National Patient Safety Goals for Nursing Care Centers
Key Points
- The Joint Commission updates National Patient Safety Goals annually using current safety data.
- Nurses should apply goals specific to their practice setting, including nursing care centers.
- Core nursing-care-center priorities are identification accuracy, medication safety, infection prevention, falls prevention, and pressure-injury prevention.
- Goal implementation depends on consistent workflows, documentation, and patient/caregiver teaching.
- Goal sets are setting-specific across multiple care environments, so teams should validate the active version for their service line annually.
Pathophysiology
NPSG is a systems-safety framework that targets high-frequency, high-harm failure points in care delivery. In nursing care centers, harm often clusters around identification mistakes, medication communication gaps, infections, falls, and skin breakdown.
Using standardized goal-based practices lowers preventable injury risk and improves continuity across handoffs, transfers, and outpatient follow-up.
Classification
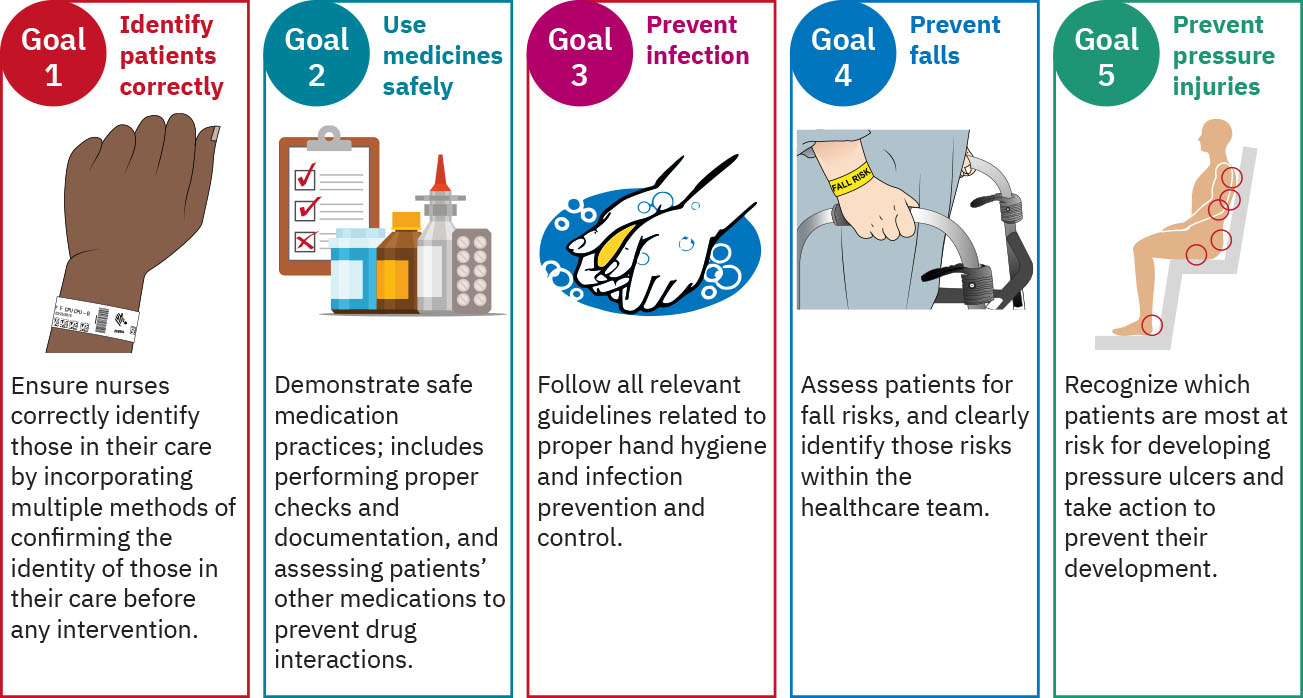 Illustration reference: OpenStax Fundamentals of Nursing Ch.9.1.
Illustration reference: OpenStax Fundamentals of Nursing Ch.9.1.
- Identify residents correctly: Use at least two identifiers before care, medication, and treatment.
- Two-identifier confirmation options: Verbal identifiers (name/date of birth) plus second-source verification (wristband scan/chart/MAR photo/staff or family confirmation when the patient cannot self-identify).
- Use medicines safely: Apply high-risk medication safeguards and reconcile medications across transitions.
- Prevent infection: Follow CDC/WHO hand-hygiene guidance and track improvement.
- Prevent falls: Identify high-risk residents and implement fall precautions.
- Prevent pressure injuries: Identify at-risk residents, apply prevention bundles, and reassess skin frequently.
Nursing Assessment
NCLEX Focus
NPSG questions test whether the nurse can map a safety event to the correct goal and immediate prevention action.
- Verify two-identifier compliance before interventions.
- If the patient cannot state identifiers, use policy-approved alternate verification (for example wristband scan and independent staff/family confirmation).
- Assess anticoagulant and polypharmacy risks in medication workflows.
- Assess medication-list accuracy at admission, transfer, and return visits.
- Assess hand-hygiene adherence and infection-risk patterns.
- Assess fall risk factors (for example weakness, dizziness, sedating medications).
- Assess pressure-injury risk and current skin integrity status.
- Assess bedside safety-readiness details that prevent immediate harm (for example allergy-band visibility when indicated, isolation-precaution signage/equipment, and call-light access with bed-low/locked setup).
Nursing Interventions
- Enforce two-identifier verification for all medications and treatments.
- Use medication reconciliation workflows and provide patients written medication lists.
- Teach residents/families to carry an updated medication list to each provider visit.
- Apply CDC/WHO hand-hygiene standards and unit-level adherence goals.
- Implement individualized fall precautions for high-risk residents.
- Use a repeatable safety sweep workflow during care rounds (identity/allergy check, bed position and side-rail strategy, call-light reachability, and line/device hazard check).
- Implement pressure-injury prevention actions and scheduled reassessment per protocol.
- Review annual NPSG updates and align unit policy/practice accordingly.
Goal-Drift Risk
When annual goal updates are not integrated into daily practice, preventable harm patterns can recur.
Pharmacology
Medication-related NPSG focus includes anticoagulant safety, complete medication reconciliation, and clear patient-facing medication instructions at transitions.
Clinical Judgment Application
Clinical Scenario
A long-term-care resident is readmitted after dizziness and a fall; medication list differs from previous discharge paperwork.
- Recognize Cues: Fall event plus medication-list discrepancy.
- Analyze Cues: NPSG gaps in falls prevention and medication safety are likely.
- Prioritize Hypotheses: Immediate risk reduction requires reconciliation and fall-prevention update.
- Generate Solutions: Complete med reconciliation, adjust precautions, reinforce two-identifier process.
- Take Action: Implement revised plan and educate resident/family.
- Evaluate Outcomes: No recurrent fall and medication list remains accurate across transitions.
Related Concepts
- organizational-culture-patient-centered-collaborative-and-safety-frameworks - System culture needed to sustain NPSG implementation.
- medication-rights-and-three-checkpoint-verification - Identification and medication-check workflow support.
- medication-regimen-management - Reconciliation and patient medication-list reliability.
- fall-prevention - Core interventions for high-risk residents.
- pressure-injury-staging-and-risk-assessment - Prevention and surveillance aligned with NPSG skin goals.
Self-Check
- Which NPSG actions are mandatory before medication administration in nursing care centers?
- Why is medication reconciliation central to NPSG medication-safety performance?
- How do fall and pressure-injury goals interact in frail residents?