Neurological Physical Assessment at Red Flag Screening
Mahahalagang Punto
- Pinagsasama ng neurological assessment ang subjective history at objective cognitive, cranial-nerve, motor, sensory, at coordination testing.
- Mahalaga ang bilateral comparison at trend-based reassessment para matukoy ang acute neurologic deterioration.
- Nangangailangan ng agarang escalation ang BEFAST findings, bagong aphasia, biglaang pagbabago sa mental status, at focal weakness.
- Ang maagang pagbabago sa level of consciousness ay high-priority cue at dapat mag-trigger ng structured reassessment (halimbawa Glasgow Coma Scale) at mabilis na escalation kapag lumalala.
Pisyopatolohiya
Maaaring magmula ang neurologic deficits sa structural injury, ischemia, infection, toxic-metabolic imbalance, neurodegeneration, o peripheral nerve dysfunction. Nag-iiba ang assessment findings ayon sa lokasyon ng lesion at bilis ng paglala.
Ang maagang bedside detection ng banayad na pagbabago sa language, movement, sensation, at coordination ay nakakatulong upang maiwasan ang pagkaantala sa time-sensitive treatment.
Nahuhubog din ang neurologic outcomes ng social at structural factors. Maaaring maantala ng access barriers, bias, at socioeconomic exposures ang diagnosis at specialist follow-up, na nagpapataas ng panganib ng advanced presentation at mas mahinang functional outcomes.
Klasipikasyon
- Subjective domains: Onset/timing ng dizziness, vertigo, numbness, weakness, dysphagia, dysphasia, seizures, confusion, at recent injury.
- Objective domains: Mental status/LOC, pupils, cranial nerve exam, motor strength, sensory function, cerebellar tests, gait, balance, at deep tendon reflex patterns.
- Mental-status component domains: LOC/orientation, appearance, behavior, affect/mood, speech, at cognitive performance.
- Escalation domains: Pinaghihinalaang stroke, seizure emergencies, lumalalang consciousness, at progressive focal deficits.
- Equity/risk domains: Access barriers, limits sa health literacy, at social determinants na maaaring makaapekto sa neurologic follow-up at treatment adherence.
- Screening-tool domains: GCS para sa LOC trend, NIHSS/BEFAST para sa acute stroke screening, at MMSE para sa stratification ng cognitive impairment.
- Abnormal-pattern domains: Altered mental status, altered language (aphasia), cranial-nerve deficits, sensory alteration (kabilang ang peripheral neuropathy), at motor-coordination alteration.
- Exam-type domains:
- Routine bedside exam: RN-focused mental status/LOC, pupils, motor strength, sensation, at gait checks na may paggamit ng GCS trend kapag indicated.
- Comprehensive neurologic exam: Pinalawak na cranial-nerve, cerebellar, deep tendon reflex, at MMSE-focused assessment, madalas sa specialty evaluation contexts.
- Periodic reevaluation exam: Reassessment at documentation sa nakatakdang oras para sa acute neurologic injury o illness ayon sa agency policy.
Pagsusuri sa Pag-aalaga
Pokus sa NCLEX
Unahin ang airway, breathing, at acute stroke o seizure risk kaysa sa mas mababang-acuity na chronic findings.
- Suriin ang orientation, attention, behavior, at level of consciousness gamit ang standardized tools kapag indicated.
- Magtatag ng LOC/orientation baseline sa admission at i-trend kahit bawat shift o ayon sa acuity protocol; ihambing ang mga pagbabago sa baseline na iyon.
- Gumamit ng direktang orientation prompts (name, place, day/date; kung kailangan day-of-week/month/season) at i-dokumento ang preserved versus impaired domains (halimbawa oriented to self only).
- Piliin ang lalim ng exam (routine vs comprehensive vs periodic reevaluation) batay sa care setting, kasalukuyang diagnosis, at active neurologic symptom burden.
- Kumuha ng history para sa kasalukuyang neurologic symptoms, nakaraang neurologic conditions, recent falls/head injury, at swallowing/speech concerns.
- Para sa acute neurologic complaints, gumamit ng PQRSTU-focused follow-up habang naghahanda ng agarang escalation kung may active stroke-like findings.
