Mental Health sa Homeless at Displaced na Populasyon
Mahahalagang Punto
- Ang housing instability ay parehong sanhi at bunga ng mental illness at substance-use disorders.
- Kabilang sa barriers ang poverty, discrimination, legal entanglement, limitadong services, at psychosocial trauma burden.
- Nangangailangan ang recovery-oriented approaches ng coordinated housing, health, behavioral health, at social support systems.
- Kritikal na connectors ang mga nars para sa assessment, referral, advocacy, at cross-sector collaboration.
- Bidirectional ang ugnayan ng homelessness at health: maaaring magdulot ng homelessness ang health problems, maaaring magdulot ng illness ang homelessness, at maaaring humarang ang homelessness sa epektibong treatment.
- Maaaring magpababa ng emergency visits at hospitalizations sa unhoused populations ang low-threshold integrated medical-home models.
- Pinapabuti ng person-centered terminology (halimbawa preferences sa unhoused/houseless) at nonstigmatizing communication ang trust at engagement.
- Nangangailangan ng iniangkop na outreach ang veterans, families na may children, at rural communities dahil magkakaiba ang barrier patterns at local resources.
- Madalas pinagsasabay sa community-based nursing encounters ang mental-health support at practical frontline care (halimbawa wound care, immunizations, at basic screening) upang ma-stabilize ang engagement.
- Itinatampok ng point-in-time estimates sa source context na ito ang malaking unsheltered burden, kaya kailangan ang low-barrier outreach sa halip na clinic-only follow-up plans.
- Sa displaced populations, maaaring baguhin ng legal status differences (refugee vs asylum seeker) ang resettlement pathways at praktikal na access sa health services.
- Dapat isama ng refugee-care planning ang trauma-informed mental-health assessment kasama ng communicable-disease screening, vaccination review, at language-access support.
Patopisyolohiya
Inilalantad ng homelessness at displacement ang mga tao sa chronic stress, trauma, victimization risk, at putol-putol na care, na lahat ay nagpapalala ng psychiatric symptoms at physical health outcomes. Karaniwan ang co-occurring serious mental illness at substance-use disorders at maaaring lumikha ng paikot na instability.
Pinapahina ng paulit-ulit na housing loss ang social support at treatment continuity, na nagpapataas ng emergency utilization at nagpapababa ng long-term recovery probability kung walang integrated interventions.
Klasipikasyon
- Housing instability factors: Economic shocks, legal displacement, discrimination, at hindi sapat na affordable housing.
- Displacement-legal-status domain: Magkaiba ang refugee at asylum-seeker pathways sa legal recognition at entitlement timing, na nakaaapekto sa service access at continuity planning.
- Homelessness-contributor domain: Poverty, affordable-housing shortage, unaffordable health care, domestic violence, SUD burden, at persistent mental illness risk.
- Risk-matrix domains: Economic pressure, health burden, family conflict/violence exposure, social isolation, legal actions (eviction/foreclosure), disaster displacement, policy trends (gentrification), substance misuse, at limitadong support-service access.
- Clinical vulnerability factors: Serious mental illness, SUD, trauma exposure, at untreated comorbidity.
- Service access barriers: Transportation gaps, insurance limitations, fragmented systems, at rural scarcity.
- Clinical-access barrier cluster: Transportation limits, fragmented services, scheduling barriers, stigma, distrust, social isolation, at competing survival needs.
- Terminology-respect domain: Maaaring may magkakaibang lived meanings ang
homeless,unsheltered,unhoused, athouseless; dapat isama sa assessment ang language preference ng tao. - Special-population domain: Veteran homelessness na may PTSD/anxiety burden, family/child developmental risk habang may instability, at hidden rural homelessness na may mababang service density.
- Low-threshold medical-home model: Walk-in/flexible access, street/shelter outreach, integrated primary-mental health care, on-site sustenance supports, at intensive cross-agency care management.
Nursing Assessment
Pokus sa NCLEX
Suriin nang magkakasama ang immediate safety, housing status, at co-occurring SMI/SUD upang magabayan ang realistic care planning.
- Suriin ang kasalukuyang housing status, shelter safety, at immediate survival risks.
- Suriin ang psychiatric symptom burden, suicidality, at substance-use severity.
- Suriin ang practical disease-management feasibility sa kasalukuyang housing context (halimbawa medication storage, hygiene access, diet constraints, at wound-care follow-through).
- Suriin ang access barriers: transportation, insurance, identification documents, at service eligibility.
- Suriin ang practical care-access barriers na partikular sa homelessness (appointment-keeping feasibility, trust/distrust patterns, at immediate survival-resource needs).
- Para sa bagong displaced/refugee clients, suriin ang camp/route exposure risks (overcrowding, sanitation/water limitations, interrupted vaccination history, at delayed chronic-disease treatment).
- Tanungin ang tao kung anong housing terminology ang mas gusto niya at iwasan ang identity labels na maaaring magpataas ng stigma o disengagement.
- Suriin ang social supports, legal stressors, at naunang engagement sa community resources.
- Suriin ang readiness para sa motivational therapies at recovery-housing options.
- Suriin ang emergency-utilization pattern at repeated hospitalization risk na kaugnay ng untreated basic-needs burden.
- Suriin ang criminal-legal involvement, arrest/victimization history, at emergency-department dependence patterns na kaugnay ng housing instability.
- Suriin ang special-population needs (veteran status, family/child safety-development concerns, at rural service-access limitations).
