: Acute, episodic acute, chronic, eustress, and distress.
- Stress-valence domain: Neutral stress, positive adaptive stress (eustress), and negative harmful stress (distress).
- Stress-intensity continuum: Mild daily stress through severe life-threatening stress exposure with corresponding escalation in physiologic response.
- Stressor-origin domain: Physiologic stressors (illness, injury, pain, malnutrition, temperature extremes) and psychosocial stressors (grief, conflict, addiction, mental illness, ineffective coping).
- Stressor-location domain: Internal stressors (appraisal-driven interpretation) and external stressors (outside-body or environmental triggers).
- Stressor-scale domain: Significant life changes, catastrophic events, frequent annoyances, and omnipresent irritations.
- Common stressor domains: Environmental, lifestyle, major-life-event, organizational-routine, physiologic illness/pregnancy, and financial-pressure stressors.
- Stressor-context domain: Developmental stressors (lifespan milestones), situational stressors (unexpected personal events), and adventitious stressors (traumatic disaster/violence events).
- Life-stage vulnerability domain: Children (limited coping-language/regulation capacity) and older adults (cognitive/functional stress-amplifying factors) may show different but clinically significant stress responses.
- Appraisal domain: Stressor interpretation as growth challenge versus threat/harm expectation.
- Transactional model domain: Stress response reflects a person-environment transaction shaped by personal, social, environmental, spiritual, cultural, educational, and emotional-regulation factors.
- Psychophysiological coupling domain: Mental distress amplifying physical strain and physical strain amplifying anxiety/distress.
- Coping domains: Problem-focused, emotion-focused, and resilience-oriented strategies.
- Coping quality: Adaptive (problem-solving, mindfulness, support use) versus maladaptive (avoidance, withdrawal, aggression, substance misuse).
- Defense-mechanism pattern: Protective responses may be adaptive in limited use, but excessive/maladaptive reliance can worsen functioning and psychiatric burden.
- Need-impact domain: Effects on physiologic function, safety/resource stability, belonging, esteem, and higher-level fulfillment.
- Self-regulation domains: Physiologic regulation (SNS-to-PNS balance), emotional regulation, and behavioral regulation aligned with long-term values.
- Anxiety-intensity levels: Mild, moderate, severe, and panic.
- Level progression cues: Mild (focused energy with manageable restlessness), moderate (selective inattention, hampered learning/problem-solving, sympathetic activation), severe (markedly narrowed perceptual field, dazed/confused automatic behavior, and near-total loss of learning/problem-solving), panic (disorganized behavior and inability to process external cues).
- Panic-level profile: May include pacing/running/shouting/screaming or abrupt withdrawal, occasional transient reality-contact disturbance, and post-episode exhaustion.
Nursing Assessment
NCLEX Focus
Differentiate adaptive stress from pathologic anxiety by duration, intensity, and functional impact.
- Assess stressors, symptom pattern, and duration.
- Assess stressor origin and scale to clarify whether symptoms are primarily physiologic-triggered, psychosocial-triggered, or mixed.
- Assess individualized stress response drivers, including physical state, emotional state, and cognitive understanding/appraisal of the stressor.
- Assess appraisal modifiers that change internal stressor intensity, including age, sex, lived experience, values, cultural/religious beliefs, and practical resources.
- Assess transactional context (social supports, environment, spirituality/culture, educational background, and emotional-regulation capacity) because it changes stress-response trajectory.
- Differentiate stress subtype (acute, episodic acute, chronic, eustress, or distress) and its functional impact.
- Assess personal adaptation factors: baseline coping capacity, current health burden, support-system reliability, and SES/SDOH constraints.
- Assess predisposing risk factors for poor adaptation, including early-life adversity (for example prenatal stress and ACE burden), chronic optimism/pessimism pattern, previous coping failures, and unresolved health/surgical sequelae.
- Assess life-stage modifiers directly: children may have limited stress vocabulary and impulse-control coping, while older adults may have cognitive slowing, mobility decline, and independence-related stress amplification.
- Assess which need levels are disrupted (physiologic, safety/resources, belonging, esteem, and self-actualization goals).
- Assess acute autonomic cues (elevated heart rate/respiratory rate/blood pressure, dilated pupils, diaphoresis).
- In moderate anxiety, assess selective inattention plus physiologic cues such as sweating, tachycardia/tachypnea, headache, gastric discomfort, urinary urgency, voice tremor, and shakiness.
- In severe anxiety, assess for hyperventilation, pounding heart, insomnia, confusion/dazed presentation, automatic behavior, and expressed sense of impending doom.
