Vital Sign Indicators of Physiologic Functioning and Homeostasis
Key Points
- Vital signs are interdependent markers of physiologic balance and early deterioration.
- Interpretation should combine normal ranges, age variation, baseline trend, and current context.
- Pain is commonly assessed with vital signs because it can shift heart rate, respiratory pattern, and blood pressure.
- Nurses should recheck and validate unexpected readings before acting on a single abnormal value.
- Early-warning frameworks (for example MEWS with consciousness scoring) support timely escalation decisions.
- Combined vital-sign patterns provide a practical snapshot of circulatory, respiratory, and neurologic status.
- In older adults, baseline temperature may run lower, so high-normal readings can still indicate clinically important infection.
Pathophysiology
Homeostasis is the body’s self-regulation process across temperature control, oxygenation, circulation, and ventilation. Vital signs are bedside indicators of whether that regulation is stable or threatened. Central autonomic control (including medulla-oblongata pathways) and peripheral chemo/baroreceptor feedback loops (for example carotid and renal pathways) continuously shape these vital-sign trends.
A change in one vital sign can cause compensatory changes in others. For example, pain or anxiety may increase pulse and blood pressure, while hypoxemia may increase respiratory effort and heart rate before late desaturation appears. Hypoxemia refers to reduced oxygen in arterial blood, while hypoxia refers to inadequate oxygen delivery at the tissue level; prolonged deficits can cause ischemic injury in oxygen-sensitive organs. Because abnormal vital signs are not specific to pain, interpretation should be paired with subjective report and behavioral findings; post-intervention normalization supports analgesic effect but does not confirm pain as the only cause. In thermoregulation, hypothalamic control drives vasodilation/sweating for heat loss and shivering for heat generation; circadian and metabolic variation should be considered before labeling minor temperature shifts as pathologic.
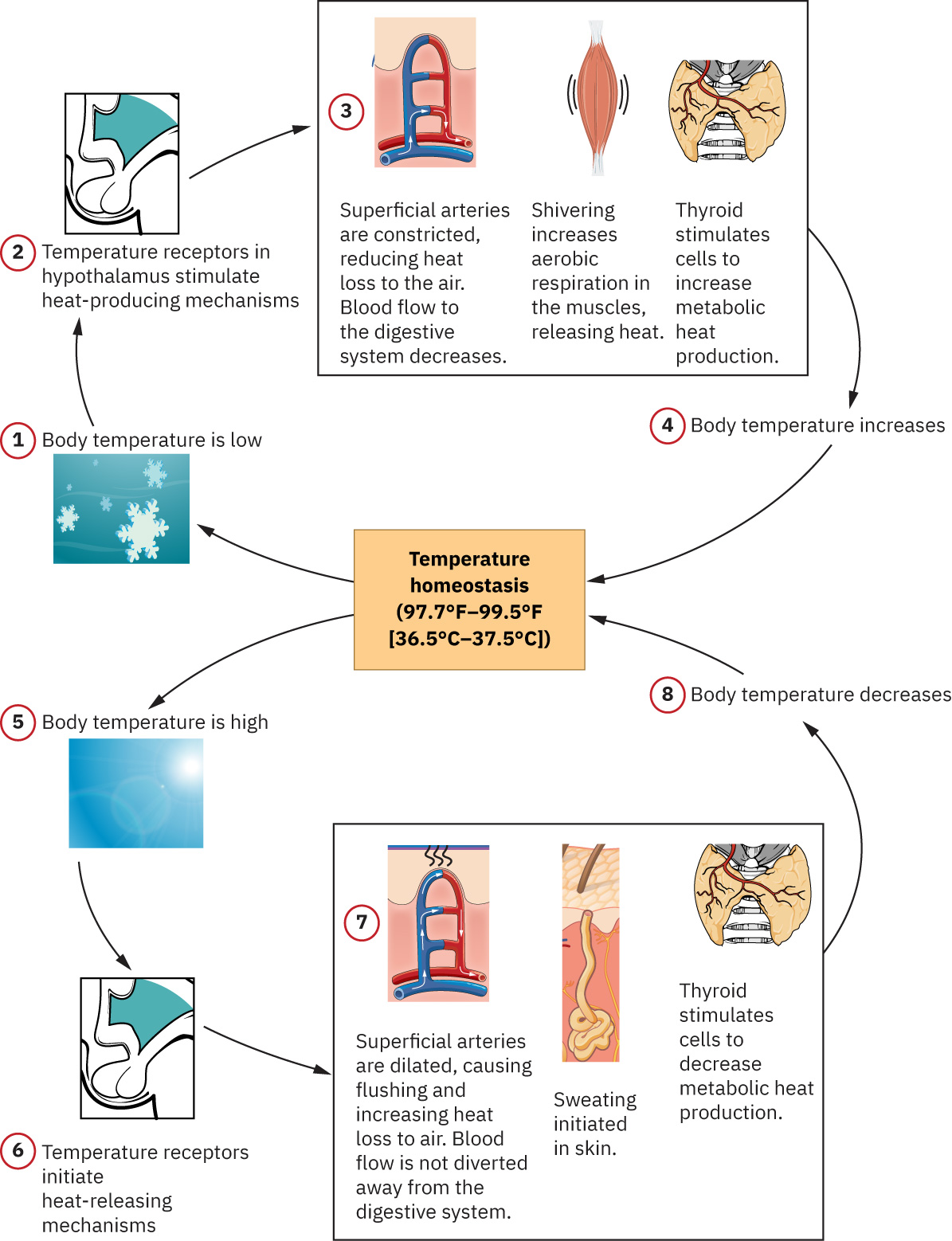 Illustration reference: OpenStax Fundamentals of Nursing Ch.7.1.
