Cesarean Section
Key Points
- Cesarean birth is delivery through a uterine incision when vaginal birth is unsafe or unlikely to succeed.
- Current cesarean rates in many settings are roughly one-quarter to one-third of births, with dystocia as a leading indication.
- Common indications include dystocia, fetal compromise, placental/cord complications, and selected maternal comorbid conditions.
- Planned cases commonly use regional anesthesia, while urgent emergencies may require general anesthesia for rapid delivery.
- Nursing priorities include patient education, surgical readiness, fetal surveillance, and postpartum bonding support.
Pathophysiology
Cesarean birth bypasses the vaginal route when maternal, fetal, placental, or cord factors make labor continuation high risk. Surgical delivery is used electively for anticipated risk or emergently when intrapartum deterioration threatens maternal-fetal safety.
Underlying drivers include impaired labor mechanics, uteroplacental compromise, and conditions with hemorrhage or hypoxia potential. Nursing care must maintain physiologic stability, procedural safety, and informed, patient-centered communication during rapid transitions.
Classification
- Planned cesarean: Scheduled for known risk (for example, multiple gestation, large-for-gestational-age fetus, active HSV lesions, HIV, persistent malpresentation, placenta previa, or prior cesarean context).
- Unplanned/emergency cesarean: Triggered by intrapartum complications such as fetal distress or labor arrest.
- Repeat-cesarean/VBAC decision pathway: Candidate-specific risk-benefit counseling and continuous intrapartum surveillance.
- Incision profile: Low transverse incision is most common and more compatible with future VBAC; classical vertical incision carries higher later uterine-rupture risk.
- Cord/placental-risk pathway: Velamentous insertion, vasa previa, placenta previa, placental abruption, uteroplacental insufficiency, and placenta accreta-spectrum complications can require cesarean to reduce hemorrhage/hypoxia risk.
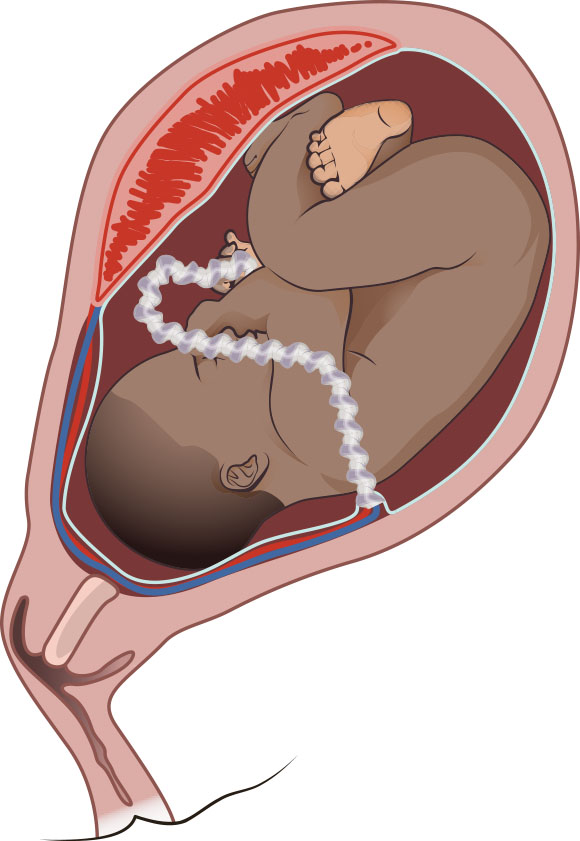 Illustration reference: OpenStax Maternal-Newborn Nursing Ch.19.6.
Illustration reference: OpenStax Maternal-Newborn Nursing Ch.19.6.
Maternal and fetal indication highlights:
- Planned cesarean contexts commonly include multiple gestation, macrosomia, prior cesarean, active genital HSV lesions, high-risk HIV transmission context, persistent malpresentation, and previa.
- Unplanned cesarean contexts include failed labor progression and acute maternal-fetal deterioration during labor.
- Severe fetal distress cues include severe bradycardia, absent variability, and recurrent late decelerations.
- Meconium-stained fluid alone does not automatically mandate cesarean without other distress evidence.
Nursing Assessment
NCLEX Focus
Priority questions test when urgent conversion to cesarean is needed and what nursing preparations must occur immediately.
- Identify current indication severity (maternal instability, fetal compromise, hemorrhage risk, labor failure).
- Monitor fetal status continuously and trend maternal hemodynamics pre- and intra-procedure.
- Assess anxiety, understanding, and support-person needs during plan changes.
- Verify preoperative readiness, consent status, and team coordination for neonatal support.
- Review prior uterine-incision history and uterine-scar status when evaluating VBAC candidacy and rupture risk.
- For breech counseling, distinguish planned vaginal-breech eligibility (selected criteria only) from higher-risk patterns that favor cesarean (for example incomplete breech, large fetus, oligohydramnios, pelvic contracture, prior cesarean, or prior neonatal trauma history).
- In multifetal labor, correlate presentation pattern with route planning (for example vertex-vertex often vaginally feasible, presenting breech twin more often cesarean pathway).
