ISBAR na Klinikal na Handoff Communication
Mahahalagang Punto
- Ini-standardize ng ISBAR ang urgent at routine clinical communication sa iba’t ibang team.
- Ang pagkakasunod ay Introduction, Situation, Background, Assessment, Recommendation.
- Ang istrakturadong handoff ay nagpapababa ng omissions at sumusuporta sa mas mabilis na shared understanding.
- Kapaki-pakinabang ang ISBAR para sa shift reports, interunit transfers, at escalation calls.
- Dapat unahin ng interprofessional updates ang maigsi at clinically relevant na wika upang mabawasan ang treatment delay.
- Madaling tandaan ang mnemonic at pinananatiling nakikita ang mga item na nangangailangan ng agarang atensyon sa urgent communication.
- Ang pagdagdag ng readback (ISBARR) ay nagpapalakas sa handoff reliability sa high-risk transitions.
- Nakaayon ang ISBARR sa QSEN teamwork/collaboration competency at Joint Commission communication-focused patient-safety goals.
- Maaaring gamitin ang I-PASS bilang complementary structure para sa interprofessional handoff, lalo na kung inaasahan ang explicit synthesis ng receiver.
- Pinapabuti ng bedside handoff na may client inclusion ang continuity, safety, at nurse/client satisfaction kapag pinananatili ang privacy safeguards.
- Kinikilala ang inadequate handoff communication bilang severe-harm risk, kaya ang standardized structure at readback ay mga core safety controls.
- Ang handoff ay real-time transfer at acceptance ng responsibilidad sa care, hindi lang one-way information report.
- Dapat destination-focused ang transfer report upang makuha ng receiving team ang pinaka-actionable data para sa acuity level na iyon.
- Sa perioperative handoff, dapat malinaw na kumpirmahin ang patient-verified procedure/laterality, surgeon site marking, at allergy reaction profile upang mabawasan ang wrong-site risk.
- Sa emergency-trauma pathways, pagsamahin ang EMS prearrival update at bedside ISBAR handoff upang mabawasan ang setup at transfer omissions.
