Mga Indikasyon ng CVAD at Pagpili ng Device
Mahahalagang Punto
- Karaniwang indicated ang CVAD placement para sa long-term infusion therapy, high-osmolarity infusions, vesicant medications, at piling emergency access needs.
- Binabawasan ng central infusion sa malaking ugat (gaya ng superior vena cava) ang irritation risk sa pamamagitan ng hemodilution.
- Dapat i-individualize ang device at site selection ayon sa therapy duration, medication profile, vascular characteristics, at patient-specific risk factors.
- Hindi ideal ang PICC lines para sa lahat ng clients; halimbawa, sa vein-preservation priorities sa end-stage renal disease, maaaring mas pabor ang alternatibong access planning.
- Nangangailangan ng specially trained clinicians ang CVAD insertion, habang ang bedside nursing maintenance at aseptic care ay patuloy na safety priorities.
- Invasive at may kaakibat na panganib ang CVAD insertion, kaya dapat isaalang-alang ang alternative access bago placement kung naaangkop.
Pathophysiology
Naitutulak ang paggamit ng CVAD ng vascular safety at delivery reliability. Maaaring makasira sa peripheral vessels o nakapaligid na tissue ang high-osmolarity solutions (halimbawa total parenteral nutrition at hypertonic IV fluids) at vesicants kapag may infiltration o extravasation. Ang paghahatid ng mga therapy na ito sa malaking central vein ay nagpapabuti ng dilution at nagpapababa ng local endothelial injury risk.
Kabilang sa common insertion pathways ang neck, chest, o groin venous entry (halimbawa internal jugular, subclavian, o femoral) na may catheter advancement hanggang ang tip ay nasa central location (gaya ng superior vena cava, inferior vena cava, o right atrial region ayon sa device purpose at policy).
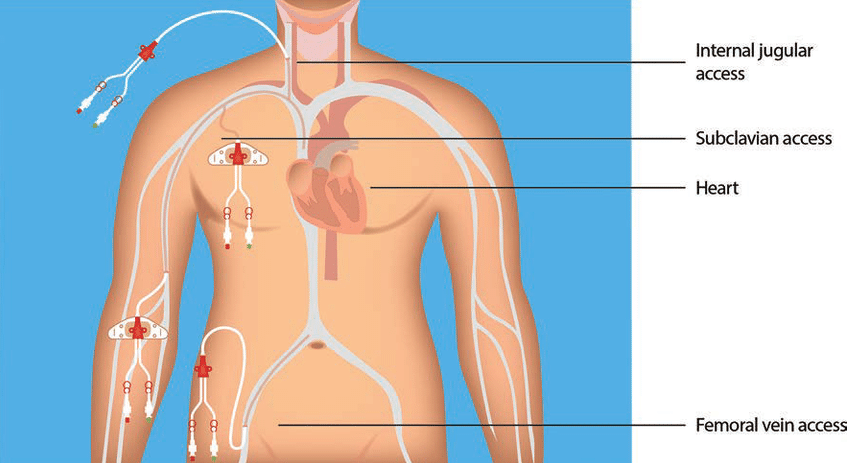 Illustration reference: OpenRN Nursing Advanced Skills Ch.4.1.
Illustration reference: OpenRN Nursing Advanced Skills Ch.4.1.
Para sa critically ill patients, maaari ring suportahan ng central access ang mabilis na fluid resuscitation at hemodynamic monitoring. Sa context na ito, ipinapakita ng central venous pressure ang pressure malapit sa right atrial entry at maaaring gamitin bilang preload-oriented volume-status measure sa resuscitation planning.
Classification
- PICC: Manipis na catheter na ipinapasok sa upper-arm vein at inaabante hanggang superior vena cava; karaniwang ginagamit sa loob ng ilang linggo hanggang buwan at maaaring gamitin para sa blood sampling ayon sa policy. Mag-ingat sa clients na may end-stage renal disease, thrombosis history, o hypercoagulable risk kapag kailangan ang long-term vein preservation.
- Non-tunneled CVAD: Karaniwang duration ay ilang araw hanggang ilang linggo; ginagamit para sa mas maiikling high-acuity needs. Sa adults, madalas na mas pinipili ang subclavian placement kaysa femoral access kapag clinically feasible dahil maaaring mas mababa ang thrombosis at infection risk.
- External tunneled CVAD: Long-term o permanent access na may subcutaneous tunnel upang mabawasan ang bloodstream entry risk.
- Implanted venous access device (port/IVAD): Long-term o permanent access na nakakabit sa reservoir pocket at ina-access gamit ang noncoring needle; madalas na mas hindi nakikita at mas mababa ang daily-activity maintenance kaysa external devices.
