Comprehensive Abdominal Assessment
Mahahalagang Punto
- Pinagsasama ng abdominal assessment ang focused GI at GU interview data kasama ang sequenced physical exam.
- Ginagabayan ng interview findings ang exam priorities, lalo na para sa pain, elimination changes, at urinary symptoms.
- Pinapabuti ng PQRST ang paglarawan ng abdominal pain at tumutulong ikonekta ang lokasyon sa malamang pathology.
- Pinananatili ng abdominal exam order ang bowel sound accuracy sa pamamagitan ng pagsasagawa ng auscultation bago palpation.
Patopisyolohiya
Madalas na sumasalamin ang abdominal symptoms sa dysfunction ng gastrointestinal at genitourinary structures na magkakasalo sa anatomic space at may nagsasapawang symptom patterns. Dahil maraming disorders ang may nonspecific findings, kailangang isama ng nurses ang history at exam trends upang maagang matukoy ang deterioration.
Dinisenyo ang abdominal assessment model upang mabawasan ang missed cues. Tinutukoy ng subjective findings ang malamang targets, habang kinukumpirma o hinahamon ng objective findings ang initial hypotheses. Sinusuportahan ng cyclic process na ito ang mabilis na reprioritization kapag may bagong data.
Anatomically, ang abdomen ay anterior trunk region sa pagitan ng diaphragm at pelvis. Maaaring sumalamin ang abdominal findings sa gastrointestinal at genitourinary function at maaari ring magbigay ng clues tungkol sa reproductive, metabolic, at immune system status.
Ang intra-abdominal pressure (IAP) ay dynamic pressure state na nalilikha ng interaction ng abdominal wall at viscera. Ang volume-raising conditions (halimbawa obstruction, ascites/fluid accumulation, organ inflammation, mass effect, o pagbubuntis) ay maaaring lumampas sa compensatory stretch capacity at mag-ambag sa organ dysfunction.
Dapat maagang i-screen ang risk context dahil binabago ng modifiable at nonmodifiable factors ang GI symptom burden at complication probability. Ang diet pattern, inactivity, medication effects (halimbawa iron at opioids), family history, aging physiology, at severe stress exposure ay maaaring magbago ng baseline risk bago pa lumitaw ang acute findings.
Classification
- Subjective domain: Prior diagnoses, surgeries, medications, pain pattern, bowel at urinary symptom review.
- Objective domain: Inspection, auscultation, percussion, at palpation na may quadrant-based interpretation.
- External-structure domain: Skin, superficial/transversalis fascia, abdominal wall muscles, fat, at peritoneum layers na sumusuporta sa protection, movement, thermoregulation, at organ anchoring.
- Anatomic-reference domain: Apat na abdominal quadrants na binubuo ng nagsasalubong na horizontal/vertical reference lines sa umbilicus para sa symptom localization.
- Quadrant-organ correlation domain:
- RUQ: Liver, gallbladder, right kidney (posterior), at mga bahagi ng small/large bowel.
- LUQ: Stomach, spleen, pancreas, left kidney (posterior), mga bahagi ng bowel, at bahagi ng liver.
- RLQ: Appendix, cecal/ascending colon segments, right adnexa (kung present), at upper right bladder region.
- LLQ: Descending/sigmoid colon segments, left adnexa (kung present), at upper left bladder region.