Illustration reference: OpenStax Fundamentals of Nursing Ch.7.1.
Severe temperature extremes should be interpreted as high-risk instability: core temperature above 105.8 F (41 C) suggests hyperthermia and below 95 F (35 C) suggests hypothermia, often from external exposure stressors rather than routine circadian fluctuation.
A temperature above 100.4 F (38 C) is pyrexia (fever); a patient with fever is febrile, and return to normal range is afebrile status.
Hormonal transitions (for example menopause-related estrogen change) can alter thermoregulatory sensitivity and perceived temperature instability.
For pulse interpretation, cardiac output is defined as CO = SV x HR (stroke volume times heart rate). When stroke volume is strong (for example trained athletes), resting heart rate may be lower while maintaining adequate output. At the other extreme, severe tachycardia can reduce ventricular filling time, lower stroke volume, and eventually reduce effective cardiac output despite a fast pulse.
Respiratory pattern also reflects acid-base compensation: nonpulmonary acidosis often drives tachypnea/hyperventilation to eliminate CO2, while nonpulmonary alkalosis may present with hypoventilation/bradypnea.
Blood pressure trends reflect interaction of cardiac contractility, vascular tone/diameter, and circulating blood volume; abrupt hypotension with tachycardia should trigger evaluation for shock physiology.
Pulse pressure (systolic minus diastolic) and mean arterial pressure (MAP) add perfusion context; sustained MAP below about 60 mmHg increases ischemia risk from inadequate tissue blood flow.
Heat exchange with the environment occurs through four practical pathways that influence bedside temperature trends and comfort interventions:
- Conduction: Direct contact transfer (for example ice packs, tepid sponge contact, cooling blankets), typically a small fraction of total heat loss.
- Convection: Air or water current transfer (for example fan, wind exposure, conditioned airflow), which can accelerate heat loss in exposed patients.
- Radiation: Infrared-wave transfer without direct contact (for example sun exposure, radiant warmers, room heat sources), often the largest passive transfer component.
- Evaporation: Heat loss when water turns to vapor (for example perspiration), strongly affected by ambient humidity.
Classification
- Thermoregulatory indicators: Temperature and fever/hypothermia patterns.
- Perfusion indicators: Pulse rate/rhythm/force and blood pressure trends.
- Ventilation and oxygenation indicators: Respiratory rate/quality and SpO2 trend.
- Integrated distress indicators: Pain and symptom context affecting all domains.
- Consciousness-status indicators: AVPU/GCS-linked arousal and response trends that modify deterioration risk.
- Escalation-score class: Modified Early Warning Score (MEWS) combines vital signs and consciousness cues to trigger response tiering.
Nursing Assessment
NCLEX Focus
Priority decisions emphasize trend interpretation and immediate verification of unexpected abnormalities.
- Assess each vital sign with route/method accuracy and standardized timing.
- Use contextual SpO2 targets: most adults
94-98%; selected chronic-hypercapnic profiles (for example some COPD patients) may use lower ordered targets such as88-92%. - Verify equipment size and configuration are appropriate for the patient (especially BP cuff sizing and sensor fit).
- Review prior trends, clinical history, and ordered monitoring parameters before interpretation.
- Compare findings to age-specific ranges and patient baseline.
- In pediatric workflows, anticipate routine blood-pressure screening from about age 3 (earlier with cardiac-risk concerns) and interpret pediatric BP by age, height, and sex-specific norms.
- Assess context factors such as activity, pain, anxiety, medications, and environment.
- Assess required monitoring cadence by setting and acuity (for example routine acute-care intervals, high-frequency critical-care surveillance, outpatient visit-based checks, or long-term-care daily/as-needed schedules).
- Assess exposure risks that amplify heat loss or gain (for example inadequate clothing in cold/windy settings, high ambient heat, prolonged wet skin).