- Magtanong nang malinaw tungkol sa recent medication changes na maaaring magpalala ng dizziness o orthostatic symptoms, lalo na sa older adults na may fall risk.
- Suriin ang sedatives, analgesics, neuromuscular-blocking agents, alcohol, at substance use dahil maaaring makagulo ang mga ito sa interpretasyon ng neurologic exam.
- I-trend ang level of consciousness gamit ang consistent tools (halimbawa Glasgow Coma Scale sa acute care): 15 = best response, less than 8 = comatose range, 3 = unresponsive, at clinically significant ang pagbaba ng 2 o higit pang points.
 Illustration reference: OpenStax Clinical Nursing Skills Ch.26.2.
Illustration reference: OpenStax Clinical Nursing Skills Ch.26.2.
- Gumamit ng MMSE kapag indicated ang cognitive screening at i-interpret ayon sa score bands (mga 24-30 no major impairment, 18-23 mild impairment, less than 18 severe impairment) kasama ang clinical context.
- Ihiwalay ang altered mental-status patterns gamit ang history at trend: progressive dementia pattern, acute fluctuating delirium pattern, depressive cognitive slowing, at coma-level unresponsiveness.
- Suriin ang cranial-nerve function na may side-to-side comparison at pupil reactivity checks.
- I-classify ang cranial-nerve findings bilang sensory, motor, o mixed modality kapag nilolocalize ang deficits.
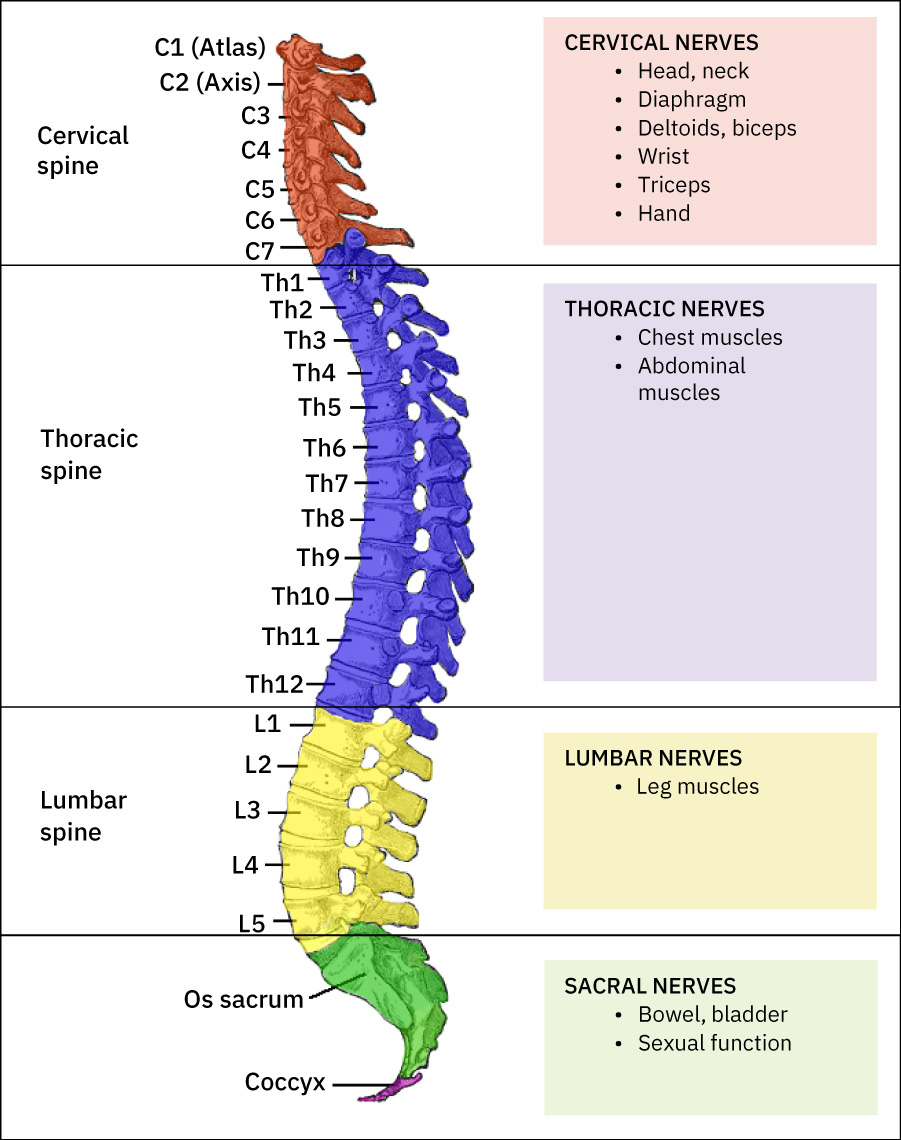 Illustration reference: OpenStax Clinical Nursing Skills Ch.26.1.