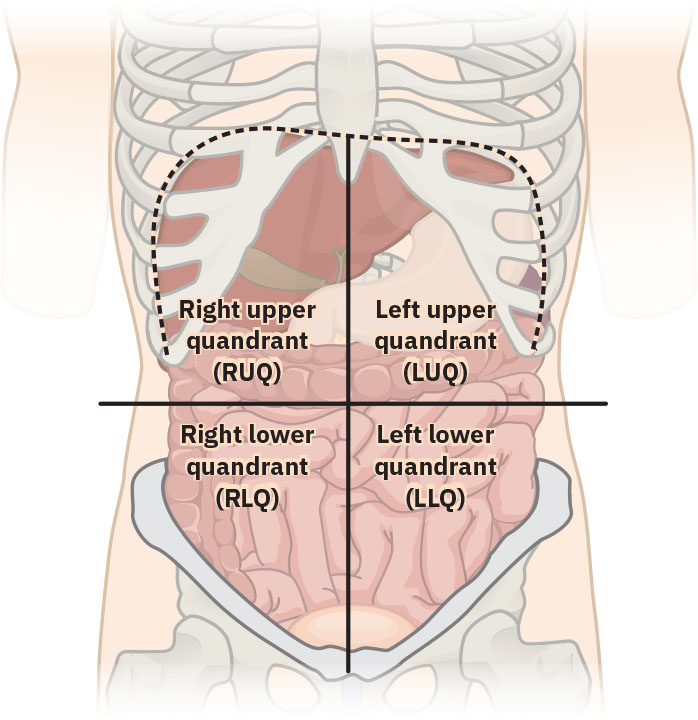 Illustration reference: OpenStax Clinical Nursing Skills Ch.27.2.
Illustration reference: OpenStax Clinical Nursing Skills Ch.27.2.
- Abdominal-wall support domain: Sinusuportahan ng rectus abdominis ang posture at anterior-organ containment; sinusuportahan ng external/internal obliques ang trunk rotation; sinusuportahan ng transversus abdominis ang trunk stability at intra-abdominal pressure regulation.
- Major abdominal-vascular landmarks: Ang abdominal aorta (primary arterial outflow sa lower systemic circulation) at inferior vena cava (major venous return mula lower body) ay key interpretation targets para sa pulsation, bruit, at instability cues.
- Viscera-type domain: Solid viscera (halimbawa liver, spleen, kidneys, pancreas, gallbladder) kumpara sa hollow viscera (halimbawa stomach, intestines, bladder); may leak-peritonitis risk ang hollow-viscera injury.
- Arterial-supply domain: Kabilang sa major abdominal perfusion branches ang celiac at mesenteric arterial pathways na nagseserbisyo sa hepatobiliary, gastric, pancreatic, at intestinal structures.
- Venous-drainage domain: Ang portal/mesenteric/hepatic/renal/gonadal venous return pathways ay nakikiintegrate sa systemic venous flow sa pamamagitan ng IVC tributary architecture.
- Functional-abdominal domain: Sumusuporta sa forced expiration/cough, bladder emptying, emesis, defecation/flatulence, at pregnancy-related abdominal wall adaptation.
- Common-impairment contributor domain: Medication effects (halimbawa opioid-constipation, antibiotic-associated diarrhea, NSAID/antacid overuse dyspepsia-reflux), poor diet/inactivity, reflux burden, at stress-related GI symptom amplification.
- Symptom-pattern domain: Colicky/wavelike, cramp-like, generalized, at localized abdominal pain descriptors kasama ang associated symptoms (bloating, nausea, anorexia, bowel-habit change, distention).
- Pain framework: PQRST (provocation, quality, region/radiation, severity, timing).
- Diagnostic-support domain: Targeted labs (CBC, CMP, albumin, thyroid function, stool studies, lipase, CRP/ESR), breath testing, genetics pathways, at imaging/endoscopy na pinipili mula sa exam cues.
Pagtatasa sa Nursing
Pokus sa NCLEX
Madalas nakadepende ang prioritization sa pagkilala sa red-flag abdominal cues at paggamit ng systematic follow-up questions.
- Magtanong ng targeted GI at GU history questions, kabilang ang prior abdominal surgery, bowel pattern changes, dysphagia, dysuria, urgency, at incontinence.
- Para sa dysuria, linawin ang internal versus external discomfort pattern at prior self-treatment attempts.
- Para sa urinary symptoms, ilarawan ang daytime-versus-nocturnal frequency, urgency na may leakage, stress incontinence triggers (ubo/bahing/exertion), at hesitancy sa pagsisimula ng stream.
