General Survey and Anthropometric Measurement in Initial Assessment
Key Points
- Initial assessment begins with a structured general survey before focused examination.
- Anthropometric measures provide objective baseline data for nutrition, risk stratification, and trend monitoring.
- In bedside inpatient workflows, general survey includes height, weight, appearance, hygiene, behavior, and full vital signs to establish a shift/admission baseline.
- General survey starts at first contact and includes environmental sensory cues (what the nurse sees, hears, feels, and smells).
- Behavior and communication cues can reveal early hypoxia, neurologic deterioration, psychiatric distress, or pain-related instability.
- Initial visual inspection findings should guide when focused palpation or deeper exam techniques are needed.
- Observation quality and measurement technique directly affect downstream clinical decisions.
- Unexpected findings should trigger focused reassessment and escalation when clinically significant.
Pathophysiology
General survey findings reflect integrated function across neurologic, respiratory, cardiovascular, metabolic, and behavioral systems. Changes in appearance, mobility, speech, posture, or distress cues may be early signs of instability before laboratory or imaging abnormalities appear.
Anthropometric trends (for example height/weight pattern shifts) can signal fluid imbalance, malnutrition, chronic disease progression, or treatment effects. Accurate baseline measurement supports meaningful comparison over time.
Classification
- General survey domains: Appearance, behavior, level of distress, body position, gait/mobility, hygiene, and communication cues.
- General-survey continuity domain: Begins at first contact and continues throughout care interactions as new cues emerge.
- First-impression cue domains: Environmental safety/comfort, interaction quality, verbal and nonverbal communication, and observable respiratory effort.
- Physical-exam technique domain: Objective assessment methods include inspection, auscultation, palpation, and percussion.
- Anthropometric domains: Height, weight, BMI-related interpretation, and trend direction over time.
- Extended anthropometric domains: Waist/hip/limb circumference, pediatric head/chest circumference trends, and selected body-composition proxies.
- Anthropometric device matching: Standing, bed, sling, and bariatric scale options chosen by mobility status and safety requirements.
- Developmental domains: Age-expected gross/fine motor, speech/language, and social milestones.
- Cognitive-status domains: Orientation (person/place/date/time), level of consciousness terms, and structured tools such as GCS when indicated.
- Cognitive follow-up tools: Focused neurologic screening, targeted medication/substance-history questions, and structured tools (for example MMSE) when screening is abnormal.
- Instrument domains: Vital-sign tools (thermometer, stethoscope, BP cuff, pulse oximeter) and anthropometric tools (scale, height device, tape, calipers).
- BMI stratification: Underweight (<18.5), healthy range (18.5-24.9), overweight (25-29.9), obesity (>=30.0), and severe obesity (>=40.0).
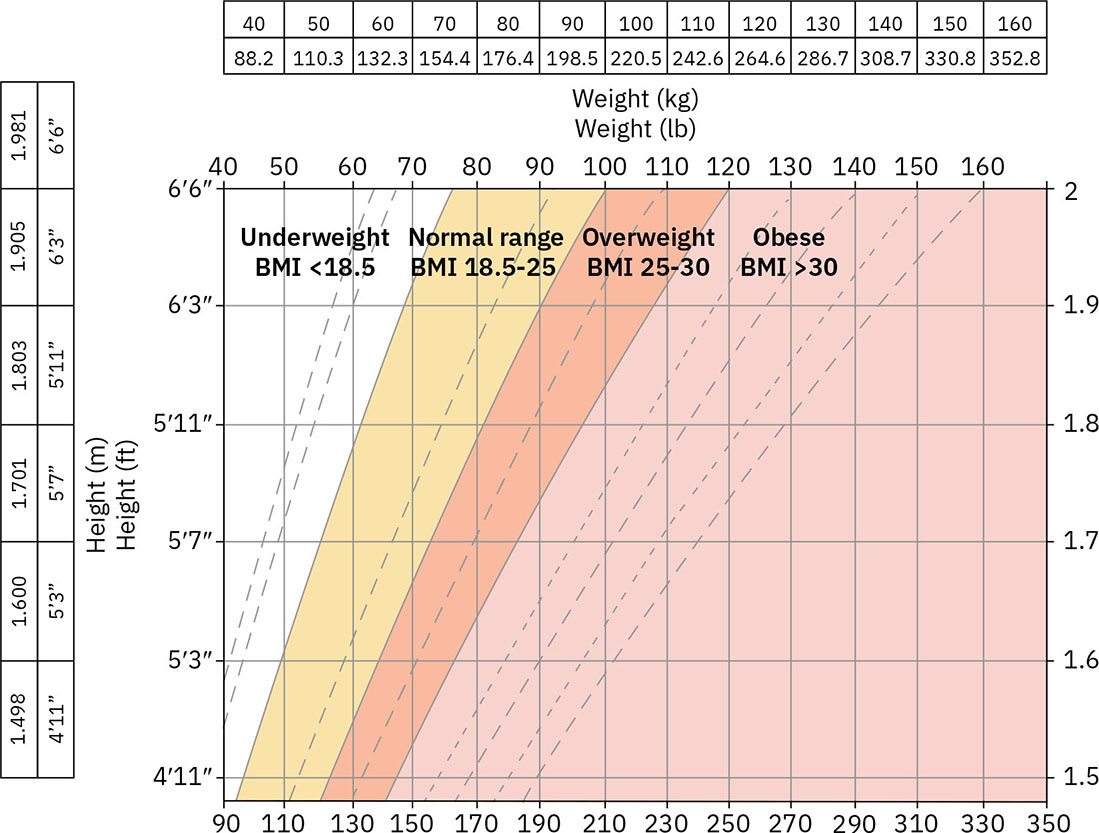 Illustration reference: OpenStax Clinical Nursing Skills Ch.15.
