Healthcare Delivery Models at Organizational Structures
Mahahalagang Punto
- Nagkakaiba ang health systems ayon sa financing model, governance, at service organization.
- Kabilang sa mga karaniwang model categories ang Beveridge, Bismarck, National Health Insurance, at Out-of-Pocket structures.
- Ang U.S. health care ay hybrid na pinagsasama ang elements ng lahat ng apat na major model archetypes.
- Kabilang sa U.S. delivery ang for-profit, not-for-profit, at government institutions sa public at private sectors.
- Pinapahusay ng integrated delivery systems ang continuity sa pamamagitan ng pag-uugnay ng services at impormasyon sa iba’t ibang care settings.
- Sumasaklaw ang delivery settings sa inpatient, subacute, outpatient, post-acute, at community adult-care services, bawat isa ay may magkakaibang goals at staffing intensity.
- Binabago ng organization type ang tax, profit, charity-care, at safety-net obligations na direktang nakaaapekto sa access pathways.
- Maaaring tumaas ang U.S. health spending habang nahuhuli ang outcomes kumpara sa peer nations, kaya dapat husgahan ang financing decisions batay sa value at hindi sa spending volume lamang.
- Maaaring maging pangunahing expenditure driver ang diffusion ng bagong medical technology, kaya dapat gumamit ang adoption decisions ng malinaw na cost-effectiveness at equity criteria.
- Pinalawak ng ACA (nilagdaan noong March 2010) ang coverage sa pamamagitan ng mas matibay na preexisting-condition protections at mas malawak na essential-benefit access.
- Pinahusay ng ACA-era protections ang fairness, ngunit naaapektuhan pa rin ang aktuwal na access ng affordability pressure (premiums, out-of-pocket costs, at formulary limits).
- Pinagsasama ng U.S. funding streams ang government programs, employer/Marketplace private insurance, at self-pay pathways na lumilikha ng magkakaibang access constraints.
- Patuloy na binabago ng demographic shifts (aging population, increasing diversity, at immigration-driven growth) ang service demand at delivery priorities.
- Gumagamit ang public-health policy delivery ng mechanism categories tulad ng fiscal policy, regulation, education, preventive treatment, at screening.
- Nahuhubog ang pharmaceutical affordability at access ng global supply-chain resilience, PBM pricing intermediaries, at policy levers tulad ng Medicare inflation-rebate requirements.
- Magkaugnay ang laws at policies ngunit hindi mapagpapalit: ang laws ay government-enforced rules, habang ang policies ay structured action frameworks na ginagamit ng governments, professions, at institutions.
Pisyopatolohiya
Inilalarawan ng konseptong ito ang macro-level health system design sa halip na disease physiology. Naaapektuhan ng system structure ang access, coordination, affordability, at quality outcomes.
Ang fragmentation sa financing at delivery structures ay maaaring magdulot ng hindi pantay na access at duplicated services. Binabawasan ng integrated structures ang mga risk na ito sa pamamagitan ng unified networks at shared data.
Klasipikasyon
- Financing models: Beveridge, Bismarck, National Health Insurance, Out-of-Pocket.
- Payment-model structure domain: Core models (fee-for-service, capitation, bundled/episode-based), supplementary models (pay-for-performance, shared savings, retainer-based), at organizational models (ACO, medical home) na ginagamit sa mixed combinations.
- Economics lens: Sinusuri ng macroeconomics ang society-level spending decisions; sinusuri ng microeconomics ang organizational at individual financial decisions.
- Hybrid-model implementation: Maaaring sumunod ang national systems sa isang dominant model, habang hinahalo ng U.S. delivery ang model elements ayon sa payer at setting.
- Cost-driver lens: Intrinsic drivers (aging demographics, chronic-disease burden, demand growth) at extrinsic drivers (technology, prescription pricing, workforce costs, policy environment).
- Pharmaceutical supply-chain domain: Nakasalalay ang medication availability sa global raw-material sourcing, manufacturing capacity, distributor logistics, at regulatory oversight continuity.