- Lumen configuration: Pinipili ang single-, double-, o multi-lumen configurations ayon sa therapy needs. Karaniwang triple-lumen use patterns ay naglalagay ng fluids/TPN/medications sa proximal o middle lumens, habang ang mas malaking distal lumen ay karaniwang inilalaan para sa blood administration, blood sampling, at central venous pressure monitoring ayon sa policy.
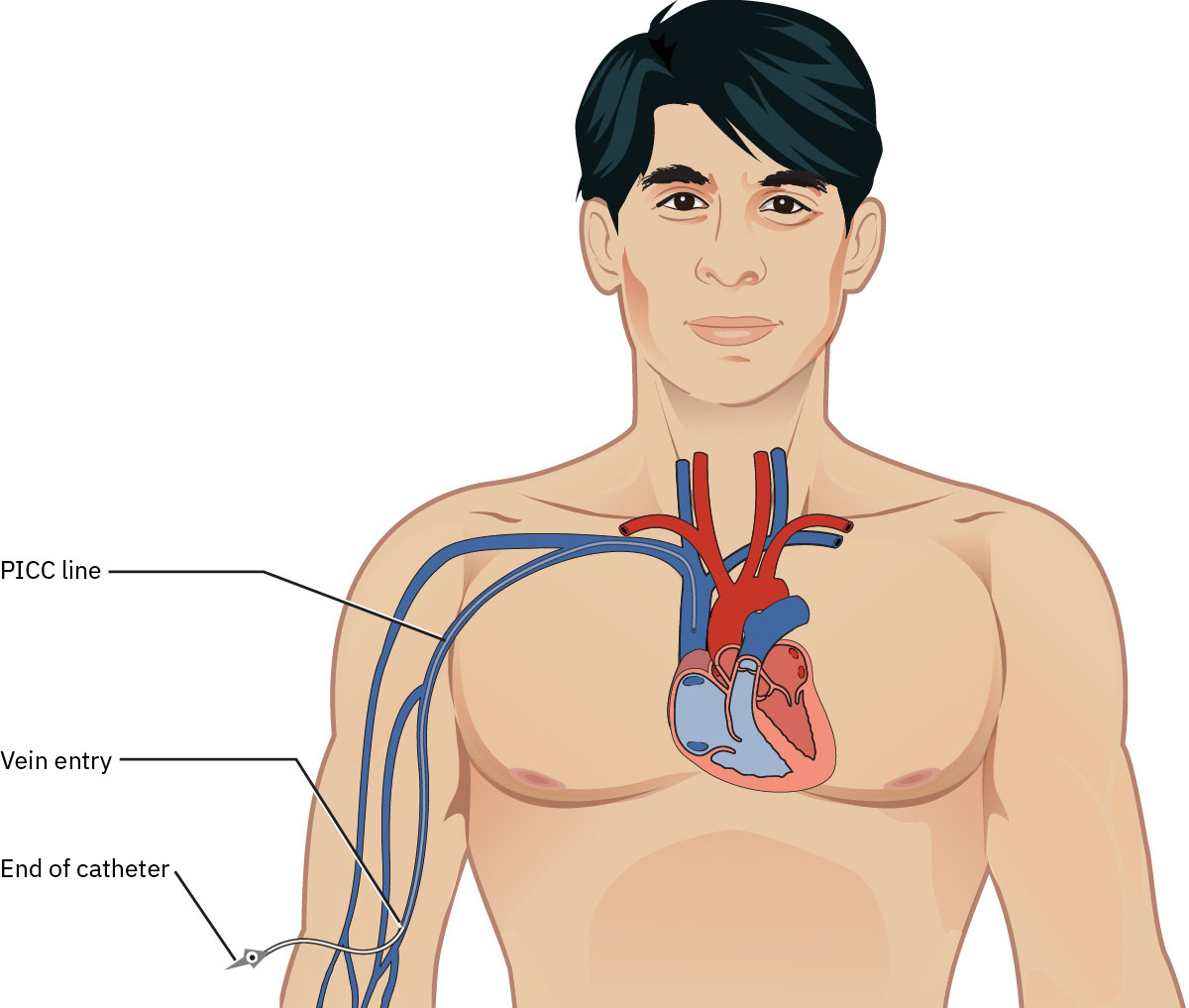 Illustration reference: OpenStax Clinical Nursing Skills Ch.13.
Illustration reference: OpenStax Clinical Nursing Skills Ch.13.
Nursing Assessment
NCLEX Focus
Madalas na tinatanong sa prioritization questions kung aling infusion types ang nangangailangan ng central access at aling patient factors ang nagpapaligtas sa isang specific device.