- Assess distress-linked emotional and somatic cues (for example unease, sadness, pain, and nonspecific symptom clusters that are difficult to localize).
- Assess chronic stress patterns (irritability, fatigue, headache, poor concentration, insomnia, digestive changes, appetite changes, helplessness, low self-esteem, frequent illness, reduced sexual desire).
- Assess overlap pattern of acute-on-chronic burden (for example new injury/infection layered on chronic illness) because combined stressors can rapidly worsen coping and physiologic stability.
- Assess cumulative stress stacking (multiple simultaneous stressors) and practical burden barriers (cost, transportation, income loss, and care-access friction).
- Assess for withdrawal-associated stress physiology in at-risk patients (for example anxiety with tachycardia and marked hypertension after abrupt substance cessation).
- When anxiety is persistent, trend severity using structured self-report tools when available (for example STAI and BAI) and correlate with functional impairment.
- Use objective adjuncts when needed (for example heart rate/blood pressure/respiratory trends, ECG-based autonomic response, or skin-conductance measures) while recognizing anxiety remains primarily a clinical and subjective diagnosis.
- If presentation and context are unclear, include behavior-based assessment (for example approach-avoidance response to feared stimuli) with safety safeguards.
- Assess multidomain distress manifestations in workforce settings: physical (for example headache, sleep disruption, palpitations/blood-pressure elevation, GI changes, tremor, diaphoresis), mental (for example anger, irritability, mood change, isolation, reduced confidence), and behavioral (for example increased alcohol/substance use, appetite shift, conflict escalation, workplace error increase).
- Assess cognitive distortions (catastrophizing, all-or-nothing thinking, overgeneralization, jumping to conclusions, personalization, and threat overestimation).
- Assess current coping style effectiveness and available social supports.
- Assess support-system strength because poor family/friend support increases risk of persistent distress.
- Assess safety concerns, including escalation to panic, self-harm risk, or substance misuse.
- Assess whether anxiety is physiologically stress-induced by active medical illness (for example severe cardiopulmonary or pain crises) before concluding a primary anxiety disorder.
- Assess colleague-observed stress signals (for example irritability, withdrawal, fatigue, error increase, or absenteeism) because external observation may identify distress earlier than self-report.
- In pediatric-family contexts, assess dyadic escalation patterns (caregiver anxiety transmission, prolonged goodbye patterns, and child loss-of-control behavior under hospitalization stress).
- Screen for panic features (palpitations, chest discomfort, paresthesias, lightheadedness, depersonalization, acute fear of losing control) and treat sudden severe presentations as urgent while medical emergencies are ruled out.
- Distinguish panic as a continuum-level anxiety state from a DSM-defined panic-attack episode with specific diagnostic criteria.
- Assess stress-related cognitive performance (processing speed, concentration, memory recall, and decision quality), especially during high-stakes care discussions.
Nursing Interventions
- Teach grounding, paced breathing, and relaxation techniques for acute symptom reduction.
- Reinforce adaptive self-regulation practices such as reflection/journaling, healthy boundary setting, structured positive self-talk, and psychotherapy referral when maladaptive defense patterns persist.
- When defense mechanisms are prominent, use nonjudgmental active listening and open-ended exploration instead of direct confrontation, then support gradual insight as readiness improves.
- Teach relaxation breathing: comfortable position, slow diaphragmatic breaths, inhale/exhale counts, and minimum 5-minute practice.
- Coach problem-solving and time-management skills for controllable stressors.
- Use stepwise adaptation coaching: identify predisposing risk factors, identify the stressor, clarify personal feelings, choose prioritized actions, and reassess outcomes.
- For physiologic stressors, prioritize cause-directed care (for example hydration, pain control, nutrition support, temperature management) while monitoring return to baseline.
- For external physiologic stressors (for example infection/injury or urinary retention), prioritize direct trigger relief (such as antimicrobials, procedures, or catheterization when indicated) to reduce ongoing stress activation.
- When medical illness is the likely stressor, treat the underlying physiologic trigger while concurrently using anxiety-reduction communication and coping support.
- Promote sleep hygiene, activity, and nutrition to reduce physiologic burden.
- For chronic distress cycles, pair symptom care with health-habit reset plans (nutrition, activity, tobacco/substance reduction, and social reconnection).
- Build practical daily coping plans: set boundaries, use realistic expectations, avoid alcohol/illicit drugs/tobacco coping, and schedule social connection.
- Co-design constructive actions that improve access to coping resources (for example mobility aid placement, water availability, and practical support setup) and avoid destructive options that add secondary distress.
- Distinguish willingness from ability to change and use motivational interviewing plus staged goals when readiness is mixed.