Nursing Interventions
- Provide concise education on rationale, expected sequence, and recovery implications.
- Optimize positioning and perfusion, avoiding full supine compression effects.
- Prepare equipment, blood-product contingency, and neonatal-resuscitation readiness when indicated.
- Support skin-to-skin, bonding, and early feeding goals whenever clinically feasible.
- Complete structured preoperative checks for scheduled cases (identity/allergy/reason verification, consent, baseline maternal-fetal assessment, IV/bolus prep, urinary catheter, SCD placement, antiseptic prep, and surgical time-out readiness).
- Anticipate anesthesia pathway differences: regional block for most planned cases, with emergency conversion to general anesthesia when immediate delivery is required.
- In immediate postoperative recovery, perform frequent head-to-toe reassessment (commonly every 15 minutes in hour 1, every 30 minutes in hour 2, then hourly) with focused checks of fundus/lochia, incision dressing, pain control, oxygenation, urine output, and IV patency.
- During cesarean positioning, avoid full supine compression and maintain left tilt/lateral displacement to reduce aortocaval compromise.
- If placenta accreta-spectrum emergency is identified intrapartum, anticipate hysterectomy and rapid blood-product escalation workflows.
- In OR/recovery bonding support, facilitate support-person presence when possible, early skin-to-skin, breastfeeding in the first hour when stable, and family-preference respectful communication.
VBAC Safety Considerations
- VBAC is most likely to succeed after one prior low transverse uterine incision and is less likely after prior cesarean for dystocia.
- Higher-risk features include prior vertical/classical incision, prior uterine rupture, additional uterine scars, or inability to provide immediate emergency cesarean capability.
- In trial-of-labor-after-cesarean contexts, continuous fetal monitoring is recommended because fetal tracing abnormality is a common early rupture cue.
- Typical stronger-candidate profile includes one prior low-transverse cesarean, term-near gestation under about 40 weeks, and estimated VBAC success likelihood around 60 to 70 percent.
- Poor-candidate features include prior classical/T incision, prior uterine rupture, transfundal uterine surgery, more than one prior cesarean, suspected macrosomia, unknown uterine-scar type, or major obesity-associated risk burden.
- Uterine-rupture risk rises with two prior cesareans (about two- to threefold compared with one prior cesarean).
- Interpregnancy interval greater than about 18 months is preferred to reduce rupture risk.
- Prior successful VBAC increases probability of VBAC success.
- Avoid prostaglandins for cervical ripening/induction in VBAC attempts; oxytocin use carries slightly higher rupture risk, while Foley-balloon ripening does not show the same increase.
- Attempt trial of labor only in facilities that can perform emergency cesarean without delay.
Scheduled Cesarean Preoperation Safety Checks
- Verify patient identity, allergies, and procedural indication.
- Confirm cesarean consent and document comorbidities/pregnancy complications.
- Record baseline maternal vital signs and fetal heart rate.
- Start IV access and fluid bolus before regional anesthesia when ordered.
- Prepare operative site, apply SCDs, and complete electrosurgery safety prep per policy.
- Insert Foley catheter and confirm fetal status immediately before procedural start.
- Perform antiseptic abdominal prep and formal time-out.
- Provide real-time support to patient and support person during transfer and setup.
Hemorrhage and Hypoxia Risk
Delays in emergency cesarean preparation during maternal-fetal deterioration can rapidly increase severe morbidity.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| anesthesia-for-labor-and-birth (anesthetic-agents) | Regional or general anesthesia context | Monitor hemodynamics closely and coordinate rapid escalation if instability occurs. |
| uterotonics | Oxytocin postpartum context | Used after birth to support uterine tone and reduce hemorrhage risk. |
Clinical Judgment Application
Clinical Scenario
A laboring patient develops persistent late decelerations and failure of descent despite corrective interventions.
- Recognize Cues: Ongoing fetal compromise with nonprogressive labor.
- Analyze Cues: Vaginal continuation is increasingly unsafe and unlikely to resolve promptly.
- Prioritize Hypotheses: Immediate priority is expedited, coordinated surgical birth preparation.
- Generate Solutions: Activate cesarean pathway, complete rapid readiness checks, and coordinate neonatal team.
- Take Action: Transfer safely, maintain monitoring, and support informed communication.
- Evaluate Outcomes: Birth occurs with stabilized maternal status and prompt neonatal assessment.
Related Concepts
- interventions-during-birth - Operative pathways often progress toward cesarean when assisted birth is not appropriate.
- labor-dystocia - Frequent indication for cesarean conversion.
- obstetrical-emergencies - Emergency scenarios may require immediate surgical delivery.
- preexisting-conditions-placing-delivery-at-risk - Comorbidity profile influences cesarean threshold.
- postpartum-hemorrhage - Post-cesarean surveillance must prioritize bleeding risk.
Self-Check
- Which intrapartum findings most strongly indicate emergency cesarean need?
- How does VBAC candidacy alter intrapartum monitoring intensity?
- Which nursing actions best preserve safety and patient-centered care during urgent cesarean transition?