Self-Concept Components and Lifespan Development
Key Points
- Self-concept is a dynamic perception of self that changes with development, social context, and life events.
- Core components include self-image, self-esteem, ideal self, personal identity, social identity, body image, and role performance.
- Congruence between actual self and ideal self supports well-being, while major discrepancy can cause distress.
- Actual, ideal, and ought self can create growth-driving tension, but persistent mismatch increases emotional strain.
- Different self-discrepancy patterns often map to distinct emotions, including disappointment, shame, fear, or guilt.
- Shame-driven conformity can produce a protective “false self” pattern that weakens authenticity and resilience.
- Social comparison (upward and downward) can either motivate growth or worsen self-judgment, depending on context.
- Persistent body-image dissatisfaction can increase risk for anxiety, depression, and maladaptive coping behaviors.
- Positive self-concept supports engagement in self-care, chronic-disease management, and health-promoting behaviors.
Pathophysiology
Self-concept is a psychosocial construct shaped by cognition, emotion, social feedback, and meaning-making. It is not static; it changes as individuals integrate new experiences and reinterpret identity over time.
Early development establishes foundational self-recognition and social belonging. Adolescence intensifies identity exploration, and adulthood continuously recalibrates self-concept through relationships, work, health status, and role transitions.
Reflected appraisal also shapes identity formation: repeated messages from significant others can be internalized as self-defining labels. Supportive feedback can strengthen agency, while persistent negative labeling can entrench shame-based self-narratives.
Symbolic interaction processes are especially influential in childhood and adolescence. Caregiver, teacher, and peer appraisals shape how children interpret their own strengths and limitations, and these interpretations are repeatedly revised during identity formation.
When self-appraisal remains flexible and realistic, individuals are more likely to sustain resilience and adaptive coping. Rigid or negatively distorted appraisal increases vulnerability to shame, avoidance, and impaired functioning.
Alignment between self-image and ideal self is a key stabilizer. Sustained mismatch can amplify anxiety, depressed mood, and preoccupation with perceived appearance flaws.
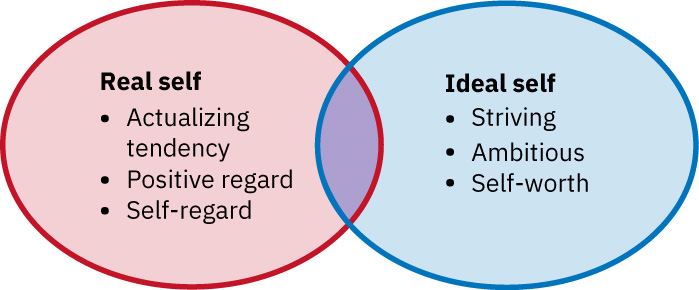 Illustration reference: OpenStax Fundamentals of Nursing Ch.32.1.
Illustration reference: OpenStax Fundamentals of Nursing Ch.32.1.
The self-system also includes the actual self (current lived identity) and ought self (internalized standards and “should” expectations). When expectations are rigid and externally driven, self-criticism and role strain often intensify.
Emotional burden differs by discrepancy type. Actual-versus-ideal mismatch often presents as disappointment or frustration, while mismatch against others’ expectations more often presents as shame or embarrassment. Actual-versus-perceived duty mismatch can produce agitation and fear of consequences, and mismatch with personal duty standards can present as guilt and inadequacy.
Chronic pressure to conform can drive a “false self” pattern in which patients overinvest in approval-seeking roles while suppressing authentic preferences and limits. This pattern may briefly reduce interpersonal conflict but commonly increases exhaustion, resentment, and self-worth instability over time.
Social comparison is another core mechanism. Upward comparison may support skill growth when framed constructively, but can intensify inferiority and hopelessness when standards feel unattainable. Downward comparison may provide short-term relief yet can also reinforce avoidance of meaningful growth goals.
During school-age development, children become especially sensitive to competence comparisons in academics, social participation, and physical skills. Feedback quality from caregivers and teachers therefore has outsized influence on emerging self-worth and confidence.
Classification
- Structural components: Self-image, self-esteem, ideal self, personal identity, social identity, body image, role performance.
- Self facets: Actual self, ideal self, and ought self.
- Self-discrepancy patterns: Actual-versus-ideal mismatch and actual-versus-ought mismatch.
- Discrepancy-emotion patterns: Disappointment/frustration, shame/embarrassment, fear/agitation, guilt/inadequacy.
- Identity-protection patterns: Authentic-self expression versus false-self conformity.