- PBM pricing-intermediary domain: Nakikipag-negosasyon ang pharmacy benefit managers sa drug prices at formulary access sa pagitan ng manufacturers, insurers/employers, pharmacies, at government programs.
- Drug-price escalation drivers: Limited competition/monopoly conditions, mataas na development costs at mahabang approval timelines, severe-disease demand inelasticity, at policy influence mula sa industry lobbying.
- Inflation-rebate policy domain: Ang Medicare-focused inflation rebate requirements ay policy tool na naglalayong limitahan ang sobrang year-over-year price growth.
- ACA policy domain: Marketplace plan pathways, preexisting-condition protections, reduced exclusion-limit risk, preventive-service coverage rules, essential-benefit access, at insurer-appeal safeguards.
- U.S. funding-stream domain: Government funding (Medicare/Medicaid at iba pang public programs), private insurance, at self-pay.
- Medicare structure domain: Part A (inpatient/skilled nursing/hospice/some home health), Part B (outpatient/provider/preventive services), Part C (private Medicare Advantage na pinagsasama ang A/B at madalas D), at Part D (prescription coverage na may plan formulary variation).
- Medicaid structure domain: Joint federal-state low-income coverage na may state-level service variation at ACA-linked expansion pathways.
- Other public-coverage domain: CHIP, military/veteran systems, at iba pang federally/state-supported special-population programs.
- Insurance-plan design domain: HMO, PPO, POS, at HDHP/HSA structures na may magkakaibang tradeoffs sa premium, network flexibility, referral/preauthorization burden, at upfront cost sharing.
- Cost-sharing domain: Naiimpluwensiyahan ng deductible at copay requirements kung praktikal bang magamit ng insured clients ang kinakailangang care.
- Ownership structures: For-profit, not-for-profit, state/local government.
- Institution types: Public institutions, private institutions, at federally run service systems.
- Delivery design: Stand-alone sites kumpara sa integrated delivery systems (IDS).
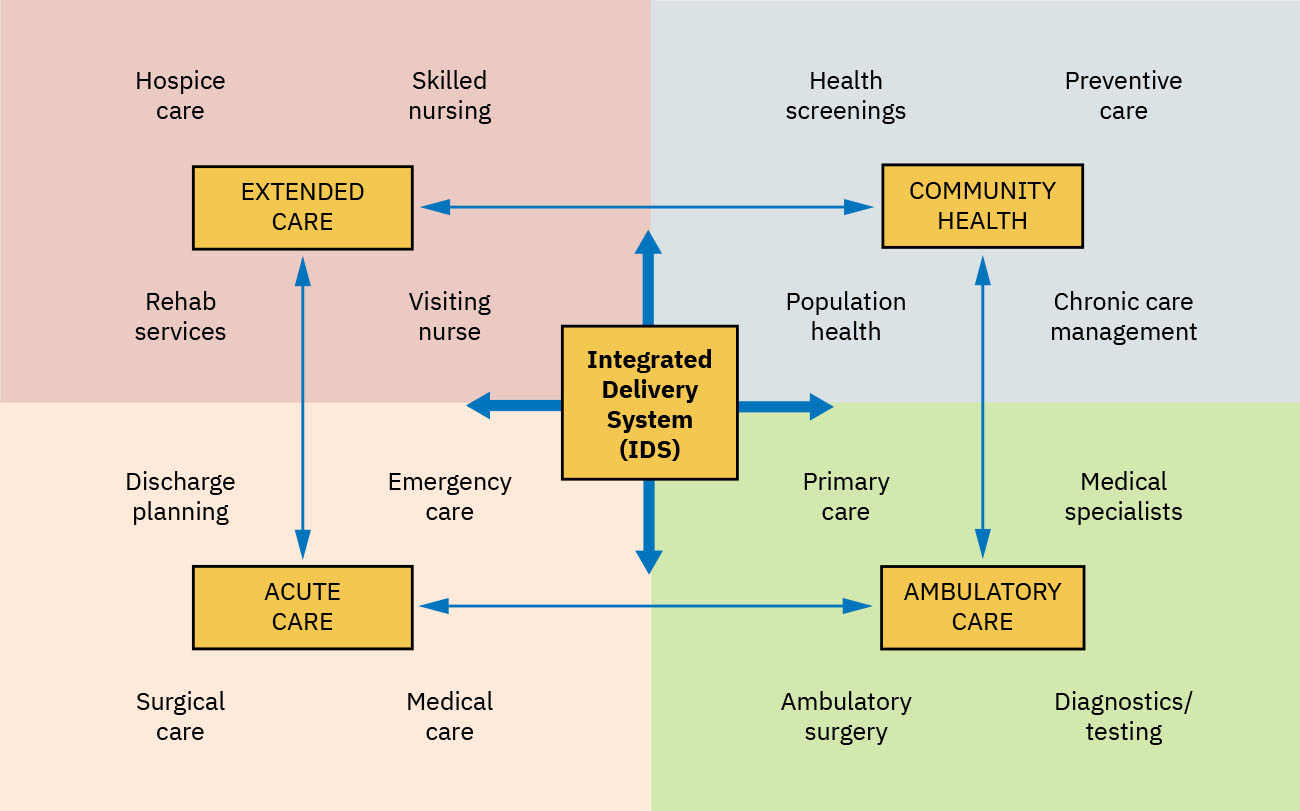 Illustration reference: OpenStax Fundamentals of Nursing Ch.3.2.
Illustration reference: OpenStax Fundamentals of Nursing Ch.3.2.
- Service-continuum domain: Inpatient acute care, subacute skilled services, outpatient/ambulatory care, post-acute recovery support, at community adult-care services.
- Care-desert domain: Mga rehiyong may limitadong hospitals/clinics, specialist access, trauma access, maternal services, o pharmacy services; kadalasang lumalala dahil sa rural hospital closure at workforce shortage.