Illustration reference: OpenStax Clinical Nursing Skills Ch.26.1.
- Isama ang focused cranial-nerve screening tasks kapag indicated: CN I odor identification (eyes closed), CN II distance-vision check (halimbawa Snellen na may corrected-vision documentation), at pinagsamang CN III/IV/VI ocular tracking na may PERRLA checks.
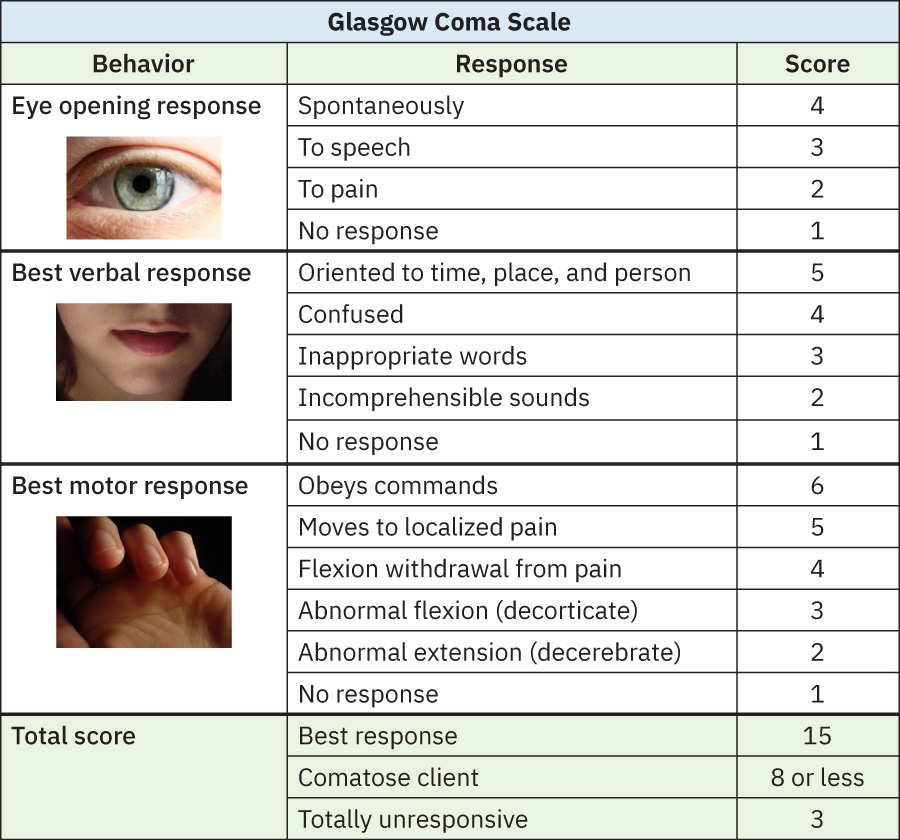 Illustration reference: OpenStax Clinical Nursing Skills Ch.26.2.
Illustration reference: OpenStax Clinical Nursing Skills Ch.26.2.
- Sa CN III/IV/VI screening, i-verify ang direct at consensual pupillary light constriction at i-dokumento ang asymmetric o sluggish responses bilang abnormal cues.
- Para sa CN V assessment, subukan ang light-touch sensation sa noo/pisngi/baba (eyes closed) at subukan ang motor strength sa pamamagitan ng palpation ng temporalis/masseter contraction habang nagki-clench ng ngipin at sinusuri ang symmetry sa jaw opening/closing.
