Leadership Styles and Situational Use in Nursing
Key Points
- No single leadership style is optimal across all clinical situations.
- Style selection should follow acuity, team experience, urgency, and goal type.
- Autocratic style supports rapid crisis action; collaborative styles support engagement and innovation.
- Transformational, authentic, resonant, and servant styles are generally associated with higher nurse job satisfaction, while passive-avoidant and laissez-faire patterns are associated with lower satisfaction.
- Overuse of one style can reduce morale, creativity, or reliability.
- Democratic leadership uses participatory, multidirectional communication while the leader still retains final decision accountability.
- Every style has predictable tradeoffs, so leaders must weigh speed, structure, morale, and innovation demands before choosing.
Pathophysiology
Leadership style changes team cognition, communication flow, and decision speed. In time-critical events, directive leadership can reduce delay; in complex improvement work, participatory or transformational styles increase buy-in and sustainability.
Mismatch between style and context can produce avoidable friction, compliance drift, and reduced patient-safety margins.
Evidence from nursing leadership outcomes also shows that style selection influences workforce stability: relationship-centered styles improve morale and retention signals, whereas passive leadership patterns correlate with turnover pressure and weaker engagement.
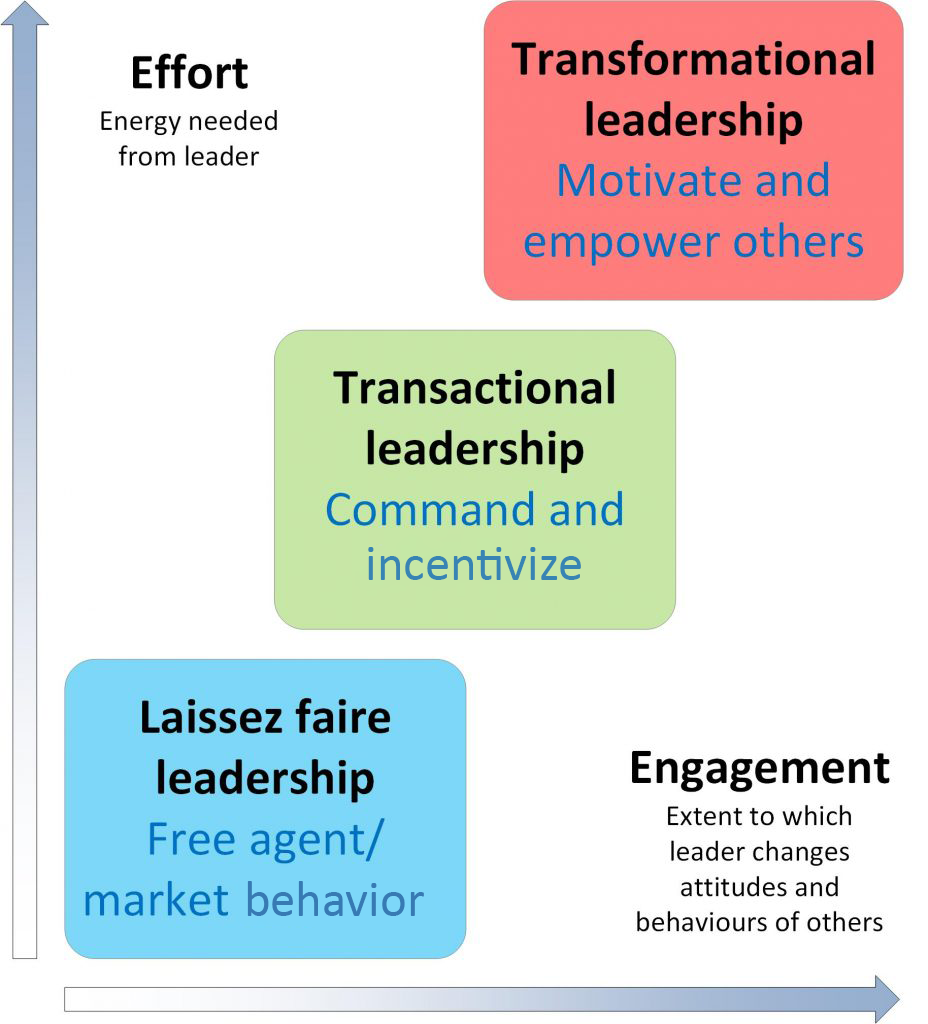 Illustration reference: OpenRN Nursing Management and Professional Concepts 2e Ch.4.2.