- Ilarawan ang stool patterns gamit ang consistent descriptor framework (halimbawa Bristol stool forms) kapag sinusuri ang constipation o diarrhea trends.
- Mag-screen ng cultural influences sa symptom expression at dietary practices, kabilang ang preferred terminology, family support structure, at complementary-treatment use.
- Mag-screen ng socioeconomic barriers na nakaaapekto sa GI outcomes, tulad ng food insecurity, medication affordability, access sa screening procedures, at oral-health access para sa chewing/intake.
- Magtanong ng focused bleeding at elimination safety questions, kabilang ang hematochezia, melena, hematemesis, abdominal distention, recent bowel movement timing, at flatus passage.
- Magtanong ng associated symptom questions para sa bloating/fullness, nausea/pagsusuka, appetite loss (anorexia), at stool-habit change upang mapino ang differential direction.
- Para sa diarrhea-focused history, idokumento ang watery versus formed stool pattern at 24-hour episode count upang gabayan ang dehydration/infectious-workup priorities.
- Linawin ang stool quality details sa interview: color, consistency, caliber, odor, mucus, at undigested-food patterns upang ihiwalay ang expected variation mula sa alarm findings.
- Ituring ang black/red stool, persistent white stool, recurrent watery stool, hard pellet stool, o progressively narrow stool caliber bilang escalation cues sa buong clinical context.
- Ituring ang bagong bright red rectal bleeding o bagong melena bilang urgent provider-notification findings dahil parehong maaaring magpahiwatig ng clinically significant GI bleeding.
- I-escalate ang persistent o high-risk emesis patterns (halimbawa pagsusuka lampas 24 oras, dugo sa emesis, severe pain, o dehydration signs) para sa urgent provider reassessment.
- Ituring ang bloody stool, hematemesis, new/worsening melena, o dehydration na may oliguria (halimbawa urine output na mas mababa sa humigit-kumulang 30 mL/hour) bilang critical findings na nangangailangan ng immediate escalation.
- Mag-screen ng swallowing safety sa clients na may history ng stroke o TIA at i-monitor ang pill/liquid/food tolerance upang mabawasan ang aspiration-pneumonia risk.
- Gamitin ang komprehensibong pagtatasa at dokumentasyon ng sakit kasama ang PQRST para sa abdominal pain, at i-map ang findings sa quadrants.
- Linawin nang tahasan ang pain descriptors (colicky, cramp-like, generalized, localized) dahil bawat pattern ay nagbabago ng urgency at malamang source interpretation.
- Gamitin nang consistent ang quadrant localization kapag nagdodokumento ng pain, tenderness, masses, o distention upang suportahan ang differential narrowing at handoff clarity.
- Ihanda para sa exam accuracy sa pamamagitan ng pagtataguyod ng comfort (warm room/stethoscope, bladder emptying, relaxed positioning).
- Gamitin ang standardized pre-exam safety sequence: hand hygiene/PPE kung indicated, identity verification, exam explanation kasama ang consent, supine positioning, at modesty-preserving exposure.
- Isama ang focused oral-oropharyngeal screening kapag ang GI concerns ay may intake/swallowing issues: suriin ang lips, buccal mucosa, gums/teeth, tongue mobility, palate/uvula, at tonsillar/oropharyngeal findings.
- Ituring ang bagong lip asymmetry na may facial droop, arm weakness/numbness, o speech change bilang potential acute stroke pattern na nangangailangan ng immediate escalation.
- Kung pinaghihinalaan ang epiglottitis (halimbawa stridor, hyperthermia, drooling, severe sore throat), iwasan ang tongue-depressor provocation dahil sa airway-spasm risk at agarang i-escalate.
- Suriin ang contour at distention habang supine at relaxed ang pasyente, at idokumento ang symmetry, contour type (flat/rounded/scaphoid/protuberant), scars, umbilicus position, masses, at visible pulsations/peristalsis.
- Sa inspection, kumpirmahin ang relaxed abdominal wall (arms at sides; head/knee support kung kailangan) at idokumento ang striae, hernia-like bulges, scar correlation, at umbilicus (karaniwang inverted at midline).