- Sa comatose-patient assessment contexts, isama ang supervised corneal-reflex check (cotton-wisp blink response) kapag kinakailangan ng protocol para sa advanced CN V screening.
- Para sa CN VII screening, suriin ang facial symmetry at muscle strength sa smile, teeth-showing, bilateral eye closure, cheek puff, frown, at eyebrow raise tasks.
- Isama ang taste screening kapag kailangan (halimbawa hiwalay na salt/sweet/sour stimuli na eyes closed) at i-dokumento ang tamang identification at side-to-side differences.
- Para sa CN VIII bedside hearing screening, subukan ang bawat tainga nang hiwalay na may contralateral occlusion gamit ang low-volume letter-number whisper sequences; i-dokumento ang repeat performance at pass/fail trend.
- Para sa consistency ng whispered-voice screening, ituring na praktikal na pass threshold ang tamang pag-uulit ng kahit 3 sa 6 kabuuang letter-number items.
- Para sa CN IX-focused screening, suriin ang palate at uvula midline symmetry habang nagpapa-”Ah” ang pasyente at i-dokumento ang asymmetrical rise o deviation.
- Para sa CN X-focused screening, suriin ang gag response (posterior pharynx stimulation) at swallowing coordination habang mino-monitor ang aspiration-risk cues.
- Para sa CN XI screening, subukan ang sternocleidomastoid at trapezius strength laban sa resistance habang head turn, forward head push, shoulder shrug, at shoulder retraction tasks; suriin ang asymmetry o shoulder droop.
- Para sa CN XII screening, suriin ang tongue protrusion para sa midline deviation/unilateral weakness at gumamit ng cheek-resisted tongue push para matukoy ang focal motor deficit.
- Gamitin ang CN expected-vs-unexpected mapping sa interpretasyon: CN I anosmia; CN II acuity/field loss; CN IV/VI gaze-limitation na may diplopia/ptosis pattern; CN VII facial asymmetry o taste loss; CN IX/X absent gag o dysphagia/speech change; CN XI shoulder-turn weakness; CN XII tongue deviation from midline.
- Sa pupillary testing, ihambing ang parehong pupils para sa symmetry at reactivity (karaniwang mga 2-5 mm range); suriin ang anisocoria, sluggish response, o nystagmus bilang abnormal cues na nangangailangan ng escalation context.
- Suriin ang accommodation/convergence sa paglipat ng visual focus mula near papuntang far target at kumpirmahin ang inaasahang pupillary constriction (near) na may dilation (far).
- Suriin ang memory at mood sa interview (halimbawa agitation, anger, depression, euphoria) at kung congruent ang affect sa konteksto.
- Suriin ang cranial-nerve function na may side-to-side comparison ng symmetry ng mukha/leeg; pagsamahin ang related testing kung angkop (halimbawa CN III/IV/VI eye-movement assessment).
- Suriin ang motor strength at symmetry sa upper at lower extremities gamit ang resistance testing.
- Gumamit ng bilateral bedside strength maneuvers (sabay na handgrip, forearm pull laban sa resistance, seated lower-leg pull, hip flexion lift laban sa resistance, ankle dorsiflexion/plantar-flexion resistance) at i-dokumento ang side-to-side asymmetry.
- Maingat na i-interpret ang bahagyang dominant-side strength advantage at mag-escalate kapag malinaw na disproportionate o progresibong lumalala ang asymmetry.
- Suriin ang sensory function na eyes closed at cue-neutral prompts; subukan ang light touch at sharp/dull discrimination sa pangunahing extremity regions at torso kapag indicated.
- Para sa dermatomal screening, subukan muna ang representative distal skin regions sa halip na lahat ng surface area sa routine exams; palawakin tungo sa focused dermatome mapping kapag may numbness, weakness, o focal deficits.
- Kung hindi nadedetect ang light touch at kailangan ang advanced assessment, mag-escalate sa supervised higher-intensity sensory checks (halimbawa cold o pin-prick methods) ayon sa protocol.