Illustration reference: OpenRN Nursing Management and Professional Concepts 2e Ch.4.2.
Classification
- Directive styles: Autocratic and transactional for urgency, clarity, and compliance.
- Collaborative styles: Democratic and servant for engagement and shared ownership.
- Adaptive/innovation styles: Transformational and quantum for change-intensive environments.
- Relational climate styles: Resonant and authentic for trust, transparency, and sustained commitment.
- Autonomy style: Laissez-faire for highly skilled, self-directed teams with low oversight needs.
- Avoidant risk style: Passive-avoidant leadership with delayed response and weak accountability.
- Behavior-signal profile: Autocratic uses centralized decisions and tighter control, democratic uses participatory decisions and multidirectional communication, transactional uses external rewards/penalties, transformational builds shared ownership around vision, servant centers team growth and shared decisions, and authentic leadership emphasizes transparent information sharing.
- Style tradeoff profile: Autocratic for urgent clarity but lower creativity, democratic for consensus but slower decisions, transactional for short-term compliance but weaker long-term initiative, servant for empathy/trust but weaker fit for strict time-critical protocol contexts, quantum for uncertainty adaptation but less measurable consistency.
Nursing Assessment
NCLEX Focus
Identify which style best fits the immediate unit need: speed, consensus, innovation, or strict compliance.
- Assess event urgency and patient acuity.
- Assess team experience and independence level.
- Assess whether the objective is crisis control or long-term improvement.
- Assess current morale and response to prior leadership approach.
- Assess risk of communication delay with collaborative processes.
Nursing Interventions
- Use directive commands during emergencies, then debrief collaboratively.
- Use democratic input for protocol redesign and workflow optimization.
- Use transformational framing for culture and quality initiatives.
- Use resonant and authentic behaviors (empathy, transparency, and trust-building) when rebuilding morale.
- Distinguish leadership and management functions in real time (vision/change influence vs staffing/resource execution) to prevent role-blur delays.
- Use transactional reinforcement for high-compliance safety tasks.
- Use servant leadership behaviors to strengthen trust and belonging when team cohesion is the primary need.
- Use quantum leadership behaviors when uncertainty is high and rapid adaptation is required, then add structure as conditions stabilize.
- Avoid passive-avoidant leadership in unstable units because delayed corrective action increases operational risk.
- Reassess style fit as patient and operational conditions change.
Style Rigidity
Using one preferred style in every scenario can undermine safety or team performance.
Pharmacology
Medication safety operations often need transactional clarity for compliance while benefiting from transformational culture-building to sustain safe habits.
Clinical Judgment Application
Clinical Scenario
A unit faces a code event followed by recurring hand-hygiene noncompliance trends.
- Recognize Cues: Crisis response and long-term behavior change require different leadership approaches.
- Analyze Cues: One style will not solve both problems effectively.
- Prioritize Hypotheses: Directive leadership first, then collaborative improvement.
- Generate Solutions: Command-based code management plus post-event team QI planning.
- Take Action: Shift from autocratic to democratic/transformational mode after stabilization.
- Evaluate Outcomes: Faster crisis execution and improved sustained compliance.
Related Concepts
- leadership-attributes-and-competencies-in-nursing - Competencies guide style adaptation.
- quality-improvement-nurse-role-and-qapi - Style choice influences QI adoption.
- evidence-based-decision-making-in-nursing - Collaborative styles support evidence uptake.
- employee-engagement-skills-in-nursing-management - Style climate strongly influences morale, engagement, and retention.
Self-Check
- Which style is safest during immediate life-threatening deterioration?
- Why is democratic leadership less practical during emergencies?
- How can style transitions improve both outcomes and team morale?