Illustration reference: OpenStax Clinical Nursing Skills Ch.15. - BMI interpretation limits: BMI is a screening tool and can misclassify adiposity in clients with high muscle mass, atypical body composition, and population-specific fat-distribution differences.
- BMI age context: Routine BMI computation is generally applied from about age 2 onward with age-appropriate interpretation in pediatrics.
- Clinical-use class: Baseline establishment, risk detection, and response-to-treatment monitoring.
Nursing Assessment
NCLEX Focus
Prioritize objective cue capture and trend reliability before drawing conclusions from a single isolated value.
- Conduct first-look assessment systematically and document objective descriptors rather than assumptions.
- Include room and context observations early (temperature, noise level, unusual odors, clutter/safety concerns).
- Obtain anthropometric measures using standardized technique and calibrated equipment.
- Confirm unit consistency and conversion accuracy when documenting or teaching (kg/lb and cm/in).
- Compare findings with age/context expectations and known baseline data.
- Set monitoring frequency by clinical context (single baseline at admission vs daily/weekly trend surveillance).
- Assess speech clarity, pace, and emotional tone during interaction; garbled or slurred speech requires focused neurologic follow-up.
- Assess response to simple commands because reduced comprehension or cooperation can signal acute cognitive or neurologic change.
- Assess language-access needs early and activate qualified interpreter support when language discordance is present.
- Assess communication-accommodation needs during first contact (for example interpreter pathway, hearing-aid availability, or other assistive communication supports).
- Assess behavior patterns for urgency cues: restlessness, inability to remain still, lethargy, respiratory posturing, accessory-muscle use, or new inability to ambulate.
- Reconcile verbal report with nonverbal cues (for example saying “no pain” while grimacing/guarding) before closing assessment conclusions.
- Distinguish mood from affect and document incongruence (for example flat affect or unexpectedly elated behavior in high-risk contexts) for focused mental-status follow-up.
- Interpret eye contact patterns cautiously because cultural norms can change expected nonverbal behavior.
- Assess contextual modifiers (family history, metabolic factors, activity pattern) before labeling obesity risk from BMI alone.
- Observe family interaction patterns when caregivers are present because role strain or conflict can alter care participation and ADL support reliability.
- Assess for abuse indicators (fearfulness, withdrawal, unexplained bruises/burns, inconsistent explanations) and confirm safety concerns with private interviewing when feasible.
- Assess for potential substance-use cues (for example unusually constricted or dilated pupils with atypical behavior) and escalate for focused evaluation.
- Ask directly rather than assuming biological sex or cultural preferences; integrate responses into individualized assessment planning.
- Use adjunct obesity-risk data when needed (diet pattern analysis, activity level, and other body-composition assessments).
- Identify red flags (rapid weight change, visible distress, altered mentation, severe fatigue, unstable mobility).
- Evaluate skin and mucous findings for concerning patterns: pallor, jaundice, cyanosis, flushing, abnormal moisture, and localized discoloration.
- Prioritize high-risk skin color cues at lips, mucous membranes, and sclera.
- Screen for fluid-status visual cues: dehydration patterns (dry skin, dry mucous membranes, sunken eyes) and fluid-overload patterns (peripheral edema with new breathing difficulty).
- In infants, treat a sunken fontanel with dry mucosa/skin as a high-priority dehydration cue requiring focused reassessment.
- In pediatric assessments, include head circumference through early childhood and screen developmental progression when milestones are delayed or regressing.
- In pediatric general-survey encounters, use calm/gentle communication and demonstration on dolls or stuffed animals when procedural fear may limit cooperation.