- I-grade ang motor strength sa 1-5 scale sa shoulders, elbows, wrists, hips, knees, at ankles; suriin ang tone sa pamamagitan ng passive range of motion at tukuyin ang hypotonia versus hypertonia.
- Obserbahan ang involuntary motor findings (tics, tremors, myoclonus) at i-dokumento ang movement symmetry/coordination.
- Suriin ang cerebellar function gamit ang gait/posture screening at focused coordination tests (finger-to-nose, heel-to-shin, rapid alternating hand movements).
- Para sa cerebellar gait screening, suriin ang 10-foot walk na may pivot/return, heel-to-toe walk, tiptoe walk, at heel walk; abnormal cues ang shuffling, jerky steps, balance loss, o arm-swing incoordination.
- Suriin ang pronator drift para sa banayad na upper-limb weakness: eyes closed, arms extended sa shoulder level na nakataas ang palad sa loob ng 20-30 seconds; abnormal ang pronation o pababang drift.
- Para sa gait-coordination screening, isama ang short-distance ambulation na may pivot/return, heel-to-toe walk, toe walk, at heel walk; i-dokumento ang shuffling, jerky movement, arm-swing asymmetry, o balance loss.
- Para sa finger-to-nose testing, ipa-extend sa pasyente ang parehong braso, isara ang mata ayon sa utos, at salit-salitang hawakan ang dulo ng ilong kanan/kaliwa bago bumalik sa extension; tandaan ang overshoot, tremor, o side-dominant dysmetria.
- Para sa heel-to-shin testing, ihiga ang pasyente at ipatapat ang bawat sakong mula sa opposite knee pababa sa ankle nang tuwid at makinis; abnormal ang heel drop-off o irregular tracking.
- Gamitin ang Romberg testing kapag angkop (magkadikit ang paa, eyes closed) na may close guarding para sa fall prevention; abnormal ang positive sway o pagkawala ng balanse.
- Sa routine RN neurologic exams, karaniwang limitado ang auscultation; kapag may advanced assessments na nakatukoy ng carotid bruits, ituring ito bilang posibleng cerebral blood-flow warning cues.
- Iugnay ang reflex findings (halimbawa deep tendon at Babinski patterns) sa kabuuang neurologic context at provider-reported exam findings.
- Gamitin nang tama ang reflex exam context: maaaring hindi kasama sa routine adult RN neuro checks ang full tendon-reflex panels, ngunit karaniwang kasama ito sa specialty o advanced assessments.
- Kapag sinusuri ang deep tendon reflexes, gamitin ang standard 0-4+ grading (
2+expected):0absent,1+hypoactive,3+hyperactive without clonus,4+hyperactive with clonus; ulitin pagkatapos makapag-relax bago kumpirmahin ang weak/absent responses. - Kapag kailangan ang localization detail, i-map ang reflexes ayon sa segment: brachioradialis (C5-C6), triceps (C6-C7), patellar (L2-L4), at plantar/Babinski pathway (L5-S1 context).
- I-interpret ang Babinski ayon sa age context: maaaring expected ang extensor response sa children under about 2 years, samantalang abnormal ang persistent extensor response sa older children/adults.
- Suriin ang cortical sensory processing gamit ang stereognosis sa paglalagay ng pamilyar na object sa bawat kamay (eyes closed) at pagpapakilala ng object.
- Magdagdag ng graphesthesia kapag kailangan ang cortical-sensory detail sa pag-trace ng number o letter sa palad at pagpapakilala nito na eyes closed.
- Suriin ang psychosocial response sa neurologic illness at coping capacity dahil binabago ng anxiety, role disruption, at function loss ang adherence at kaligtasan.
- Bago ang language/communication testing, kumpirmahin ang baseline sensory supports (halimbawa hearing aids o salamin) upang maiwasan ang false-positive aphasia findings.
- Ilapat ang lifespan context sa interpretasyon: pediatric fall/head-injury vulnerability at older-adult risks tulad ng baseline atrophy, vascular change, at neurocognitive decline.
- Para sa infants at children, isaalang-alang ang developmental anatomy at kaligtasan (halimbawa anterior fontanel closure around 12-18 months, posterior fontanel closure around 2-3 months, immature thermoregulation, higher head-injury susceptibility, at motor-development-related fall risk).
