Soft Tissue Injuries
Key Points
- Soft tissue injuries commonly affect muscles, tendons, ligaments, and bursae.
- Frequent patterns include sprain, strain, contusion, tendinitis, and bursitis.
- Most cases improve with conservative care, especially early RICE-based management.
- Nursing priorities are symptom control, edema reduction, mobility protection, and prevention teaching.
Pathophysiology
Soft tissue injuries result from overload, overuse, direct blunt trauma, falls, sports movement, and age-related tissue vulnerability. Injury severity depends on force, mechanism, and the specific tissue involved.
Sprains and strains usually follow twisting, pulling, or rapid directional change. Contusions follow direct impact with tissue bleeding under intact skin. Repetitive tendon loading causes tendinitis; adjacent bursal inflammation can follow, producing bursitis.
Classification
- Sprain: Ligament overstretching or tear (often ankle, knee, wrist).
- Strain: Muscle or tendon overstretching or tear (often back or hamstring region).
- Contusion: Blunt-force bruising injury to muscle/soft tissue without skin break.
- Tendinitis: Overuse-driven tendon inflammation/irritation (commonly shoulder, elbow, knee, ankle, foot).
- Bursitis: Bursa inflammation, often overlapping with tendon overuse syndromes.
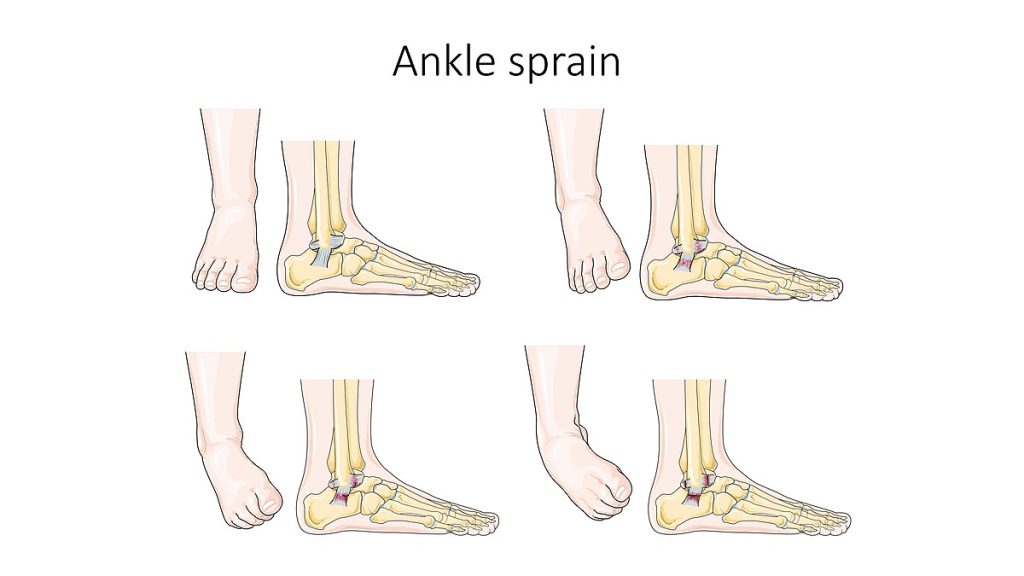 Illustration reference: OpenRN Health Alterations Ch.10.10.
Illustration reference: OpenRN Health Alterations Ch.10.10.
Nursing Assessment
NCLEX Focus
Identify mechanism first, then confirm severity and functional impact.
- Assess mechanism (sports movement, fall, trauma, repetitive overuse).
- Assess pain location/intensity, swelling, bruising, redness, weakness, and muscle spasm.
- Assess movement limitation and functional impact (weight bearing, grip, gait, ADLs).
- Assess for red flags suggesting broader injury burden (severe deformity, neurovascular change, suspected fracture).
- For less-obvious injuries, anticipate advanced imaging support (CT/MRI); x-ray is most useful when bone injury is suspected.
- In trauma/fall contexts with bleeding concern, monitor ordered blood-loss labs (for example hemoglobin/hematocrit).
Nursing Interventions
- Implement RICE early when appropriate:
- Rest: Pause the provoking activity.
- Ice: Apply cold packs about 20 minutes at a time, multiple times daily.
- Compression: Use compression wrap/bandage to reduce swelling.
- Elevation: Elevate injured area above heart level to reduce edema.
- For sprain stabilization, assist with first brace application and verify independent reapplication before discharge.
- Reinforce pain/swelling reassessment and safe progression back to activity.
- Schedule or reinforce follow-up when symptom resolution is delayed.
Prevention Teaching
- Use proper equipment and properly fitted footwear.
- Warm up before activity and cool down afterward.
- Stretch before and after exercise.
- Maintain hydration during activity.
- Build planned rest intervals during repetitive or high-intensity activity.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| nsaids | Ibuprofen, naproxen | First-line in many soft tissue injuries for pain and swelling reduction. |
| opioids | Short-course severe-pain contexts | Usually avoided in routine cases; use only when pain severity justifies short-term escalation. |
Clinical Judgment Application
Clinical Scenario
A patient presents after a weekend basketball game with ankle swelling, bruising, and painful weight bearing.
- Recognize Cues: Acute activity-related soft tissue injury pattern with edema and pain.
- Analyze Cues: Mechanism and findings are most consistent with ankle sprain/strain spectrum.
- Prioritize Hypotheses: Limit further tissue damage and control swelling/pain while screening for fracture risk.
- Generate Solutions: Start RICE, support brace use, and plan reassessment/follow-up.
- Take Action: Implement compression/elevation teaching and verify safe home self-management.
- Evaluate Outcomes: Swelling and pain decrease, ROM improves, and function returns progressively.
Related Concepts
- common-musculoskeletal-disorders-recognition-and-care-priorities - Differential recognition across musculoskeletal injury and disease patterns.
- immobilization-devices-and-restraint-safety - Brace and support-device safety checks.
- fracture - Distinguishing soft tissue injury from bone injury in trauma pathways.
- promoting-joint-mobility-and-activity - Safe return-to-activity progression after acute injury.
Self-Check
- What assessment findings help distinguish sprain from strain and contusion?
- Why is early RICE timing important for symptom control and recovery?
- Which findings should trigger escalation beyond routine conservative soft tissue care?