Pagsusuri ng Bibig, Lalamunan, Ilong, at Sinus at mga Abnormalidad
Mahahalagang Punto
- Pinagsasama ng oral, pharyngeal, nasal, at sinus assessment ang symptom interview at structured inspection/palpation.
- Ang pananakit sa paglunok, pagbabago ng boses, airway symptoms, at persistent lesions ay priority cues para sa escalation.
- Ang pagbabago sa amoy/lasa, chronic congestion, at paulit-ulit na throat inflammation ay maaaring malaki ang epekto sa nutrisyon at kaligtasan.
- Pinapahusay ng anatomy-guided technique ang paghiwalay ng expected variation mula sa clinically significant pathology.
- Dapat makuha ng focused questioning ang prior diagnoses, kasalukuyang symptom profile, at medication/herbal use na maaaring makaapekto sa findings.
Pisyopatolohiya
Ang bibig, lalamunan, ilong, at sinuses ay bumubuo ng magkakaugnay na airway-digestive region na sumusuporta sa paghinga, paglunok, pagsasalita, pang-amoy, at panlasa. Ang inflammation, obstruction, o infection sa isang bahagi ay maaaring makaapekto sa buong functional pathway.
Dahil parehong kasangkot ang airway protection at oral intake, ang localized pathology ay maaaring mabilis na makaapekto sa respiratory safety, hydration, nutrisyon, at komunikasyon. Kasama sa oral cavity ang lips, teeth, jaws, tongue, palate, uvula, at salivary structures; malaki ang papel ng masseter at temporalis sa mastication, kaya maaaring maapektuhan ng structural o motor change ang pagnguya, pagsasalita, at intake. Ang dental plaque ay biofilm ng naiwang food debris at bacteria na maaaring mag-demineralize ng enamel sa paglipas ng panahon, na humahantong sa dental caries at pain-limited mastication. Kasama sa pharynx ang nasopharynx (air conduction na may adenoidal immune tissue), oropharynx (air-food pathway na may palatine/lingual tonsils), at laryngopharynx (shared pathway patungo sa trachea/esophagus). Sinusuportahan ng laryngeal at epiglottic function ang phonation at pinoprotektahan ang airway habang lumulunok. Kasama sa nasal structure ang external bridge/nares at internal septum, cavities, at turbinates na nagfi-filter, nagpapainit, at nagpapahumidify ng inspired air habang sumusuporta sa olfaction-gustation integration at resonance. Ang paranasal sinuses (frontal, maxillary, ethmoid, sphenoid) ay mucosa-lined, air-filled spaces na nagpapagaan ng bigat ng bungo, nakaaapekto sa quality ng boses, at tumutulong sa mucociliary defense.
Klasipikasyon
- Assessment domains: Oral mucosa/dentition/tongue, pharynx at tonsils, nasal cavity/septum/turbinates, at sinus tenderness/drainage patterns.
- Oral-structure domain: Lip/dentition alignment, jaw movement, tongue mobility, palate/uvula position, at salivary moisture pattern.
- Pharyngeal domain: Nasopharynx-oropharynx-laryngopharynx function na may tonsillar at airway-protection relevance.
- Nasal-sinus domain: Septum/turbinate patency at paranasal-sinus pattern (frontal, maxillary, ethmoid, sphenoid).
- Abnormality groups: Infectious-inflammatory, structural/congenital, neoplastic warning patterns, at airway-urgent conditions.
- Symptom-risk class: Mild local irritation versus hirap lumunok, dyspnea, muffled voice, o progressive pain/swelling.
- Age-related sensory-change class: Maaaring magpakita ang older adults ng reduced smell discrimination at diminished taste sensitivity na maaaring makaapekto sa gana, kaligtasan, at medication tolerance.
Pagsusuri sa Pag-aalaga
Pokus sa NCLEX
Unahin ang airway at swallowing safety cues bago ang lower-acuity na chronic comfort complaints.
- Suriin ang sore throat, hirap lumunok, hoarseness, oral pain, congestion, sinus pressure, pagbabago sa amoy/lasa, at bleeding.
- Suriin ang progression ng plaque-caries pattern (pananakit habang ngumunguya, visible decay, thermal sensitivity, at pagbawas ng intake dahil sa oral discomfort).
