Temporomandibular Disorders
Key Points
- TMD is a group of disorders affecting jaw-joint or jaw-muscle function and can significantly disrupt chewing and speech comfort.
- Etiology is multifactorial and may include stress, genetic predisposition, jaw trauma, teeth grinding, and inflammatory joint disease.
- Common cues include jaw/facial pain, limited jaw movement or locking, clicking/popping, and bite-alignment change.
- Focused history and jaw range-of-motion assessment are central first-line nursing evaluation steps.
- TMD presentations can be grouped into joint disorders, muscle disorders, and headache-associated patterns.
Pathophysiology
The temporomandibular joint is a bilateral sliding hinge between the mandible and temporal bone. TMD reflects dysfunction in joint mechanics, surrounding musculature, or related pain pathways.
Current evidence supports a multifactorial process rather than one single mechanism. Psychological/life stressors, inherited susceptibility, jaw trauma, bruxism, and inflammatory arthritic conditions can combine to trigger or sustain symptoms.
Classification
- Joint disorder pattern: Dysfunction centered on TMJ structural/mechanical movement.
- Muscle disorder pattern: Dysfunction centered on masticatory muscle tension/pain.
- Headache-associated pattern: Headache syndromes linked to TMJ dysfunction.
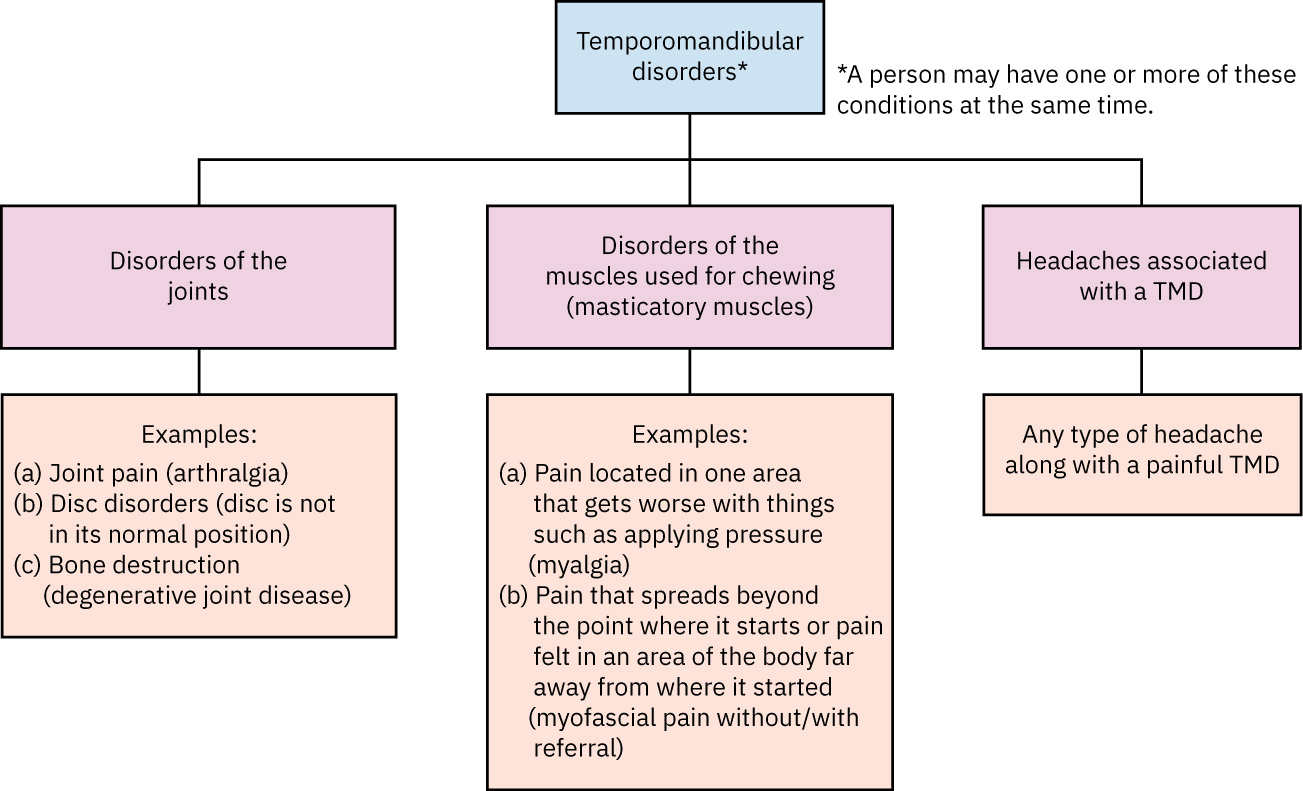 Illustration reference: OpenStax Medical-Surgical Nursing Ch.19.2.
Illustration reference: OpenStax Medical-Surgical Nursing Ch.19.2.
Nursing Assessment
NCLEX Focus
Distinguish routine jaw discomfort from function-limiting or locking patterns that need escalation.
- Assess jaw pain location, radiation (face/neck/ear), and intensity pattern.
- Assess functional impact: chewing pain, speech discomfort, locking episodes, and movement limitation.
- Assess associated mechanical cues such as jaw clicking/popping and bite-alignment change.
- Perform focused history on onset, aggravating/relieving factors, and symptom frequency.
- Assess jaw range of motion and identify provocative maneuvers.
- Assess associated symptom burden, including headache and related musculoskeletal discomfort.
- Support provider-directed diagnostics when needed (for example x-ray, CT, or MRI) to evaluate joint structure and rule out alternate causes.
Nursing Interventions
- Document focused jaw findings and symptom triggers with clear trend comparison.
- Reinforce avoidance of known aggravating behaviors while diagnostic evaluation is in progress.
- Prioritize pain-relief support and patient teaching on prevention-focused self-management.
- Reinforce stress-management strategies to reduce jaw clenching and teeth grinding behavior.
- Coordinate follow-up evaluation for persistent locking, progressive pain, or worsening functional limitation.
- Support patient education on symptom monitoring and timely reassessment.
Function-Limiting Jaw Pattern
Progressive locking or inability to open/close the jaw safely can impair nutrition and requires prompt escalation.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| Symptom-directed analgesia | Provider-directed pain regimens | Monitor pain trend and function response while definitive evaluation proceeds. |
Clinical Judgment Application
Clinical Scenario
A patient reports recurrent jaw pain radiating to the ear, morning jaw stiffness, and intermittent clicking with chewing.
- Recognize Cues: Jaw pain with functional and mechanical TMJ symptoms, plus stress-linked clenching history.
- Analyze Cues: Pattern is consistent with probable temporomandibular disorder.
- Prioritize Hypotheses: Priority is preventing functional decline and identifying persistent trigger patterns.
- Generate Solutions: Complete focused history/ROM assessment and coordinate provider-directed workup.
- Take Action: Document trigger-linked findings and escalate worsening locking or movement limitation.
- Evaluate Outcomes: Pain and function trends improve with targeted management and follow-up.
Related Concepts
- mouth-throat-nose-and-sinus-assessment-and-abnormalities - Oral-cavity and jaw assessment context.
- acute-vs-chronic-pain-and-observable-cues - Jaw-pain pattern differentiation and reassessment workflow.
- oral-care-assistance - Oral-function support considerations when pain limits self-care.