- In pediatric physical exams, document caregiver/chaperone presence and chaperone identity for sensitive breast/genital/anorectal assessment, honoring adolescent client comfort and chaperone-gender preference when feasible.
- In adolescent assessments, include private interview time for sensitive risk topics in addition to caregiver-present history.
- Document orientation as A&O x4 (person/place/date or day/time context) and note developmentally expected limits for infants/young children.
- If consciousness is reduced, classify response level (for example lethargic/obtunded/comatose) and apply structured LOC scoring as indicated.
- If screening cognition is abnormal, expand assessment with focused neurologic/mental-status follow-up (for example cranial nerve checks and MMSE-style tasks).
- In older-adult encounters, ensure glasses/hearing aids are in place, allow additional response time, and use collateral history sources when direct communication is limited.
- Escalate urgently for sudden facial asymmetry or speech change as potential stroke cues.
Nursing Interventions
- Use reproducible measurement workflow (timing, device, positioning, documentation fields).
- Start encounters with privacy setup, role-purpose-time explanation, and two-identifier verification (name/DOB plus approved secondary verification source).
- Recheck surprising values and confirm method accuracy before escalation.
- Ensure equipment is appropriately sized and matched to age/body habitus to protect measurement validity.
- Incorporate circumference measures when indicated: pediatric serial head/chest growth tracking and adult waist-centered adiposity risk assessment.
- Before beginning survey observations, address immediate readiness needs (for example pain, toileting, and sensory aids) and defer to emergency workflow if acute distress signs (for example chest pain or breathing difficulty) are present.
- If first-contact cues suggest functional limitation (poor grooming, inappropriate dress, mobility difficulty), expand assessment for ADL and support needs.
- Use inspection findings to guide focused palpation and other exam components when abnormalities need clarification.
- Use active listening plus adaptive follow-up questions when patients provide off-script concerns that may indicate hidden deterioration.
- If growth or developmental findings diverge from expected trajectory, initiate focused endocrine/neurologic and functional assessment pathways.
- Trigger focused assessments and provider notification when survey or measurement cues suggest deterioration.
- Escalate immediately for critical-condition clusters: newly unresponsive/altered mentation, breathing difficulty, out-of-range vital signs, or cool clammy cyanotic skin.
- Chart general-survey findings as expected-versus-unexpected objective statements (appearance, orientation, speech/command response, mobility/posture, skin-mucosa, anthropometrics, and full vital-sign set with oxygen context).
- Document communication-support actions used during bedside assessment (for example interpreter use or hearing-assist setup) to support continuity across handoff.
- When abuse is suspected, follow mandated-reporting workflow and agency policy without delay while maintaining patient safety.
- For communication barriers, use qualified interpreter pathways rather than ad hoc family translation for clinical decision-making discussions.
- Educate patient/caregiver on significance of trend monitoring and follow-up expectations.
- Use skinfold-caliper findings cautiously because inter-operator variability can limit consistency in routine practice.
- End encounters with a safety sweep (call light, bed low/locked, reachable table, fall-hazard scan), then perform hand hygiene and equipment decontamination before exit.
Baseline Integrity Risk
Inaccurate initial measurements or vague survey documentation can delay recognition of true clinical decline.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| diuretics | Furosemide, bumetanide | Can rapidly change weight and volume indicators; trend interpretation is essential. |
| corticosteroids | Prednisone-class agents | May alter weight distribution and fluid status over time. |
Clinical Judgment Application
Clinical Scenario
A patient appears fatigued with shallow breathing and has an unexpected weight increase compared with baseline over two days.
- Recognize Cues: Distress cues plus abnormal anthropometric trend.
- Analyze Cues: Combined findings raise concern for evolving fluid and cardiopulmonary stress.
- Prioritize Hypotheses: Immediate priority is confirming trend validity and assessing physiologic impact.
- Generate Solutions: Repeat measurement, obtain full vital signs, and perform focused respiratory/cardiovascular assessment.
- Take Action: Escalate validated concerns and implement ordered monitoring/interventions.
- Evaluate Outcomes: Early action prevents progression to severe decompensation.
Related Concepts
- vital-sign-indicators-of-physiologic-functioning-and-homeostasis - Integrates survey cues with physiologic trend interpretation.
- measuring-height-for-ambulatory-residents - Technique standards for reliable height baselines.
- measuring-weight-for-ambulatory-residents - Weight trend reliability for risk detection.
- nursing-assessment-type-selection - Choosing comprehensive vs focused reassessment.
- documenting-and-reporting-data - Objective charting supports safe escalation and continuity.
Self-Check
- Which general-survey cues should trigger immediate focused reassessment?
- Why is standardized technique essential for anthropometric trend interpretation?
- How can early trend changes alter care priority before severe vital-sign abnormalities appear?