- Suriin ang dental-caries risk profile (halimbawa tobacco use, diabetes, madalas na high-sugar/high-carbohydrate intake, older age, at dry mouth).
- Kapag may hinala ng oral cancer, suriin ang loose teeth, hindi naghihilom na sugat sa labi/bibig, red-white mucosal patches, bukol sa panga/leeg, mouth-ear pain, hoarseness, at hirap sa pagnguya/paglunok/paggalaw ng panga.
- Gumamit ng focused interview prompts para sa prior oral/throat/nasal diagnoses (halimbawa tooth decay, gingivitis, oral candidiasis, strep throat, tonsillitis, pharyngitis, GERD, sinusitis, rhinitis, polyps, septal deviation, nasal trauma).
- Suriin ang kasalukuyang medications, supplements, at herbs na ginagamit para sa sore throat, oral lesions, congestion, o allergies.
- Para sa active symptoms, ilapat ang PQRSTU clarification at isama ang oral-specific questions: gum bleeding, loose/sensitive teeth, denture fit, persistent halitosis, at chewing-related intake change.
- Maingat na i-dokumento ang lesion chronology (onset, persistence, growth/bleeding change, pain pattern) at i-report agad ang persistent na concerning findings.
- I-inspect ang oral cavity at throat para sa ulcers, plaques, exudate, asymmetry, mucosal color change, at lesion persistence.
- I-inspect ang lips/teeth/gums, palate/uvula alignment, tongue mobility, at saliva quality upang matukoy ang chewing/swallowing risk.
- Suriin ang jaw movement at i-palpate ang major mastication-muscle function kapag may iniuulat na chewing pain o oral-mechanics concerns.
- Suriin ang tonsillar size/exudate pattern, nasal patency at septal alignment, at sinus tenderness.
- I-screen ang oral candidiasis risk factors sa adults (halimbawa dentures, diabetes, cancer, HIV/AIDS, recent antibiotics, inhaled corticosteroids, xerostomia, at smoking).
- I-screen ang poor oral-health patterns: persistent halitosis, visible decay, bleeding/receding gums, tooth sensitivity o mobility, persistent toothache, xerostomia, o persistent foul taste.
- Ipagaya sa pasyente ang pagbigkas ng “Ah” habang gumagamit ng ilaw at tongue blade para mapahusay ang posterior-pharynx view at masuri ang symmetric uvular rise.
- I-retract ang lips/cheeks gamit ang gloved technique upang ganap na ma-inspect ang gingiva at dentition; alisin ang dentures upang ma-inspect ang underlying mucosa.
- I-evaluate ang loose teeth, gum-margin ulceration/bleeding, tongue coating/lesions/motion, at salivary-gland tenderness (parotid at submandibular regions).
- I-inspect ang external nose at gumamit ng speculum na may ilaw para sa intranasal assessment, kabilang ang drainage, septal deviation/perforation/bleeding, at turbinate congestion/polyps.
- I-palpate ang nasal bridge/sinus regions (forehead at cheeks) para sa tenderness, deformity, o crepitus kapag pinaghihinalaan ang fracture o sinus inflammation.
- Kung hindi tiyak ang swallowing safety (halimbawa recent stroke), kumpletuhin ang bedside swallow screening ayon sa policy bago oral intake o oral medications.
- Ituring ang failed swallow screening bilang
NPOhanggang makumpleto ang speech/swallow evaluation. - Iugnay ang pagbabago ng voice resonance at “stopped-up” quality sa posibleng mucosal swelling o sinus-obstruction pattern.
- Ihiwalay ang common upper-airway disorders: sinusitis (acute hanggang 4 weeks, chronic lampas 12 weeks, recurrent ilang episodes bawat taon), pharyngitis, tonsillitis, at epistaxis.
- I-screen ang epistaxis contributors tulad ng dry low-humidity conditions, digital trauma, anatomic deformity, hypertension, clotting disorders, at antiplatelet/anticoagulant use.
- I-validate ang findings gamit ang repeat exam at symptom clarification kapag magkasalungat ang objective at subjective data.
- I-dokumento nang malinaw ang parehong patient-reported data at objective findings, pinananatili ang direct symptom quotes kapag clinically relevant.