- Community-support service domain: Home health, hospice, infusion therapy, adult day care, at in-home assistance na may magkakaibang skill scope at supervision requirements.
- Public-agency support domain: Tinutulungan ng Medicare/Medicaid-linked programs at state-local agencies (halimbawa aging at disability services) na tulayin ang access gaps na may state-level variation.
- Organizational decision test: Funding source, profit expectation/disposition, tax status, at safety-net obligation ang nagtatakda ng operational type.
- Care-level governance pattern: Sa ilang systems, hiwalay ang primary/secondary/tertiary roles sa magkakaibang practitioner tracks, habang sa iba ay pinapayagan ang fluid cross-level practice.
- For-profit profile: Investor-funded, tax-paying institutions na may shareholder return expectations at mas mababang routine safety-net scope.
- Not-for-profit profile: Tax-exempt institutions na may inaasahang community-service at charity-care; nire-reinvest ang profits sa halip na ipinamamahagi.
- State/local government profile: Publicly funded, tax-exempt institutions na may malinaw na safety-net responsibilities para sa uninsured o underinsured populations.
- Public-versus-private operational lens: Government-run at population-oriented ang public institutions; non-government run ang private institutions at kabilang dito ang for-profit at not-for-profit entities.
- Public-health governance layer: Nagtatakda ang federal at state/local public-health agencies ng policy at oversight conditions na nakaaapekto sa lahat ng delivery organizations.
- Policy-versus-law domain: Ang laws ay enacted regulatory rules na may enforcement consequences; ang policies ay deliberative action plans na nag-o-operationalize ng goals sa systems at organizations.
- Policy-type taxonomy domain: Public policy (government regulation), health policy (health-goal pathway), social policy (population welfare), nursing policy (practice boundaries/requirements), at institutional policy (organization-specific rules).
- Policy cultural-fit domain: Dapat isaalang-alang ng policy design ang culture/religion/ethnicity at gumamit ng trusted community leaders sa planning upang mapahusay ang adoption at mabawasan ang inequitable impact.
- Public-health delivery-mechanism domain: Maaaring gumamit ang policy execution ng fiscal tools (subsidies/taxes/free services), regulation, health education/health-literacy support, preventive treatment pathways, at screening programs.