- Social-mirror processes: Reflected appraisal and internalized labels from meaningful relationships.
- Developmental context: Childhood formation, adolescent identity integration, adult role adaptation.
- Early developmental milestones: Infancy self-awareness, mirror-based self-recognition around 18 months, and self-definition expansion in early childhood.
- School-age integration factors: Peer comparison, performance feedback, and domain-specific competence beliefs.
- Functional expression: Health behaviors, relationships, role fulfillment, and coping response quality.
- Discrepancy-linked risk signals: Body-image distress with mood decline, obsessive appearance focus, and disordered eating patterns.
Nursing Assessment
NCLEX Focus
Assess self-concept using both patient language and function-based evidence, not labels alone.
- Assess perceived strengths, limitations, and identity statements across personal, family, and social roles.
- Assess body-image concerns and emotional impact on mood, adherence, and participation.
- Assess for depression, anxiety, and suicidal ideation when body dissatisfaction is persistent or escalating.
- Assess “should/must” self-talk and conflict between personal values and perceived external expectations.
- Assess which discrepancy pattern is most active (ideal, external expectation, or duty mismatch) and the linked emotional response.
- Assess for false-self signals, including chronic approval-seeking, overconformity, and concealment of authentic needs.
- Assess social-comparison direction (upward versus downward), trigger context, and functional impact on mood, adherence, and goal engagement.
- In pediatric contexts, assess age-appropriate self-concept cues (emerging self-recognition, self-descriptions, and response to caregiver/peer feedback).
- In school-age children, assess whether academic/sports/social feedback is being interpreted as global self-worth rather than domain-specific performance.
- Assess self-esteem pattern (stable versus situationally threatened) during illness or transition.
- Assess role performance changes and whether these changes feel meaningful, burdensome, or identity-threatening.
Nursing Interventions
- Use therapeutic communication to validate distress while reinforcing realistic strengths and progress.
- Support goal setting that closes harmful self-discrepancies through achievable, patient-defined steps.
- Map discrepancy type to tailored coping support (for example guilt-focused self-compassion work versus shame-focused relational safety work).
- Promote autonomy and shared decision-making to strengthen agency and role confidence.
- Coach authenticity-preserving boundary setting when external expectations conflict with patient values or capacity.
- Use strengths-based progress framing to reduce harmful peer benchmarking and re-anchor goals to patient-specific trajectories.
- Use targeted, domain-specific encouragement to prevent globalized “I am bad at everything” beliefs after single-domain failures.
- Coordinate interdisciplinary referrals when self-concept disturbance significantly impairs function.
- Escalate for specialized mental-health evaluation when obsessive appearance concerns or eating-disorder cues emerge.
Identity-Disruption Risk
Persistent self-concept disturbance can reduce treatment engagement and worsen psychosocial outcomes.
Pharmacology
Pharmacology does not directly treat self-concept, but medication side effects (for example weight change, sedation, sexual dysfunction, cognitive dulling) can worsen body image and self-esteem and should be proactively monitored.
Clinical Judgment Application
Clinical Scenario
A patient with new functional limitations after injury says, “I am useless now” and withdraws from rehabilitation.
- Recognize Cues: Global negative self-labeling, role-loss language, treatment disengagement.
- Analyze Cues: Self-concept disruption is now affecting recovery behavior.
- Prioritize Hypotheses: Priority is restoring agency and functional participation.
- Generate Solutions: Reframe goals around meaningful role restoration with incremental wins.
- Take Action: Implement strengths-based coaching and coordinate psychosocial support.
- Evaluate Outcomes: Improved participation, adaptive self-statements, and functional progress.
Related Concepts
- self-concept-measurement-and-clinical-assessment-tools - Structured approaches to assess self-perception patterns.
- factors-affecting-self-concept-across-health-and-culture - Upstream drivers of self-concept change.
- nursing-support-for-self-concept-role-transition-and-coping - Care strategies for disrupted self-concept.
- person-and-family-centered-care - Aligns care plans with identity and values.
- stress-and-anxiety - Common amplifiers of negative self-appraisal.
- humanistic-theories-and-therapies - Congruence and authenticity lens for person-centered care.
- eating-disorder-risk-factors - High-risk pathway when body-image distress drives unsafe behavior.
Self-Check
- How do ideal-self and ought-self discrepancies differently affect emotional response?
- How can reflected appraisal from significant others strengthen or destabilize self-concept?
- Which lifespan transitions most commonly destabilize self-concept?
- Why does role performance assessment matter in psychosocial nursing care?