Mga Interbensyon sa Pag-aalaga
- Mag-escalate ng red flags tulad ng airway distress, severe hirap lumunok, epiglottitis-like presentation, o nonhealing suspicious lesions.
- Suportahan ang ordered oral-cancer workup pathways, na maaaring kabilang ang endoscopy, tissue biopsy/brush-biopsy, HPV testing, x-ray/CT/MRI/ultrasound/PET imaging, at selected swallow studies.
- Suportahan ang oral hygiene, hydration, at symptom-relief strategies habang hinihintay ang definitive treatment.
- Patibayin ang caries-prevention bundle: magsipilyo dalawang beses kada araw gamit ang fluoride toothpaste, mag-floss araw-araw, palitan ang toothbrush mga bawat 3-4 months, at mag-follow-up sa routine dental care (karaniwang bawat 6 months).
- Patibayin ang fluoride at nutrition counseling (halimbawa paggamit ng fluoridated water at lower-sugar dietary pattern) kasama ang smoking-cessation support.
- Ituro ang sore-throat comfort measures: warm salt-water gargles (1/2 tsp salt sa 1 cup water), soothing liquids, throat lozenges, humidified air, at acetaminophen kapag naaangkop.
- Patibayin ang organism-specific treatment logic: karamihan ng pharyngitis ay viral at symptom-directed, ngunit ang pinaghihinalaang group A streptococcal disease at bacterial tonsillitis ay nangangailangan ng antibiotic adherence upang mabawasan ang komplikasyon.
- Patibayin ang oral-candidiasis care: antifungal adherence, masusing oral hygiene, at pagwawasto ng underlying contributors.
- Para sa mga pasyenteng gumagamit ng inhaled corticosteroids, ituro ang rinse-and-spit mouth care pagkatapos ng bawat dose upang mabawasan ang recurrent oral-thrush risk.
- Mag-refer para sa dental evaluation kapag nagpapakita ang assessment ng posibleng oral disease o progressive dentition/gingival dysfunction.
- I-report agad ang methamphetamine-associated oral-destruction patterns at i-coordinate ang dental referral at substance-use-treatment evaluation.
- Ituro ang first aid para sa epistaxis: yumuko pasulong at pigain nang tuloy-tuloy ang lateral nose hanggang 15 minutes habang humihinga sa bibig; agarang mag-escalate para sa persistent bleeding o instability.
- Para sa persistent epistaxis, maghanda para sa stepped interventions (topical vasoconstrictor, cautery, packing/balloon) ayon sa orders at i-monitor ang hemodynamic status.
- Patibayin ang infection-control measures at patient education para sa recurrence prevention at follow-up.
- Sa oral-cancer treatment trajectories, unahin ang airway at nutrition support, pain management, at communication adaptations (halimbawa written communication aids pagkatapos ng major oral procedures).
- Patibayin ang prevention education sa at-risk profiles: pagtigil sa tobacco at alcohol, balanced diet support, at lip sun-protection counseling.
Panganib sa Kaligtasan ng Upper Airway
Ang progresibong throat swelling o painful swallowing na may respiratory change ay maaaring magpahiwatig ng time-sensitive airway emergency.
Karaniwang Findings sa Bibig
- Oral ulcer: Masakit na lesions sa lips, tongue, gums, o buccal mucosa; isaalang-alang ang infectious o inflammatory causes.
- Dental plaque and caries pattern: Ang plaque accumulation ay maaaring mag-demineralize ng enamel at magdulot ng cavities, oral pain, chewing difficulty, pagbaba ng hydration/nutrisyon, at visible-esthetic distress na nakaaapekto sa self-esteem.
- Leukoplakia: Makakapal na puting patches na maaaring sumalamin sa chronic irritation, fungal process, o precancerous change.
- Erythroplakia: Persistent red patches na may mas mataas na concern para sa dysplasia/malignancy, na nangangailangan ng agarang evaluation.
- Oral candidiasis (thrush): Mga puting plaque na kadalasang natatanggal sa pagkayod; mas karaniwan sa immunocompromise o disrupted oral flora.
- Meth mouth pattern: Malubhang caries, cracked/worn teeth, gum-line decay progression, xerostomia, at oral burns/lesions na kaugnay ng methamphetamine exposure at delayed dental care.
