Factors Influencing the Process of Labor and Birth
Pathophysiology
Labor progression is determined by the interaction of the five Ps: power (uterine/pushing force), passage (bony and soft tissues), passenger (fetal size, lie, attitude, position), position (maternal movement/posture), and psyche (fear, coping, support). Small changes in one domain can accelerate or hinder labor. Labor initiation appears to be a coordinated maternal-fetal-placental process. Commonly described contributors include uterine stretch, relative progesterone withdrawal with estrogen dominance, oxytocin responsiveness, placental corticotropin-releasing hormone increase near term, and fetal cortisol-linked maturation signaling. Psychologic perception of safety versus danger can further influence labor physiology. Within the power domain, myometrial contractions and interval retraction work together: contraction waves increase downward pressure for effacement/dilation/descent, and fiber retraction during rest intervals limits fetal backsliding between contractions.
- Power includes contraction quality and pushing effectiveness; contraction assessment commonly tracks duration, intensity, and frequency. Second-stage expulsive power is further shaped by pushing coordination, epidural-related urge sensation changes, fetal orientation, and contraction support.
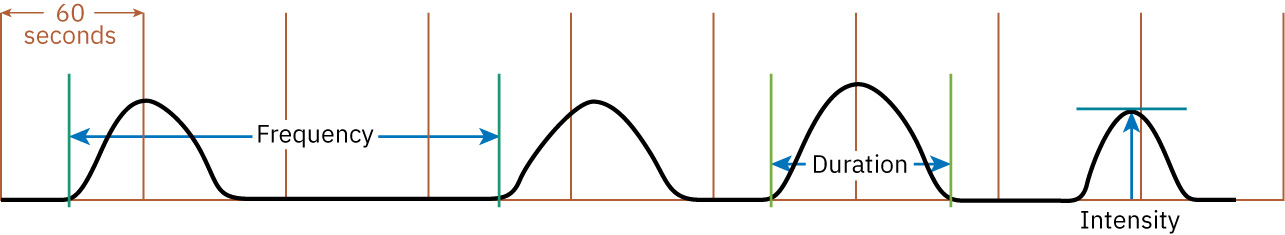 Illustration reference: OpenStax Maternal-Newborn Nursing Ch.15.1.
Illustration reference: OpenStax Maternal-Newborn Nursing Ch.15.1.
- Passageway includes pelvic bony architecture and pelvic-floor soft tissue behavior that can support or hinder fetal descent. Relaxin-related ligament softening and pelvic-floor condition can change functional passage dynamics during labor. Both pelvic-floor weakness and excessive resistance can contribute to malposition or dysfunctional labor patterns.
- Passenger includes fetal skull molding, lie, presentation, attitude, position, and station. Unfused sutures and fontanelles allow fetal-head molding that helps adaptation through inlet, midpelvis, and outlet diameters. Most term fetuses are longitudinal; persistent transverse lie at term is typically incompatible with vaginal birth, while oblique lie may convert in labor but can delay progress when cervical pressure is ineffective.
- Positioning affects fetal rotation/descent and maternal-fetal perfusion during labor.
- Psyche influences coping, catecholamine burden, and effective participation in labor. Birth hormones generally function best in calm, low-stimulation conditions; fear, anxiety, and perceived threat can counter physiologic labor progress. Pelvic-shape labels (for example gynecoid/android/anthropoid/platypelloid) may still appear in clinical language, but they have limited independent predictive value for birth outcomes and should not drive deterministic counseling.
Impending Labor Cue Domains
- Contraction domain: Progression from irregular prodromal activity to stronger, regular contractions.
- Cervical-change domain: Dilation, effacement, softening, and anterior movement as labor approaches.
- Descent domain: Lightening with increased pelvic pressure and easier diaphragmatic breathing sensation.
- Membrane/discharge domain: ROM patterns and mucus-plug/leukorrhea changes requiring triage differentiation.
- Behavior/energy domain: Short-lived increased energy (“nesting”) versus persistent overactivity needing mental-health screening.
Nursing Assessment
- Evaluate contraction pattern, cervical change, and fetal descent trend.
