Tanner’s Clinical Judgment Model in Nursing Practice
Key Points
- Tanner’s model structures judgment as noticing, interpreting, responding, and reflecting.
- The model complements ADPIE by clarifying how nurses reason within each nursing-process phase.
- Clinical judgment integrates objective and subjective patient information to reach safe care conclusions that improve outcomes.
- Judgment is iterative: reflection and new cues can trigger immediate reprioritization.
- Context, communication, and self-awareness influence judgment quality.
- The model is especially useful for helping early-career nurses build explicit clinical-judgment habits.
Pathophysiology
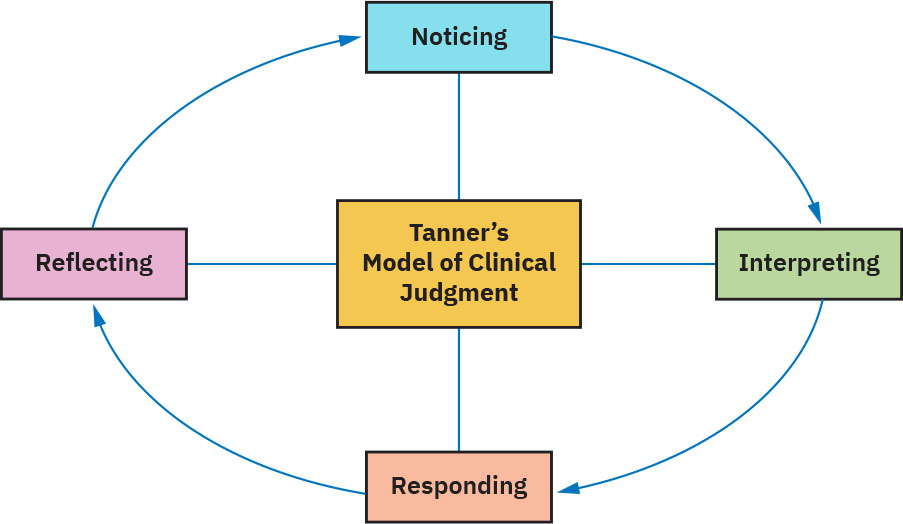 Illustration reference: OpenStax Clinical Nursing Skills Ch.1.
Illustration reference: OpenStax Clinical Nursing Skills Ch.1.
Tanner’s framework describes cognitive processing, not a disease mechanism. It explains how nurses move from patient cues to safe action and then back to self-evaluation. In rapidly changing care environments, this loop supports earlier recognition of deterioration and faster plan adjustment.
Classification
- Noticing: Identify relevant objective and subjective cues.
- Interpreting: Analyze cue meaning and generate priority hypotheses.
- Responding: Select and implement actions based on risk and feasibility.
- Reflecting: Evaluate outcomes and examine reasoning to improve future decisions.
- Reflection in action: Real-time plan adjustments while care is being delivered.
- Reflection on action: Post-encounter review of decision quality and alternative options.
Nursing Assessment
NCLEX Focus
Clinical judgment questions often test whether the nurse can reprioritize after new cues emerge.
- Assess whether important cues are recognized early and separated from noise.
- Assess whether interpretations are evidence-aligned and context-aware.
- Assess whether responses are safe, timely, and individualized.
- Assess whether reflection leads to concrete plan revision.
- Assess barriers such as cognitive overload, communication gaps, and bias.
- Assess expected versus actual outcomes and identify gaps in reasoning.
Nursing Interventions
- Use Tanner language during handoff and debrief to make reasoning explicit.
- Pair judgment decisions with measurable expected outcomes.
- Reassess continuously and update hypotheses when trends shift.
- Document rationale for major prioritization changes.
- Use reflective questioning after complex cases to strengthen future performance.
- Seek interdisciplinary feedback to improve future judgment quality.
Reflection Omission Risk
Skipping reflection can preserve ineffective reasoning patterns and delay improvement.
Pharmacology
Medication decisions should follow the same cycle: notice response and adverse cues, interpret likely causes, respond with safe adjustments or escalation, and reflect on outcome quality.
Clinical Judgment Application
Clinical Scenario
A patient has subtle early changes in vitals and mentation during a routine reassessment.
Noticing: Detect trend changes that differ from baseline. Interpreting: Link findings to potential early deterioration. Responding: Prioritize monitoring escalation and targeted interventions. Reflecting: Evaluate if actions stabilized the patient and refine future threshold recognition.
Related Concepts
- ana-nursing-process-competencies - Operational ADPIE structure used with judgment reasoning.
- evidence-based-decision-making-in-nursing - Supports interpretation and response quality.
- clinical-judgment-within-the-nursing-process - Maternal-newborn application of similar reasoning cycle.
- clinical-judgment-measurement-model - Broader measurement framework for judgment performance.
Self-Check
- How is Tanner’s model different from ADPIE, and where do they overlap?
- What cue patterns should trigger immediate reprioritization?
- Which reflection behaviors improve judgment accuracy over time?