- Oral cancer concern pattern: Nonhealing lesions, mucosal bleeding, color change, o oral-floor/tongue masses ay nangangailangan ng agarang diagnostic follow-up.
- Oral-cancer timing cue: Anumang oral lesion na nagpapatuloy ng 2 weeks o mas matagal, lalo na kung may unusual color o bleeding, ay nangangailangan ng expedited evaluation.
- Oral-cancer treatment context: Maaaring kabilang sa management ang surgery, radiation, chemotherapy, at reconstructive pathways; sa advanced disease maaaring kailanganin ang tracheostomy at feeding-tube support.
- Cleft lip / cleft palate: Congenital fusion defects na maaaring makasagabal sa feeding mechanics; lalo na sa cleft palate tumataas ang infant malnutrition risk kung walang supportive feeding strategy at definitive repair.
- Poor oral-health cluster: Halitosis, caries, gingival bleeding/recession, dry mouth, at persistent foul taste ay nagmumungkahi ng hygiene o periodontal pathology na nangangailangan ng follow-up.
Karaniwang Findings sa Lalamunan
- Enlarged tonsils: Maaaring sumalamin sa acute/recurrent infection o chronic inflammation.
- Tonsil groups: Palatine, pharyngeal (adenoids), lingual, at tubal tonsils.
- Tonsil grading:
0(post-tonsillectomy),1+normal,2+mild enlargement,3+moderate enlargement,4+severe enlargement.
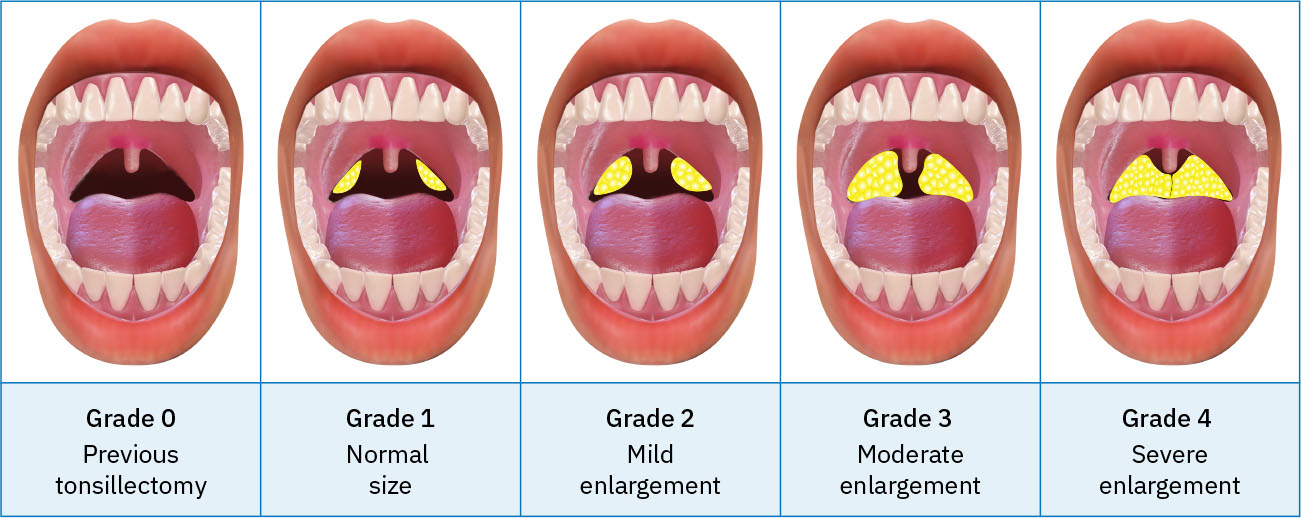 Illustration reference: OpenStax Clinical Nursing Skills Ch.22.4.
Illustration reference: OpenStax Clinical Nursing Skills Ch.22.4.
- Tonsillar exudate: Maaaring magpahiwatig ang white/yellow exudate ng bacterial pharyngotonsillar infection, kabilang ang group A streptococcal disease.
- Pharyngitis pattern: Viral o bacterial; ang streptococcal pattern na may fever, tonsillar patches, at node enlargement ay nangangailangan ng napapanahong antibiotic therapy upang mabawasan ang komplikasyon.