- Use contraction descriptors systematically (duration, intensity, frequency, and interval) and correlate with cervical change/descent.
- In suspected active labor, correlate strong contractions around every 2 to 3 minutes lasting about 60 to 70 seconds with cervical-change trend.
- If labor status is unclear, reassess cervical change after an observation interval (commonly about 1 to 4 hours) before final triage disposition.
- Assess fetal lie/presentation/position and response to positional interventions.
- Track effacement (0% to 100%), dilation (0 to 10 cm), and station (-5 to +5; engagement at 0 station).
- During slow labor or fetal-heart-rate changes, reassess current maternal position first and identify the next position strategy rather than maintaining static posture.
- Screen for maternal fatigue, fear, pain coping, and support adequacy.
- Identify warning signs requiring escalation (bleeding, fetal movement change, severe headache, rupture concerns).
- Differentiate impending/prodromal cues (for example, lightening, cervical ripening, irregular Braxton-Hicks contractions) from true labor progression.
- For possible membrane rupture, assess and document fluid time, color, amount, and odor and escalate abnormal findings.
- Use ROM workflow elements when indicated: pooling assessment, pH/nitrazine context, and ferning microscopy or speculum-assisted confirmation per policy/training.
- When commercial membrane tests are used, interpret with method-specific performance limits (for example high sensitivity but imperfect specificity) and reconcile results with clinical findings.
- Review urgent warning signs in late pregnancy triage, including heavy bleeding, fetal-movement reduction (for example under 10 in 2 hours), and preeclampsia symptom cluster.
Nursing Interventions
- Promote mobility and frequent position changes to support rotation/descent.
- Prioritize upright and dynamic movement when safe; prolonged static positioning can reduce rotational progress and worsen dysfunctional labor trends.
- Provide comfort and hydration while monitoring progression objectively.
- Reinforce education on true-labor versus prodromal signs.
- Escalate promptly for dysfunctional labor patterns or safety concerns.
- Teach return/call thresholds for suspected true labor (regular contractions that become closer/stronger and do not resolve with rest or position change).
- Align supportive care with the active limiting factor (power, passageway, passenger, positioning, or psyche) instead of applying a single generic intervention pathway.
- For prodromal discomfort, apply practical measures such as oral hydration, bladder emptying, bowel-support habits, rest, hydrotherapy, and heat/ice options when safe.
- For pelvic-pressure and lightening discomfort, coach supportive movement options (for example hands-and-knees, knee-chest, pelvic tilts, and gentle asymmetric gait walking) based on patient tolerance.
- If triage criteria for active labor are not met, provide explicit labor precautions and follow-up timing before discharge.
- For persistent non-longitudinal lie near term, coordinate evaluation for correction options (for example ECV when appropriate) and parallel operative-birth contingency planning.
- With neuraxial analgesia, protect patient and staff body mechanics and rotate through supported options (left/right side-lying, hands-and-knees, squatting variants, high Fowler with asymmetric legs/peanut-ball support, and supported upright postures when permitted).
- Avoid prolonged high-hip-flexion lithotomy when possible because extended static use is associated with pelvic-floor and musculoskeletal injury risk.
- Build a low-stimulation coping environment when feasible (dim/quiet setting, preferred sound, comfort items, and chosen support persons) to support labor physiology and reduce stress burden.
Clinical Judgment Application
Clinical Scenario
A term patient reports painful contractions every 5 minutes for 1 hour, but initial cervical findings are unchanged from a repeat assessment interval.
- Recognize Cues: Symptomatic contractions with limited short-interval cervical progression.
- Analyze Cues: Current findings fit prodromal or early latent pattern rather than established active labor.
- Prioritize Hypotheses: Priority is safe disposition with clear return criteria and continued maternal-fetal reassurance.
- Generate Solutions: Reassess fetal status, review ROM and warning-sign screen, and provide comfort plus explicit labor-precaution teaching.
- Take Action: Document findings, communicate plan, and discharge only when stability and understanding are confirmed.
- Evaluate Outcomes: Patient can state return triggers accurately and re-presents promptly if progression occurs.