- Gamitin ang method-specific expected/unexpected framing sa exam:
- Inspection expected findings: flat/rounded contour na may symmetry at intact skin.
- Inspection unexpected findings: asymmetry, progressive distention, visible peristalsis/pulsation, wounds, o skin breakdown.
- Auscultation expected finding: normal bowel sounds.
- Auscultation unexpected findings: absent/hyperactive/hypoactive bowel sounds.
- Palpation expected findings: walang masses, walang tenderness, walang involuntary guarding.
- Palpation unexpected findings: pain, rebound tenderness, rigidity, involuntary guarding, o new masses.
- GU expected findings: clear pale-yellow urine at nondistended bladder na walang urgency/frequency/retention.
- GU unexpected findings: dark/bloody/foul/sedimented urine, dysuria, urgency/frequency, distended tender bladder, o retention signs.
- Auscultate bowel sounds bago palpation upang maiwasang mabago ang baseline findings; magsimula sa RLQ at umikot clockwise.
- Kung hindi agad marinig ang bowel sounds, ipagpatuloy ang pakikinig nang hanggang humigit-kumulang 5 minuto sa quadrant na iyon bago sabihing may marked hypoactivity/absence.
- Ilarawan ang bowel sounds bilang normal/hyperactive/hypoactive sa halip na eksaktong bilangin ang frequency dahil cyclic ang bowel activity.
- Kilalanin na ang normal bowel activity ay maaaring may mahabang peak-to-peak variation (hanggang humigit-kumulang 50 hanggang 60 minuto), kaya hindi dapat agad tawaging absent sounds ang maiikling silent intervals.
- Kilalanin ang auscultation red flags: hyperactive sounds o borborygmus, hypoactive sounds pagkatapos ng surgery/ileus patterns, at unexpected vascular sounds gaya ng bruits.
- Kung malinaw ang peristaltic-sound conduction sa kabuuan ng abdomen, maaaring sapat ang single-location auscultation para sa trend checks, habang nananatiling standard ang complete quadrant review para sa initial focused assessment.
- I-interpret ang bowel-sound changes sa motility context: ang absent o markedly altered sounds ay maaaring magpahiwatig ng obstruction, ileus, o inflammatory processes at tumutulong suriin ang response sa bowel-rest o NG-decompression plans.
- Sa palpation, tasahin ang pain area sa huli at i-differentiate ang voluntary guarding mula sa involuntary guarding, rigidity, at rebound tenderness.
- Para sa light palpation, magsimula sa RLQ at umikot clockwise na may shallow pressure (humigit-kumulang 1 cm); iwan ang painful area sa huli at hikayatin ang knee flexion upang mabawasan ang muscle guarding.
- Iwasan ang deep palpation kapag pinaghihinalaang may contraindications (halimbawa abdominal aortic aneurysm, appendicitis concern, tender spleen, polycystic-kidney rupture risk, o recent kidney transplant).
- Palpate ang suprapubic-to-umbilical midline para sa bladder distention kapag pinaghihinalaan ang retention; ang distended bladder ay maaaring magpakita bilang smooth, firm, regular, midline pelvic mass.
- I-differentiate ang guarding patterns: voluntary guarding (anxiety/cold-touch related), involuntary guarding (reflex contraction na may peritoneal irritation), rigidity (persistent involuntary muscle hardening), at rebound tenderness (pain sa biglaang release).
- Gamitin ang percussion findings (tympany versus dullness) upang suportahan ang concern para sa stool burden, mass effect, o abnormal fluid patterns; ang paglipat mula expected tympany patungo sa diffuse/shifting dullness ay sumusuporta sa ascitic-fluid concern.
- Maaaring suportahan ng percussion ang liver/spleen span assessment at costovertebral-angle tenderness screening sa upper-level abdominal-kidney evaluation.