- Isama ang age-expected primitive-reflex checks sa newborns at kumpirmahin ang expected disappearance windows sa infancy.
- Para sa older adults, i-interpret ang findings kasama ang expected aging changes (atrophy, reduced vascularization, neurotransmitter decline, at increased ischemic white-matter burden) habang patuloy na nag-e-escalate ng acute deviations mula sa baseline.
- Sa older adults, isaalang-alang din ang expected sensory changes (reduced near-vision focus, smaller pupils/lens changes, hearing decline, at taste-smell-touch attenuation) habang itinuturing pa ring abnormal ang abrupt changes hanggang mapatunayang iba.
- Sa older adults, isaalang-alang din ang motor-aging patterns (reduced muscle mass/velocity, proprioceptive decline, osteoarthritis burden, at medication-related dizziness) kapag inihihiwalay ang expected slowing mula sa acute neurologic decline.
- Isama ang contributory screening labs kapag clinically indicated (halimbawa CBC, nutrition-related markers, BMP/electrolytes/glucose, ABG, toxicology, at infection cultures).
Mga Interbensyon sa Pag-aalaga
- I-activate ang urgent response para sa BEFAST-positive findings o biglaang focal neurologic changes.
- Gamitin nang pare-pareho ang NIHSS/BEFAST-style stroke screening prompts at ituring na time-critical ang positive findings.
- Magsagawa ng repeat focused neurologic checks sa ordered intervals at agad na ipaalam ang trend changes.
- Bawasan ang injury risk sa pamamagitan ng fall precautions, aspiration precautions, at communication support strategies.
- Ipatupad ang environment-based injury prevention para sa neurologic deficits (halimbawa clutter control, call-light access, supervised ambulation, at alarm/assistance strategies ayon sa risk level).
- I-dokumento nang malinaw ang ginamit na assessment tools, baseline findings, at kasunod na trend changes upang maaasahang maikumpara sa paglipas ng panahon ang progression o recovery.
Time-Sensitive Neurologic Decline
Ang bagong unilateral weakness, speech changes, o bumababang consciousness ay maaaring tanda ng mabilis na umuunlad na stroke o intracranial pathology.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| [anticonvulsants] | Levetiracetam-class contexts | I-monitor ang breakthrough events at postictal recovery trends. |
| [thrombolytics] | Acute ischemic stroke contexts | Ipatupad ang mahigpit na time-window at neurologic-monitoring protocols. |
Aplikasyon ng Clinical Judgment
Clinical Scenario
Nag-uulat ang isang pasyente ng biglaang pagkahilo at may facial asymmetry na may bagong slurred speech sa routine assessment.
- Recognize Cues: Acute focal deficits at pagbabago sa komunikasyon.
- Analyze Cues: Mataas ang concern na cerebrovascular event ang findings.
- Prioritize Hypotheses: Pinakamataas na prayoridad ang agarang pag-activate ng stroke pathway.
- Generate Solutions: Simulan ang emergency escalation at kumuha ng focused neurologic baseline documentation.
- Take Action: I-activate ang rapid response ayon sa protocol at ipagpatuloy ang madalas na reassessment.
- Evaluate Outcomes: Nababawasan ang time-to-treatment at ang panganib ng neurologic decline.
Mga Kaugnay na Konsepto
- neurological system - Konteksto ng core anatomy at function para sa exam interpretation.
- neuromuscular diagnostic testing - Objective testing pathways pagkatapos ng bedside screening.
- neurological diagnostic testing at nursing considerations - Balangkas para sa neuroimaging, CSF, electrophysiology, at procedural nursing prep.
- assisting with sensory deficits - Safety adaptation para sa persistent sensory deficits.
- documenting at reporting data - Ang trend-based neurological documentation ay sumusuporta sa ligtas na escalation.
Sariling Pagsusuri
- Aling neurologic findings ang dapat mag-trigger ng agarang BEFAST-based escalation?
- Bakit mahalaga ang bilateral comparison sa cranial-nerve at motor testing?
- Paano pinapahusay ng serial reassessment ang kaligtasan sa pinaghihinalaang neurologic decline?