Amniotic Fluid Embolism
Key Points
- Amniotic fluid embolism (AFE) is a rare, high-fatality obstetric emergency that usually occurs during labor, delivery, or shortly after birth.
- AFE can cause abrupt hypoxia, severe dyspnea, hypotension, shock, dysrhythmia, seizure, and cardiac arrest.
- Consumptive coagulopathy (DIC) with severe hemorrhage can develop rapidly and requires immediate blood-component support.
- Maternal stabilization and expedited delivery planning are simultaneous priorities.
- Time-critical multidisciplinary response is essential (airway, circulation, transfusion, and operative readiness).
- Reported incidence is roughly 1 in 80,000 to 1 in 20,000 pregnancies, and mortality remains high.
Pathophysiology
AFE occurs when amniotic fluid and fetal material enter maternal circulation through a disruption between the amniotic compartment and maternal venous system. The syndrome behaves like abrupt inflammatory and immunologic dysregulation (cytokine-mediated response) rather than a simple mechanical embolus.
Rapid cardiopulmonary instability can be followed by disseminated coagulation failure, causing both thrombosis and life-threatening hemorrhage. Maternal collapse also impairs uteroplacental perfusion, increasing fetal hypoxemia and acidosis risk.
Classification
- Initial cardiopulmonary phase: Sudden respiratory distress, hypoxia, hypotension, dysrhythmia, seizure, or arrest.
- Coagulopathic hemorrhagic phase: DIC with heavy bleeding requiring balanced blood-component resuscitation.
- Peridelivery timing window: Most events occur during labor/delivery or within about 30 minutes postpartum.
Common Risk Contexts
- Multiparity
- Advanced maternal age
- Tachysystole or uterotonic exposure
- Cesarean birth
- Uterine rupture or uterine trauma
- Placental abruption
- Intrauterine fetal demise
Nursing Assessment
NCLEX Focus
Treat abrupt respiratory or hemodynamic collapse in labor/postpartum as an arrest-level obstetric emergency until proven otherwise.
- Assess for abrupt severe dyspnea, hypoxia/cyanosis, pulmonary edema pattern, hypotension, dysrhythmia, seizure, or altered mental status.
- Recognize possible prodromal cues such as sudden sense of doom, chills, nausea/vomiting, agitation, or anxiety.
- Assess fetal status continuously because maternal collapse rapidly worsens fetal oxygenation and acid-base status.
- Assess for early coagulopathy/hemorrhage signs and trend clotting support requirements.
- Track shock progression and organ-perfusion endpoints during resuscitation.
- In survivors, monitor for neurologic sequelae (for example seizure recurrence, persistent confusion, or coma-level impairment) during critical-care transitions.
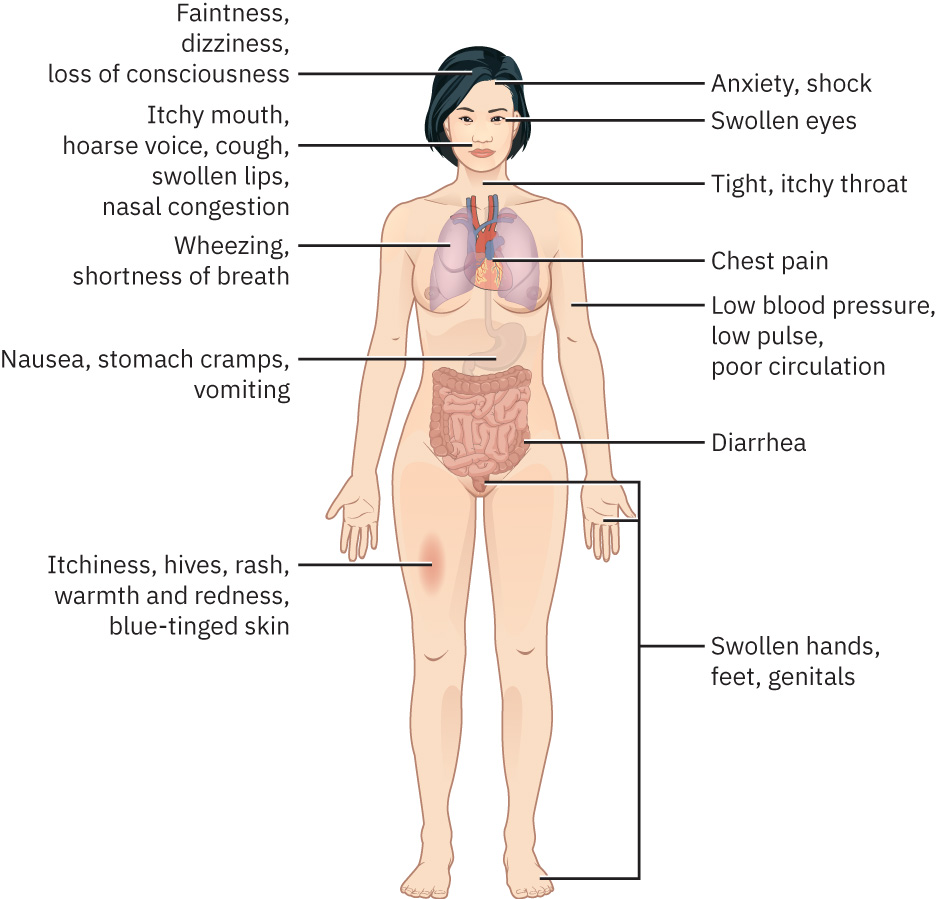 Illustration reference: OpenStax Maternal-Newborn Nursing Ch.21.2.
Illustration reference: OpenStax Maternal-Newborn Nursing Ch.21.2.
Nursing Interventions
