Seizures and Epilepsy
Key Points
- A seizure is sudden uncontrolled neuronal discharge that can alter movement, sensation, behavior, and awareness.
- Epilepsy is defined by recurrent unprovoked seizures (at least two events, at least 24 hours apart).
- In the United States, epilepsy affects millions of people and can substantially reduce quality of life without sustained management support.
- status-epilepticus (seizure >5 minutes or serial seizures without recovery) is a neurologic emergency.
- Priority nursing goals are airway protection, injury prevention, trigger reduction, and medication adherence.
- In selected refractory epilepsy pathways, ketogenic-style nutrition therapy can reduce seizure burden when managed with the care team.
- Antiepileptic regimens can alter micronutrient status, bone-health risk, appetite/weight pattern, and selected drug-food interactions.
- In advanced illness, seizure prevention and trauma reduction remain priorities even when goals of care are comfort-focused.
Pathophysiology
Seizures develop when excitatory and inhibitory signaling becomes imbalanced in the CNS, often involving reduced GABA-mediated inhibition and/or abnormal electrical firing networks. The resulting surge of synchronized activity can produce focal or generalized neurologic manifestations.
Etiology may be idiopathic or secondary to structural, metabolic, infectious, vascular, toxic, withdrawal, or traumatic processes. Postictal recovery may range from immediate return to baseline to prolonged fatigue, confusion, or weakness.
Classification
- Focal (partial) seizures: Begin in one cerebral hemisphere.
- Focal-onset aware seizures: Awareness preserved; may include aura (for example deja vu, unusual smell, sudden pain), unilateral motor/sensory change, or autonomic symptoms.
- Focal-onset impaired-awareness seizures: Confusion or reduced awareness with automatisms (for example lip smacking, repetitive leg movements), possible wandering, and postictal amnesia.
- Generalized seizures: Bilateral hemispheric involvement.
- Generalized subtypes: absence, tonic, clonic, tonic-clonic, myoclonic, and atonic (high injury risk from sudden tone loss).
- Unclassified seizures: Mixed-pattern or unclear etiology, including primary/idiopathic and secondary causes.
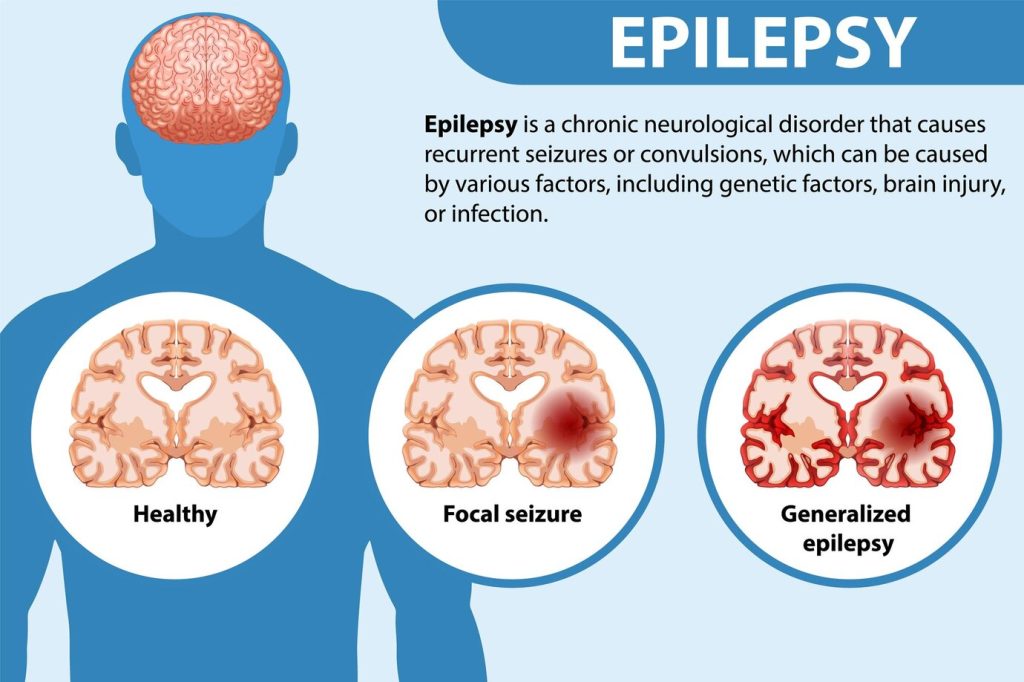 Illustration reference: OpenRN Health Alterations Ch.9.7.