- Interpret pulse across
rate,rhythm, andvolumecharacteristics, not rate alone. - Assess pulse equality between sides when clinically indicated and avoid simultaneous bilateral carotid palpation.
- In neonates, especially preterm infants, treat low temperature as high risk because immature shivering response and limited brown-fat reserve reduce heat-generation capacity.
- For older adults, monitor mental-status change (confusion, disorientation, agitation) as a potential temperature-related deterioration cue.
- Account for menstrual-cycle timing, exercise load, and emotional arousal when interpreting mild temperature elevation.
- Link pulse abnormalities with likely physiologic drivers such as fever/hyperthyroidism, hypoxemia, hypovolemia, structural heart failure, and electrical-conduction disorders.
- Respect site/route limitations driven by history (for example post-mastectomy arm precautions, wound-related site exclusions, oral-route contraindications).
- Assess for concerning pattern combinations (for example hypotension with tachycardia).
- Track respiratory pattern quality (rate, rhythm, depth) and identify high-risk abnormalities such as apnea episodes, Kussmaul pattern, or Cheyne-Stokes cycles.
- In newborns and infants, count respirations for a full minute while calm; newborn respiratory rate commonly ranges about
30-60/minand varies with sleep-wake state. - In infants who are obligate nose breathers, assess nasal patency because congestion or occlusion can rapidly worsen respiratory distress.
- Treat dyspnea with accessory-muscle use, tripod posture, or orthopnea as escalation cues for possible respiratory or cardiopulmonary decompensation.
- Use pediatric oxygen-saturation expectations of about
95-100%in most children unless an alternate target is specifically ordered. - Assess whether a reading may be technical artifact and requires repeat measurement.
- Recognize pulse-oximetry limitations in severe anemia, reduced peripheral perfusion, and dyshemoglobinemia exposure contexts (for example carbon monoxide), and escalate to confirmatory testing when readings and presentation disagree.
- When available, calculate and trend MEWS with each set of abnormal vital signs or neurologic concern.
- Integrate level-of-consciousness findings (A&O status, AVPU, or GCS) with physiologic readings rather than interpreting vitals in isolation.
Nursing Interventions
- Recheck abnormal values using correct technique and alternate method/site when needed.
- Validate electronically monitored values with manual assessment when readings are inconsistent with clinical presentation.
- Escalate validated high-risk changes promptly according to facility protocol.
- Prioritize urgent assessment for unexpectedly low temperatures in infection-risk patients, particularly at age extremes.
- Document value, method, context, and follow-up action clearly.
- Coordinate symptom and cause-directed interventions rather than isolated number treatment.
- Educate patients on expected ranges, warning signs, and when to notify providers.
- Treat ordered cadence as a minimum; obtain a full additional vital-sign set whenever status changes or concern is raised by patient/family/team.
- When collection is delegated, verify data quality and maintain RN accountability for interpretation and escalation decisions.
- If device malfunction is suspected, remove equipment from use, label appropriately, and route for technical/biomed evaluation.
- Use tiered MEWS response as a practical guide when adopted locally:
0-1: routine monitoring2-3: increase monitoring frequency (often q2h) and consider provider communication if persistent4-6: notify provider and increase monitoring (often hourly)>=7: activate rapid response/emergency pathway per policy
Single-Reading Error
Acting on one unvalidated outlier can delay appropriate care or trigger unnecessary intervention.
Pharmacology
Many medications alter vital signs (for example beta blockers affecting pulse and blood pressure). Trend interpretation should include current pharmacologic profile before concluding deterioration.
Clinical Judgment Application
Clinical Scenario
A patient has new shortness of breath, pale skin, tachycardia, and lower blood pressure than baseline.
- Recognize Cues: Multiple linked vital-sign changes suggest instability.
- Analyze Cues: Findings indicate possible perfusion and oxygenation compromise.
- Prioritize Hypotheses: Immediate priority is validating readings and preventing deterioration.
- Generate Solutions: Repeat vitals, reassess respiratory effort, and escalate quickly.
- Take Action: Notify provider/rapid response per protocol and initiate supportive care.
- Evaluate Outcomes: Stabilizing trend confirms intervention effectiveness.
Related Concepts
- measuring-body-temperature-multiple-routes - Route selection and technique affect temperature validity.
- measuring-radial-pulse - Pulse rate and rhythm trends support perfusion analysis.
- measuring-respirations - Respiratory quality and rate provide early compromise cues.
- measuring-blood-pressure-manual-and-automatic-methods - Accurate cuff method is essential for perfusion decisions.
- measuring-oxygen-saturation-with-pulse-oximetry - SpO2 interpretation requires artifact awareness.
Self-Check
- Why should nurses interpret vital signs as a pattern rather than isolated values?
- Which factors can produce a false abnormal reading that requires recheck?
- How can pain alter at least three other vital sign indicators?