- Activate obstetric emergency and arrest-level response immediately.
- Support airway and breathing (high-flow oxygen, prepare intubation/mechanical ventilation).
- Initiate hemodynamic resuscitation with IV fluids, vasopressors/inotropes as ordered, and continuous reassessment.
- Prepare rapid blood-component support in the operating room (PRBC, FFP, platelets, cryoprecipitate) for coagulopathy and hemorrhage.
- Coordinate urgent cesarean delivery pathway when maternal-fetal condition requires expedited birth.
- Anticipate CPR and advanced cardiac life support workflows when cardiac arrest occurs.
Maternal-Fetal Catastrophic Deterioration
AFE can progress within minutes from respiratory distress to shock, coagulopathy, and arrest; delayed escalation markedly increases mortality.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| blood-transfusion-verification-initiation-and-reaction-response (blood-products) | PRBC, FFP, platelets, cryoprecipitate | Prepare immediate availability for AFE-associated coagulopathy and hemorrhage. |
| vasopressors | Norepinephrine and related titrated agents | Use for persistent hypotension/shock with close hemodynamic monitoring. |
| antifibrinolytics | TXA emergency context | May be used in severe hemorrhagic pathways per obstetric critical-care protocol. |
Clinical Judgment Application
Clinical Scenario
During active labor, a patient abruptly develops severe dyspnea, oxygen desaturation, hypotension, agitation, and then heavy bleeding with worsening fetal heart tracing.
- Recognize Cues: Sudden cardiopulmonary collapse plus emerging coagulopathy in intrapartum setting.
- Analyze Cues: Findings are consistent with possible amniotic fluid embolism and impending maternal-fetal catastrophe.
- Prioritize Hypotheses: First priority is maternal airway-circulation stabilization with simultaneous fetal rescue planning.
- Generate Solutions: Activate code-level obstetric response, begin resuscitation, and prepare emergency operative delivery and blood products.
- Take Action: Execute protocolized team response with continuous reassessment and time-critical communication.
- Evaluate Outcomes: Perfusion/oxygenation trends improve and definitive delivery/hemostatic control proceeds.
Related Concepts
- obstetrical-emergencies - AFE is a core arrest-level intrapartum emergency.
- disseminated-intravascular-coagulation-in-pregnancy - Coagulopathy progression is a major mortality pathway in AFE.
- maternal-mortality-and-prenatal-care-access - AFE is an important U.S. pregnancy-related death contributor.
- postpartum-hemorrhage - Massive bleeding support pathways overlap with AFE coagulopathic hemorrhage management.
Self-Check
- Which abrupt maternal findings should make AFE an immediate high-priority hypothesis?
- Why must blood products be prepared early in suspected AFE?
- How are maternal stabilization and expedited delivery planning coordinated in AFE?