Illustration reference: OpenRN Health Alterations Ch.9.7.
Seizure Phases and Triggers
- Phases: prodromal (preictal), aura, ictal, and postictal.
- Common triggers: stress, fatigue, sleep deprivation, alcohol/caffeine excess, dehydration or missed meals, hormonal fluctuation, flashing visual stimuli, toxins, and some medication/substance exposures.
- Nutrition-therapy context: Ketogenic or modified Atkins plans may be used in selected refractory epilepsy cases (more common in pediatrics) with close interdisciplinary monitoring.
Nursing Assessment
NCLEX Focus
During and immediately after seizure activity, first priorities are airway, oxygenation, and injury prevention.
- Obtain detailed history: event count, duration, pattern, aura presence, level of consciousness, and pre/during/post-seizure findings.
- During active events, capture exact onset and duration timing and whether consciousness returns between episodes to identify status-epilepticus risk quickly.
- Assess medication, supplement, alcohol, and substance-use context and comorbid neurologic/metabolic risk factors.
- Assess for medication-related nutrition effects (weight change, appetite shift, vitamin/mineral depletion, constipation, and bone-health risk).
- Assess medication-access barriers (for example cost/insurance loss) because nonadherence is a frequent, preventable trigger of breakthrough seizures.
- Assess recent medication toxicity/withdrawal risk and organ-failure-related metabolic imbalance as potential seizure precipitants.
- Assess postictal airway safety, neuro status, agitation, orientation, and return-to-baseline timing.
- In school-age epilepsy care, assess attendance disruption, learning-impact burden, and readiness of school action plans/rescue-medication workflows.
- Use diagnostics to confirm pattern and rule out causes: EEG or SEEG, CT/MRI, SPECT/PET, lumbar puncture in selected infectious contexts, and blood tests (electrolytes, CBC, glucose, toxicology, therapeutic drug levels such as phenytoin/phenobarbital).
Nursing Interventions
- If aura occurs, move client to a safe private area and protect from environmental injury.
- During seizure: do not restrain, do not insert objects into mouth, protect head, loosen tight clothing, remove nearby hazards/glasses/neck items when feasible, and time the event.
- Escalate immediately for status epilepticus and support emergency response workflow.
- After seizure: side-lying recovery position, airway confirmation, vital signs/neuro checks, reorientation, calm communication, and documentation of aura presence, onset time, active-duration time, and postictal recovery length.
- Maintain inpatient seizure precautions when indicated (ready oxygen/suction equipment, bed in low position, agency-based side-rail precautions).
- Support psychosocial coping and family preparedness for recurrent-event management.
- In school settings, coordinate seizure action plans with caregivers, school nurse, teachers/coaches, and provider orders for rescue-medication availability.
- Provide seizure first-aid training and anti-stigma education support for school staff and peers to reduce preventable harm and social isolation.
- If ketogenic therapy is prescribed, reinforce strict carbohydrate limits and verify hidden sugar sources in medications and supplements (for example syrup formulations and gummy vitamins), because small sugar exposures can reduce therapeutic effect.
- Reinforce common antiepileptic interaction precautions: avoid alcohol with anticonvulsants, separate phenytoin from enteral feedings, and review diet pattern issues (for example high soy intake with valproate plans) with pharmacy/dietitian support.
Medical and Surgical Management
- Acute seizure control may include IV benzodiazepines (for example lorazepam, diazepam, or midazolam), with cardiorespiratory monitoring and airway support.