- I-trend ang common GI laboratory indicators kasama ang clinical picture, kabilang ang anemia/inflammation cues sa CBC, hepatobiliary markers/electrolytes sa CMP, at lipase para sa pancreatic involvement.
- Gumamit ng stool diagnostics (occult blood, culture kabilang ang C. diff testing, ova/parasite testing) at inflammatory markers (CRP/ESR) upang pinuhin ang differential priorities.
- Magdagdag ng albumin at thyroid-function trends kapag ang malnutrition, malabsorption, o bowel-motility concerns ay bahagi ng working differential.
- Itugma ang imaging modality sa clinical question at prep needs: abdominal X-ray (obstruction/perforation screening), CT (detalye na may contrast at renal/allergy review), MRI/MRCP (walang radiation; metal/implant at claustrophobia screening), ultrasound (radiation-free hepatobiliary/pancreatic assessment), at barium studies (bowel-prep/NPO at posttest fluid-fiber elimination support).
- Para sa abdominal CT na may contrast, beripikahin ang NPO status (madalas 4-6 oras ayon sa order), prior iodine/contrast reaction history, renal labs (BUN/creatinine/eGFR), at medication constraints gaya ng metformin timing restrictions.
- Para sa prior contrast-reaction history, beripikahin kung inutos at nakumpleto ang premedication pathways (halimbawa antihistamine/corticosteroid protocols) bago contrast exposure.
- Kumpirmahin ang pagtanggal ng metal/jewelry items bago imaging modalities kung saan kailangan ito ng protocol.
- Ituro ang expected contrast sensations (maikling warmth o metallic taste sa IV contrast; chalky taste sa oral contrast) at suportahan ang posttest hydration upang makatulong sa contrast elimination.
- Pagkatapos ng barium studies, asahan ang pansamantalang light/white stool at palakasin ang ordered laxative plus hydration plan upang mabawasan ang postprocedure impaction risk.
- Para sa pinaghihinalaang lactose malabsorption o small-intestinal bacterial overgrowth, asahan ang ordered hydrogen/methane (kabilang ang lactulose-based) breath-testing workflows at prep teaching.
- Sa mga pasyenteng may malakas na hereditary colorectal-cancer/polyposis patterns, i-coordinate ang genetics-risk referral pathways at idokumento ang family-history clues na nakaaapekto sa surveillance planning.
- I-integrate ang endoscopy planning at surveillance: colonoscopy/EGD/ERCP sedation workflows na may consent at NPO checks, kasama ang postprocedure monitoring para sa bleeding, perforation, pancreatitis/cholangitis risk pagkatapos ng ERCP, at capsule-retention risk sa pinaghihinalaang stricture/obstruction/fistula patterns.
- I-ugnay ang quadrant pain patterns sa malamang causes, pagkatapos ay asahan ang diagnostics kapag clinically indicated.
- Sa older-adult constipation-focused assessment, mag-screen para sa abdominal/pelvic-floor weakness, immobility, malnutrition, chronic disease burden, at long-term medication contributors.
- Direktang itanong ang constipation-complication questions (hemorrhoid bleeding, fissure pain, fecal impaction history, rectal ulcer risk).
- Ilapat ang life-span interpretation sa GI assessment: maaaring expected ang protuberant contour sa infant/young-child, tumutulong ang diaper counts sa hydration tracking, at nangangailangan ang older adults ng mas mahigpit na screening para sa constipation, xerostomia/taste change, reflux risk, ulcer risk, at bacterial-overgrowth-related diarrhea o weight loss.
- Sa infants at toddlers, isama ang wet-diaper count trends, kumpirmahin ang umbilical-cord stump drying/fall-off timing (humigit-kumulang dalawang linggo), at kilalanin ang abdominal respiratory movement bilang expected observation pattern.
- Sa pediatric abdominal complaints, asahan ang nonspecific symptom language (halimbawa “sumasakit ang tiyan ko”) at isama ang caregiver-reported functional cues gaya ng nabawasang school attendance.
Mga Interbensyon sa Nursing
- Isagawa ang standardized interview at exam sequence para sa bawat focused abdominal concern.