- State/local public-health operations: Immunization at family services, communicable-disease surveillance/reporting, emergency preparedness, at community vital-record workflows.
- IDS function profile: Mga network na nagbabahagi ng impormasyon, responsibilidad, at resources upang i-coordinate ang primary, secondary, at tertiary care.
- Primary-care medical-home link: Praktikal na halimbawa ng IDS kung saan ang primary care ang anchor ng multi-level coordination.
- Nonfederal IDS profile: Community-facing systems na pinagsasama ang hospitals at outpatient sites na may shared EHR-based continuity sa lahat ng care levels.
- Community-hospital profile: Nonfederal hospitals na nagsisilbi sa pangkalahatang publiko; maaaring integrated sa mas malalaking systems o stand-alone sites.
- Federal-system profile: Population-specific IDS structures (halimbawa veteran, tribal/indigenous, at military-family systems) na may eligibility-based access.
- Federal IDS examples: Veteran, tribal/indigenous, at military health systems na naghahatid ng multi-level care sa loob ng dedicated networks.
- Provider-practice structure: Independent (solo) practices kumpara sa group practices, na may tuloy-tuloy na consolidation patungo sa mas malalaking groups sa maraming merkado.
Pagsusuri sa Pag-aalaga
Pokus sa NCLEX
Iugnay ang patient barriers at care delays sa system-level factors tulad ng insurance, network structure, at referral pathways.
- Suriin ang insurance/coverage context at malamang na affordability barriers.
- Suriin kung aling system type ang dina-navigate ng pasyente (public, private, IDS, federal).
- Suriin ang referral pathway complexity at risk ng service fragmentation.
- Suriin ang continuity threats sa panahon ng cross-organization transitions.
- Suriin ang equity implications para sa underserved populations.
- Suriin kung nalilito ang mga pasyente sa levels of prevention at levels of care, na maaaring magbaluktot ng expectations at care navigation.
- Suriin ang malamang na transfer destination kung ang kasalukuyang institution ay hindi gumagana bilang safety-net site.
- Suriin ang risk na maaaring mabawasan ang local access dahil sa profit-driven service lines o site closures, lalo na sa rural settings.
- Suriin kung ang uninsured/underinsured patients ay maaaring dumaan sa stabilization-then-transfer workflows at maghanda ng continuity safeguards.
- Suriin ang federal-system eligibility (halimbawa veteran, tribal affiliation/service pathways, military family status) bago mag-assume ng standard community-network referral options.
- Suriin kung dominated ng malalaking groups o independent practices ang local provider market, dahil maaaring magkaiba ang availability at after-hours access patterns.
- Suriin kung tumataas ang cost burden ng local care plans nang walang malinaw na outcome gain at i-escalate ang value-review concerns sa pamamagitan ng quality channels.
- Suriin kung ang insured patients ay may practical affordability barriers pa rin (premium burden, deductibles, noncovered drugs, o formulary restrictions).
- Suriin kung ang plan structure ng pasyente (halimbawa HMO referral limits o high deductible) ay humaharang sa napapanahong diagnostics, specialist access, o medication pickup.
- Suriin ang Medicare/Medicaid eligibility context at state-variation effects bago mag-assume ng uniform benefits.
- Suriin kung ang kasalukuyang needs ng pasyente ay mas tugma sa inpatient, subacute, outpatient, post-acute, o community-based adult-care services.
- Suriin kung nauunawaan ng mga pasyente at caregivers ang pagkakaiba ng skilled home health services at non-skilled in-home assistance.
Mga Interbensyon sa Pag-aalaga
- Gabayan ang mga pasyente sa system navigation at referral processes.
- Makipag-coordinate sa case management para sa network, coverage, at access barriers.
- Gumamit ng integrated records at structured handoff upang mabawasan ang duplication.
- I-escalate ang system barriers na nakaaapekto sa napapanahong care delivery.
- Suportahan ang patient-centered planning na akma sa aktuwal na coverage at resource constraints.
- Ituro na ang prevention levels (primary/secondary/tertiary prevention) ay action domains at hindi kapareho ng care-level complexity.