- Suriin nang maingat ang trauma-persecution history (kabilang ang torture o sexual/gender-based violence risk) at bantayan ang somatic presentations (halimbawa headaches, abdominal pain, nonspecific pain) na maaaring nagtatago ng mental distress.
Nursing Interventions
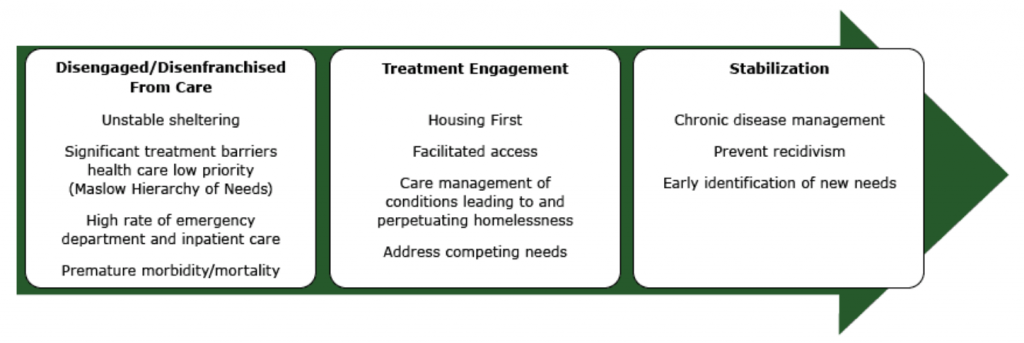 Illustration reference: OpenRN Nursing Mental Health and Community Concepts 2e Ch.17.2.
Illustration reference: OpenRN Nursing Mental Health and Community Concepts 2e Ch.17.2.
- I-coordinate ang mabilis na linkage sa housing, case management, at integrated behavioral health services.
- Gumamit ng motivational interviewing at recovery-oriented planning para sa SUD/SMI stabilization.
- Magtaguyod ng trauma-informed, low-barrier care pathways sa iba’t ibang ahensya.
- Makipagtulungan sa social work, legal aid, at public programs para sa benefits at transport access.
- Sa outreach/community settings, isama ang agarang practical care (halimbawa wound management, immunization linkage, at basic health checks) kasama ng mental-health triage upang mapabuti ang trust at follow-up.
- Gumamit ng qualified interpreters na may dialect/gender sensitivity kung posible, at malinaw na ipaliwanag ang confidentiality limits upang mabawasan ang takot na maaapektuhan ng testing results ang immigration/asylum processes.
- Suportahan ang continuity sa pamamagitan ng follow-up touchpoints at community partner communication.
- Gumamit ng low-threshold care design kung posible (walk-in capacity, outreach encounters, at same-site integrated services).
- Para sa children/families na nakararanas ng homelessness, maagang i-coordinate ang school-health at case-management linkage upang suportahan ang enrollment continuity, safety, at developmental follow-through.
- I-coordinate ang access sa immediate sustenance supports (food vouchers, hygiene kits, clothing, bus passes, at transport assistance) bilang bahagi ng clinical stabilization.
- Makipagpartner sa refugee-resettlement at specialist support agencies upang iayon ang infectious-disease screening, immunization catch-up, trauma services, at legal-social navigation.
- Ilipat ang clients sa traditional primary-care settings kapag bumuti ang housing at self-care stability, habang pinananatili ang continuity safeguards.
- Gumamit ng shelter/drop-in-center/mobile-clinic intake partnerships upang mabawasan ang first-contact barriers at mapabilis ang referral completion.
- I-refer ang eligible clients sa recovery housing programs na pinagsasama ang stable placement at counseling/support services.
- I-coordinate sa local/state/federal agencies ang funding pathways na nagpapalawak ng supportive housing, integrated SUD treatment, at rural outreach capacity.
Panganib ng Fragmentation
Madalas mabigo ang isolated referrals na walang coordinated follow-up para sa clients na humaharap sa maraming structural barriers.
Pharmacology
Nakadepende ang pagiging epektibo ng medication sa stable access, storage feasibility, at follow-up continuity. Dapat unahin ng nursing care ang practical adherence supports, regimen simplification kung posible, at integrated monitoring kasama ng outreach-based services.
Aplikasyon ng Clinical Judgment
Klinikal na Sitwasyon
Isang unhoused client na may bipolar disorder at alcohol use ang nag-uulat ng paulit-ulit na shelter loss, missed medication doses, at recurrent emergency visits.
- Recognize Cues: Kaugnay ang clinical instability sa housing at access disruption.
- Analyze Cues: Nagpapalakas sa isa’t isa ang SMI/SUD at structural barriers.
- Prioritize Hypotheses: Agarang prayoridad ang safety, housing linkage, at treatment continuity.
- Generate Solutions: Bumuo ng integrated plan kasama ang outreach psychiatry, case management, at recovery housing referral.
- Take Action: I-activate ang interdisciplinary coordination at short-interval follow-up.
- Evaluate Outcomes: Nabawasang crisis visits at mas tuloy-tuloy na medication continuity.
Mga Kaugnay na Konsepto
- mga disorder sa paggamit ng substance - Karaniwang co-occurring condition sa unstable housing contexts.
- pagharap sa adiksiyon - Mahalaga ang recovery supports para sa housing stability.
- mga pangangailangan ng komunidad sa mental health care - Social determinants framework para sa planning.
- kolaborasyon at koordinasyon ng pangangalaga - Ang cross-sector coordination ang nagtutulak ng outcomes.
- PTSD at trauma sa mga beterano - Maaaring magpataas ng homelessness risk ang veteran trauma burden at nangangailangan ng targeted referral pathways.