- Peritonsillar abscess: Severe sore throat, dysphagia, at voice change mula sa peritonsillar pus collection; kailangan ang urgent escalation.
- Laryngitis / epiglottitis: Ang hoarseness at pagkawala ng boses ay senyales ng laryngeal inflammation; ang epiglottitis signs (painful swallowing, muffled voice, breathing difficulty) ay airway emergencies.
- GERD-related throat irritation: Ang chronic reflux ay maaaring magpanatili ng cough, hoarseness, at throat discomfort.
- Throat-cancer warning pattern: Persistent throat pain, dysphagia, o progressive voice change ay nangangailangan ng expedited workup.
- Dysphagia cue cluster: Coughing habang kumakain/umiinom, wet/gurgly voice, prolonged chewing/swallowing effort, oral leakage, retained food, o breathing difficulty pagkatapos kumain.
Karaniwang Findings sa Ilong at Sinus
- Epistaxis contributors: Dry mucosa, trauma/irritants, decongestant overuse, anticoagulant/antiplatelet exposure, hypertension, polyps, at foreign bodies.
- Deviated septum: Unilateral obstruction/congestion, recurrent impeksiyon sa sinus, epistaxis, at sleep-disordered breathing; sa severe cases maaaring kailangan ng septoplasty.
- Sinusitis: Acute (hanggang 4 weeks), chronic (lampas 12 weeks), o recurrent (maraming episodes kada taon) na may congestion, facial pain/tenderness, at postnasal drip.
- Other nasal abnormalities: Nasal polyps, allergic/nonallergic rhinitis, fracture-related deformity, persistent obstruction/discharge, at congenital o acquired deformities.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| [antibiotics] | Condition-targeted agents | Kumpirmahin ang indication at i-monitor ang paglala sa kabila ng treatment. |
| [anticoagulants] | Warfarin and related agents | Suriin ang bleeding-risk history at i-monitor ang persistent o recurrent epistaxis. |
| antifungal-medications(antifungal na gamot) | Clotrimazole, miconazole, nystatin | Karaniwang ginagamit para sa candidal lesions; patibayin ang course completion at oral care. |
Aplikasyon ng Clinical Judgment
Clinical Scenario
Nag-uulat ang isang pasyente ng severe sore throat, muffled voice, painful swallowing, at lumalalang discomfort sa leeg.
- Recognize Cues: Pinagsamang upper-airway at swallowing red flags.
- Analyze Cues: Ipinapahiwatig ng pattern ang potensyal na urgent na airway-involved pharyngeal process.
- Prioritize Hypotheses: Agarang prayoridad ang airway safety at mabilis na escalation.
- Generate Solutions: Simulan ang urgent reassessment at iwasan ang pagkaantala sa provider evaluation.
- Take Action: Ipaabot nang malinaw ang objective findings at ipatupad ang ordered safety measures.
- Evaluate Outcomes: Ang maagang escalation ay pumipigil sa respiratory compromise at progression ng komplikasyon.
Mga Kaugnay na Konsepto
- oral, perineal, at catheter hygiene infection prevention - Nakaaapekto ang kalidad ng oral care sa mucosal integrity at infection risk.
- infectious at inflammatory skin conditions - Magkakatulad na principles sa pagkilala ng infectious at inflammatory patterns.
- documenting at reporting data - Pinapabuti ng objective lesion at symptom documentation ang escalation decisions.
- healthcare-associated infections - Sinusuportahan ng infection-prevention strategy ang mas ligtas na care sa iba’t ibang setting.
- respiratory system - Ang upper-airway anatomy at physiology ay nagbibigay ng konteksto para sa sinus, pharyngeal, at nasal abnormalities.
- aspiration pneumonia - Ang swallow safety screening at maagang aspiration-risk detection ay nagpapababa ng pulmonary complications.
Sariling Pagsusuri
- Aling mouth/throat findings ang nagpapahiwatig ng agarang airway-risk escalation?
- Bakit nangangailangan ng maingat na follow-up documentation ang persistent oral lesions?
- Paano makaaapekto ang nasal at sinus findings sa mas malawak na nutrition at safety outcomes?