Kagamitan
- Updated na patient chart at kasalukuyang vital/lab trends
- Unit handoff template o ISBAR prompt card
- Escalation contact pathway para sa recommendation follow-through
Mga Hakbang sa Pamamaraan
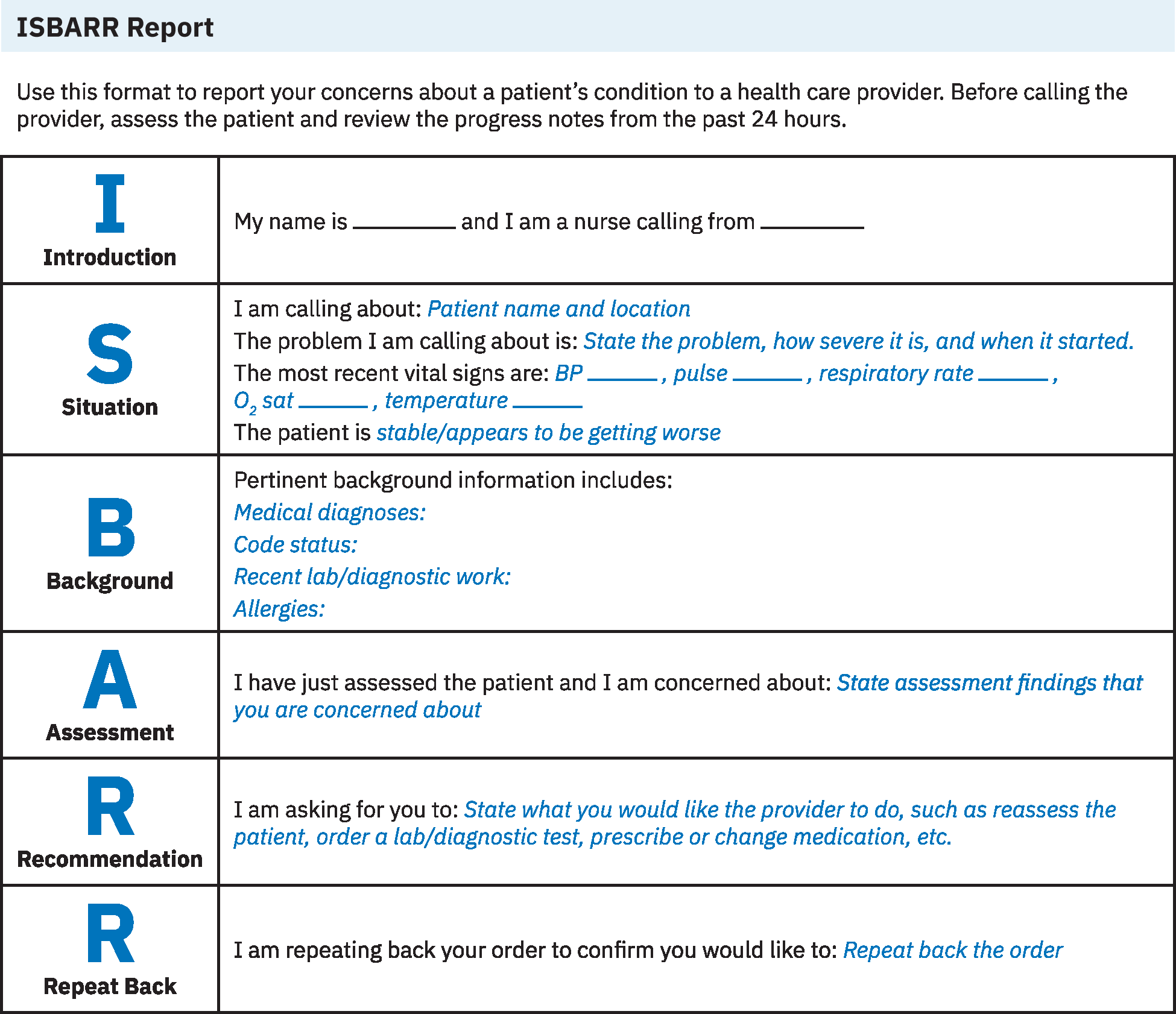 Illustration reference: OpenStax Fundamentals of Nursing Ch.8.2.
Illustration reference: OpenStax Fundamentals of Nursing Ch.8.2.
- Introduction: Tukuyin ang iyong sarili, role, unit, at patient identifiers.
- Situation: Sabihin ang agarang dahilan ng communication, urgency level, current status, at recent vital-sign trend.
- Background: Magbigay ng maigsi ngunit relevant na history, admitting context, code status, allergies, recent interventions, at key lab/diagnostic findings.
- Assessment: Iulat ang kasalukuyang clinical interpretation gamit ang objective at subjective cues.
- Recommendation: Tukuyin ang hinihiling na action, timeframe, at contingency kung lalala ang status.
- Kumpirmahin ang transfer at acceptance ng care responsibility at hilingin sa receiver na ulitin ang key plan elements.
- Magdagdag ng malinaw na readback confirmation para sa high-risk transfer details (code status, lines, wounds, pending tasks).
- Para sa verbal provider orders, gawin ang full closed-loop sequence: i-read back ang order, isagawa ang action, pagkatapos ay sabihin na nakumpleto ito.
- Bago ang escalation calls, kumpletuhin ang pre-call preparation: direct patient assessment, current-order/protocol review, recent provider at nursing-note review, at charge-nurse consult kung kinakailangan.
- Bago tumawag, ihanda agad ang high-yield data (admitting diagnosis/date, code status, allergies, recent vitals/labs, current medications/IV fluids, at active oxygen device/flow rate kapag ginagamit).
- Sa call planning, malinaw na sabihin ang inaasahang outcome/request, pagkatapos ay idokumento kung sino ang kinontak, eksaktong oras ng tawag, at buod ng impormasyong ibinahagi/natanggap kaagad pagkatapos ng tawag.