- I-pre-brief ang mga pasyente sa posibleng stabilization-and-transfer pathways kapag limitado ang institutional safety-net scope.
- I-activate ang state/local public-health resources kapag kailangan ang preventive services o safety-net access lampas sa hospital-based care.
- I-verify nang maaga ang charity-care at coverage-support pathways kapag ang organization type ay nagpo-predict ng financial barriers.
- Gamitin ang shared-record capability sa integrated systems upang mabawasan ang duplicate diagnostics at transition information loss.
- Para sa federal-system-eligible patients, i-route ang referrals sa loob ng parehong IDS kapag posible upang mapanatili ang benefit alignment at continuity.
- I-route ang eligible patients sa state/local public-health programs (halimbawa vaccination, family services, o reportable-condition follow-up) upang maisara ang prevention at continuity gaps.
- Sa cost-sensitive planning, i-prioritize ang interventions at technologies na may mas malakas na outcome benefit kumpara sa dagdag na cost at iwasan ang low-value duplication.
- Para sa ACA/Marketplace-covered patients, i-verify nang maaga ang plan-network at formulary fit at tumulong sa insurer-appeal pathways kapag indikado.
- Para sa self-pay o underinsured patients, mag-refer nang maaga sa case management/social work/financial counselors para sa Marketplace o public-program screening.
- Sa discharge planning, iayon ang recommended follow-up sites at medications sa aktuwal na network at cost-sharing constraints ng pasyente.
- Ikonekta ang eligible patients at caregivers sa community at public-agency supports (halimbawa aging services, waiver pathways, at local adult-care resources) upang mapanatili ang home at post-acute care plans.
- Itugma ang target outcomes sa pinakaangkop na delivery mechanism (fiscal, regulatory, education, preventive treatment, o screening) at tukuyin ang measurement bago rollout.
- Kapag nagdidisenyo o nagpapatupad ng policy sa diverse communities, isama nang maaga ang cultural-group leaders upang ma-validate ang values, acceptability, at practical implementation barriers.
- Para sa medication-access planning, isama ang drug-supply reliability checks at early contingency pathways (formulary alternatives, therapeutic substitutions, at refill continuity planning) kapag ang shortages o price spikes ay nagbabanta sa treatment adherence.
System-Blind Planning
Maaaring mabigo pa rin ang clinically correct plan kung hindi matutugunan ang delivery-model constraints at access barriers.
Parmakolohiya
Malakas ang impluwensiya ng coverage model at formulary structure sa medication access; dapat asahan ng mga nurse ang affordability at access barriers kapag nagpaplano ng treatment.
Paglalapat ng Klinikal na Paghuhusga
Klinikal na Sitwasyon
Tumatanggap ang pasyente ng specialty recommendations ngunit hindi nakaka-follow-up dahil sa network confusion at cost concerns.
- Recognize Cues: Ang pagkabigo ng care plan ay kaugnay ng system navigation at affordability barriers.
- Analyze Cues: Structural factors, hindi lamang patient motivation, ang nagtutulak ng nonadherence.
- Prioritize Hypotheses: Prayoridad ang muling pagdisenyo ng plan para tumugma sa delivery-model realities.
- Generate Solutions: Isama ang care coordination, i-verify ang network options, at pasimplehin ang referral path.
- Take Action: Ipatupad ang revised system-aligned follow-up plan.
- Evaluate Outcomes: Humuhusay ang attendance at continuity.
Mga Kaugnay na Konsepto
- balangkas ng levels of care: primary, secondary, at tertiary - Operational movement sa system tiers.
- patient care coordination, interdisciplinary referrals, at case management - Team workflow para sa structural complexity.
- communication barriers, emotional intelligence, at bias awareness - Mga communication factor na nagpapalala ng system barriers.
Sariling Pagsusuri
- Paano naaapektuhan ng financing models ang patient access sa care?
- Bakit madalas mapabuti ng integrated delivery systems ang continuity?
- Aling nursing actions ang pinakamainam para mabawasan ang pinsala mula sa organizational fragmentation?