- Tayahin ang indication type: long-duration therapy, vesicant administration, high-osmolarity infusion, o resuscitation need.
- Tayahin ang inaasahang tagal ng therapy bago magrekomenda ng device type.
- Tayahin ang inaasahang lumen needs bago insertion (halimbawa hiwalay na lumen use para sa blood products, CVP monitoring, parenteral nutrition, at incompatible medications).
- Tayahin ang vessel characteristics, prior infusion history, medical history, edad, at cognitive factors na relevant sa maintenance safety.
- Tayahin kung available ang ultrasound-guided insertion support dahil pinapabuti nito ang insertion success at maaaring magpababa ng placement complications.
- Tayahin ang contraindication risk patterns, kabilang ang peripheral-flow limitations o thrombosis-prone history.
Nursing Interventions
- Makipagtulungan sa provider at care team sa device/site planning bago insertion.
- Beripikahing naidokumento sa medical record ang indication, risk explanation, at informed plan.
- Suportahan ang site-appropriate safety strategy (central vs peripheral approach) batay sa therapy profile.
- Beripikahin ang catheter-tip location gamit ang accepted method (halimbawa real-time fluoroscopy o post-procedure chest X-ray kapag hindi ginamit ang fluoroscopy) at tiyaking may tip location documentation bago tuloy-tuloy na paggamit.
- I-stabilize ang catheter gamit ang sutured o sutureless engineered securement ayon sa device type at policy upang mabawasan ang dislodgement at treatment interruption.
- Palakasin ang mahigpit na aseptic practice sa insertion support at sa lahat ng maintenance tasks dahil pinapataas ng CVADs ang bloodstream-infection risk.
- Magsagawa ng structured surveillance para sa thrombosis, occlusion, phlebitis, at skin o tissue injury.
Panganib ng Extravasation Injury
Ang pagtagas ng vesicant sa nakapaligid na tissue ay maaaring magdulot ng malubhang tissue injury o destruction at nangangailangan ng agarang escalation.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| breast-cancer-chemotherapy-safety-and-support(breast-cancer chemotherapy safety and support) | Vesicant chemotherapy agents | Mas mainam ang central delivery kapag makabuluhan ang vesicant risk upang mabawasan ang malubhang lokal na injury potential. |
| [antibiotics] | Selected IV antibiotics with vessel-irritating profiles | Dapat isaalang-alang ng route at device choice ang endothelial irritation risk at treatment duration. |
| [vasopressors] | Continuous vasopressor infusions | Karaniwang mas pinipili ang central administration para sa high-risk extravasation prevention. |
Clinical Judgment Application
Clinical Scenario
Ang pasyente ay nangangailangan ng prolonged infusion ng hypertonic nutrition at intermittent vesicant medications, na may limitadong peripheral vein quality.
- Recognize Cues: High-osmolarity at vesicant therapies na may inaasahang mahabang treatment course.
- Analyze Cues: Pinapataas ng peripheral access ang panganib ng phlebitis, thrombosis, at tissue injury kung may dislodgement.
- Prioritize Hypotheses: Pangunahing prayoridad ang pagpili ng pinakaligtas at pinakamatibay na access route.
- Generate Solutions: Ihambing ang PICC, tunneled CVAD, at implanted port batay sa duration at patient factors.
- Take Action: Ipatupad ang team-selected CVAD plan at simulan ang ongoing complication monitoring.
- Evaluate Outcomes: Naipagpapatuloy ang therapy na may maaasahang access at walang major catheter-related harm.
Related Concepts
- peripheral IV access - Maaaring hindi sapat ang peripheral routes para sa vesicants o prolonged high-osmolarity therapy.
- parenteral nutrition monitoring - Karaniwang nangangailangan ng central access planning ang total parenteral nutrition.
- pagpapatupad ng CLABSI prevention bundle - Mahalaga ang infection prevention pagkatapos ng central-line placement.
- beripikasyon, pagsisimula, at pagtugon sa reaksyon sa blood transfusion - Isa pang high-risk intravascular workflow na nangangailangan ng mahigpit na verification practice.
- kaligtasan sa intravenous medication administration - Shared infusion-safety principles para sa route validation at reassessment.
Self-Check
- Bakit madalas idinadaan sa central veins ang high-osmolarity at vesicant infusions kaysa peripheral veins?
- Aling factors ang dapat gumabay sa pagpili sa pagitan ng PICC, non-tunneled CVAD, tunneled CVAD, at implanted port?
- Ano ang agarang nursing action kapag pinaghihinalaan ang extravasation ng vesicant?