- Idokumento ang findings ayon sa quadrant at exam method upang mapabuti ang handoff clarity.
- I-escalate ang findings gaya ng severe focal tenderness, bleeding signs, persistent vomiting, o progressive distention.
- Beripikahin na concordant ang subjective at objective data bago i-finalize ang interpretation; kung discordant, ulitin ang focused exam elements at linawin ang interview responses.
- Ihanda ang mga pasyente para sa inutusang diagnostics at specimen collection gamit ang privacy-preserving communication.
- Muling tasahin pagkatapos ng interventions at i-update ang care plan habang umuunlad ang cues.
- Sa pregnancy/postpartum assessment, kilalanin ang expected abdominal-wall stretching at transient linea-alba/rectus separation patterns habang ini-escalate ang persistent pain, functional decline, o concerning associated findings.
- Para sa older adults, palakasin ang activity-plus-fiber lifestyle strategies at i-monitor ang age-related abdominal changes (slower motility/metabolism, weaker muscle tone/ligament support, increasing visceral-fat burden) na nagpapataas ng constipation, hernia, at prolapse risk.
- Kapag inutos ang stool testing, magbigay ng privacy-preserving, stigma-reducing instructions para sa specimen collection at transport upang mapabuti ang adherence at sample quality.
Panganib ng Sequence Error
Ang palpation bago auscultation ay maaaring magbaluktot ng bowel sound interpretation at magpababa ng diagnostic value ng exam.
Pharmacology
Nakadepende ang pharmacologic management sa natukoy na sanhi at hindi pangunahing paksa sa assessment-focused na seksyong ito. Dapat sumunod ang medication decisions sa confirmed clinical findings at provider orders.
Paglalapat ng Clinical Judgment
Klinikal na Sitwasyon
Isang pasyente ang nag-uulat ng bagong right lower abdominal pain na may nausea at reduced appetite. Ginagamit ang interview cues at focused exam findings upang magpasya sa mga susunod na aksyon.
- Recognize Cues: Localized pain pattern, associated symptoms, at bowel trend changes.
- Analyze Cues: Ang pattern ay nagmumungkahi ng posibleng acute abdominal pathology sa halip na nonspecific discomfort.
- Prioritize Hypotheses: Agarang prayoridad ang pag-rule out ng time-sensitive causes at pagpigil ng progression.
- Generate Solutions: Kumpletuhin ang focused exam sequence, idokumento ang quadrant findings, at i-escalate ang concerning cues.
- Take Action: Agad na i-notify ang provider at suportahan ang inutusang diagnostics.
- Evaluate Outcomes: Muling tasahin ang pain trajectory at physiologic stability pagkatapos ng interventions.
Mga Kaugnay na Konsepto
- digestive system - Nagbibigay ng pundasyong GI anatomy at elimination context.
- abdominal distention at ang five Fs - Pinapalawak ang differential cues para sa generalized abdominal swelling.
- abdominal hernias - Sumasaklaw sa localized bulge patterns at structural wall defects.
- pagtatasa at pamamahala ng diarrhea - Karaniwang sintomas na nangangailangan ng stool-pattern at hydration assessment.
- constipation - Madalas na elimination issue na kaugnay ng distention at discomfort.
- social determinants of health - Binabalangkas ang food access, coverage, at screening barriers na nagmomodify ng GI risk at follow-up.
- kulturang tumutugong pagkolekta ng assessment data - Sumusuporta sa culturally safe interview technique at interpretation ng symptom language.
- dysphagia - Ang swallowing complaints at stroke history ay nangangailangan ng maagang aspiration-risk screening sa GI interviews.
Sariling Pagsusuri
- Bakit naiiba ang abdominal exam sequencing kumpara sa maraming ibang physical exams?
- Paano pinapabuti ng PQRST ang differential reasoning para sa abdominal pain?
- Aling interview findings ang dapat mag-trigger ng immediate escalation sa abdominal assessment?