- Sa admission-related handoff, malinaw na tukuyin ang present-on-admission findings (halimbawa existing pressure injury o skin wound) at legal decision-maker status upang maiwasan ang safety, documentation, at reimbursement errors.
- Para sa interfacility transfer kung magkaiba ang charting systems, muling banggitin nang malinaw ang critical lines/drains/wounds/active therapies sa halip na umasa na may EHR access ang receiving team.
- Kung gumagamit ang unit ninyo ng I-PASS, i-verify ang illness severity, patient summary, action list, situation awareness/contingency planning, at synthesis by receiver.
- Para sa shift-to-shift bedside handoff, isama ang client, off-going nurse, at oncoming nurse nang real time; isama lamang ang family kung may pahintulot ng client at HIPAA-safe setup.
- Sa bedside handoff assessment exchange, isama ang baseline head-to-toe findings, current lines/tubes/drains, at recent changes sa medications, labs, diagnostics, at treatments.
- Sa structured handoff, tiyaking naililipat ang minimum critical-content: sender contact information, illness-severity framing, concise hospital-course summary, to-do list, contingency plans, allergies, code status, medication list, recent labs, at recent vital signs.
- Idokumento ang handoff content, actions requested, at response timeline.
- Para sa PACU-to-inpatient transfer, isama ang minimum dataset elements: full identifiers (kabilang ang medical ID), code status at allergies, procedure at anesthesia type/duration, current vital trend, IV medications/fluids at blood products, urine output, drain output, incision/dressing status, intraoperative complications, baseline versus current orientation/LOC, mobility restrictions, language/sensory support needs, family/decision-maker context, pending tests/procedures, at current low-hemoglobin o hemodynamic management plan.
- Para sa interagency transfer, gamitin ang receiving-facility checklist requirements at magpadala ng expanded continuity details na lampas sa unit-to-unit handoff minimums.
- Para sa preop-to-OR transfer, i-verify kasama ang pasyente at receiving nurse ang: full identifiers, procedure at laterality, consent alignment, surgeon-marked site, allergy band/reaction symptoms, at accompanying family-contact details kapag naaangkop.
- Sa PACU discharge o unit transfer calls, malinaw na iulat ang readiness criteria status: vital-sign stability, effective pain control, return to baseline alertness/orientation, voiding status, at safe ambulation plan.
- Sa emergency-trauma intake, isama ang prearrival EMS briefing sa maagang ISBAR preparation, pagkatapos ay kumpletuhin ang mas malawak na secondary-survey handoff pagkatapos ng stabilization.
- Kung walang available na definitive specialty services sa lokal na setting (halimbawa burn, stroke, o maternal-neonatal specialty care), gamitin ang ISBAR upang i-coordinate ang napapanahong escalation at transfer sa angkop na pasilidad.
Karaniwang Pagkakamali
- Pagbibigay ng hindi istrakturadong narrative nang walang recommendation → delayed action.
- Hindi pagsama ng key background risks → hindi kumpletong clinical context.
- Pagkabigong gawin ang closed-loop confirmation → misunderstandings sa transition points.
- Paglaktaw sa synthesis by receiver → hindi nabeberipikang plan at mas mataas na handoff error risk.
- Walang dokumentasyon ng handoff at requests → mahinang accountability trail.
- Ang inadequate handoff ay maaaring mag-ambag sa severe harm events (halimbawa treatment delay, falls, medication errors, at wrong-site events).
Kaugnay
- continuity of care sa evaluation phase - Sinusuportahan ng ISBAR ang ligtas na care transitions.
- mga prinsipyo ng ANA nursing documentation - Nakasalalay ang handoff quality sa tumpak na source data.
- workflow ng source vs problem-oriented documentation - Naaapektuhan ng documentation structure ang linaw ng handoff.
- leadership attributes at competencies sa nursing - Ang leadership behaviors ang nagtutulak sa maaasahang team communication sa transitions.