- Coach diet-related stress hygiene by limiting simple carbohydrates, excess caffeine, and stress-related overeating patterns.
- Teach WHO-style micro-skills for intrusive stress reactions: grounding, unhooking, values-based action, kindness, and making room for difficult feelings.
- Teach practical grounding sequence for acute overload: notice thoughts/feelings, slow breathing, reconnect to body posture, then orient with five-senses prompts.
 Illustration reference: OpenStax Psychiatric-Mental Health Nursing Ch.17.1.
Illustration reference: OpenStax Psychiatric-Mental Health Nursing Ch.17.1. - Use brief reality reorientation plus paced breathing when perceived threat is disproportionate to objective danger, to reduce sympathetic escalation.
- Use compassionate pacing and active listening to identify the patient’s highest-priority concern, which may differ from assumed stressors.
- Provide clear written information and repeat key teaching when stress burden is high because real-time cognitive processing may be reduced.
- Teach unhooking sequence for intrusive thoughts: notice, name (“I notice…”), and refocus on the present task or person.
- Use brief cognitive reframing prompts (for example, “What is the worst realistic outcome right now?”) to interrupt catastrophic thought spirals.
- Teach mindfulness in nonjudgmental present-centered terms: notice thoughts/feelings as they arise, accept their presence, and choose a deliberate response instead of automatic reaction.
- Teach world-events stress hygiene: limit repeated news/social-feed exposure, do a brief self-check before consuming difficult headlines, and schedule screen-disconnection periods.
- Offer emotion-focused options such as mindfulness meditation, guided imagery, and yoga when aligned with client preference and capacity.
- For selected clients with trained-provider access, consider adjunctive biofeedback or hypnotherapy as part of a broader anxiety-management plan.
- Include humor-based reframing and safe laughter activities as optional emotion-focused coping tools when culturally appropriate and acceptable to the client.
- Train self-regulation skills by pairing symptom awareness (breath, heart rate, muscle tension) with intentional PNS-activating techniques.
- Encourage routine self-monitoring with brief standardized stress tools (for example perceived-stress screening) so distress escalation is identified early.
- Reinforce resilience-building habits and support-network engagement.
- Reinforce resilience during prolonged public stress periods: maintain preventive health routines, protect sleep/activity/nutrition basics, and use intentional phone/video social connection to reduce isolation.
- Use peer-support communication when harmful stress signs are noticed (for example nonjudgmental “I noticed…” check-ins) and share formal support options early.
- Coordinate psychotherapy/pharmacotherapy referral when anxiety impairs function.
- Use physical down-regulation techniques such as breathing-based biofeedback and short cooling-compress application to head/face/neck when clinically appropriate.
- Optimize healing environment cues by reducing noise/news exposure (for example turning off distressing media and using calming/nature audio when available).
- For extreme anxiety or panic, stay with the client, reduce environmental stimuli, use calm/brief reassurance, and prioritize immediate safety.
- In pediatric separation distress, coach caregivers to use calm brief goodbyes, maintain predictable routines, and use familiar comfort objects/distraction rather than prolonged reassurance cycles that increase anxiety.
- Discuss complementary approaches (for example massage, acupuncture, chamomile, kava, melatonin, lavender) with caution because evidence is mixed and interaction risk can exist.
Chronic-Stress Normalization
Treating severe chronic stress as “normal life pressure” delays care and increases morbidity.
Pharmacology
Medication options for anxiety may include SSRIs/SNRIs, buspirone, and short-term benzodiazepine use in selected contexts. Nursing care must monitor dependency risk, withdrawal risk, side effects, and functional response.
Clinical Judgment Application
Clinical Scenario
A client reports persistent worry, insomnia, muscle tension, gastrointestinal upset, and declining concentration at work for months.
- Recognize Cues: Multi-domain anxiety burden with functional decline.
- Analyze Cues: Pattern exceeds short-term adaptive stress response.
- Prioritize Hypotheses: Priority is anxiety disorder evaluation and immediate coping support.
- Generate Solutions: Combine symptom-regulation skills with therapy/medication pathway.
- Take Action: Implement grounding education, sleep plan, and referral coordination.
- Evaluate Outcomes: Reassess anxiety severity, function, and coping capacity.
Related Concepts
- anxiety-related-disorders - Expands diagnosis-specific anxiety conditions and interventions.
- self-harm-and-suicide - Addresses escalation risk in severe anxiety/depressive overlap.
- the-spectrum-of-mood-disorders - Supports differential evaluation with mood-spectrum states.
- trauma-induced-and-stress-related-disorders - Links chronic stress responses with trauma syndromes.
- client-engagement - Improves adherence to anxiety-management plans.