- Maintenance therapy commonly uses antiepileptic drugs (for example levetiracetam, phenytoin, phenobarbital), plus fluid/electrolyte correction when indicated.
- Drug-resistant focal epilepsy may require resective/disconnection procedures (for example lobectomy, corpus callosotomy, hemispherotomy, multiple subpial transection, or thermal-ablation pathways) in selected surgical candidates.
- Neuromodulation options may include vagal-nerve stimulation, responsive neurostimulation, or deep-brain stimulation in selected refractory pathways.
High-Risk Deterioration
Prolonged seizures can cause neuronal injury, hypoxia, aspiration, and cardiorespiratory compromise if escalation is delayed.
Pharmacology
| Medication Context | Examples | Key Nursing Considerations |
|---|---|---|
| Acute seizure termination | IV lorazepam, diazepam, midazolam | Continuous respiratory/cardiac monitoring and airway support are required. |
| Maintenance anticonvulsants | Levetiracetam, phenytoin, phenobarbital | Match drug to seizure type, monitor adverse effects/toxicity, and reinforce strict adherence. |
| Titration and monitoring strategy | Monotherapy-first approach in many clients | Titrate dose to seizure control/minimal toxicity; adjust for illness, stress, and weight changes. |
Current evidence does not support routine anti-seizure medication initiation after a first-time seizure in every client; rapid neurology follow-up and individualized risk discussion are prioritized.
Health Teaching and Evaluation
- Teach never to stop anticonvulsants abruptly and provide missed-dose instructions.
- Reinforce therapeutic-level lab follow-up and provider review before OTC/supplement use.
- If using ketogenic or modified Atkins plans, teach practical carbohydrate tracking (often very low total daily carbohydrate limits per prescription) and escalate concerns about diet tolerability or recurrent breakthrough seizures.
- Teach ongoing nutrition-lab follow-up for long-term antiepileptic therapy (for example vitamin D/calcium and selected B-vitamin status) to reduce deficiency and bone-loss risk.
- Teach emergency response steps for family/caregivers and when to call EMS.
- Reinforce trigger reduction, driving/machinery law adherence, medical-alert identification, and seizure-diary tracking.
- Link families to community support services such as epilepsy organizations.
- Reevaluate outcomes continuously and revise care plans when goals are partially met or unmet.
Clinical Judgment Application
Clinical Scenario
A hospitalized patient with known epilepsy develops a tonic-clonic seizure lasting 6 minutes with cyanosis and no return to consciousness between episodes.
- Recognize Cues: Prolonged/recurrent seizure activity with oxygenation risk.
- Analyze Cues: Status epilepticus is likely and can cause rapid neurologic injury.
- Prioritize Hypotheses: Airway and oxygenation stabilization plus emergency seizure termination are immediate priorities.
- Generate Solutions: Activate emergency response, protect airway, prepare IV benzodiazepine administration, and continuous monitoring.
- Take Action: Implement seizure-safety bundle, document timing/findings, and communicate deterioration.
- Evaluate Outcomes: Seizure activity stops, oxygenation stabilizes, and recovery trend is reassessed.
Related Concepts
- anticonvulsants - Core long-term pharmacologic seizure-prevention framework.
- febrile-seizures - Pediatric fever-associated seizure pattern with age- and duration-based classification.
- neurological-diagnostic-testing-and-nursing-considerations - EEG/imaging/lab safety and interpretation context.
- common-neurological-disorders-recognition-and-priority-care - Escalation framework for seizure emergencies.
- nursing-care-priorities-for-neuromuscular-impairment - Airway and aspiration-risk prevention overlap.
- meningitis-priority-care-and-icp-risk - Infectious etiologies can precipitate seizure activity.
Self-Check
- Which bedside actions are contraindicated during an active generalized seizure?
- When does seizure activity meet status-epilepticus criteria requiring emergency escalation?
- Which teaching points most reduce breakthrough-seizure risk in home management?