Invasive Mechanical Ventilation Modes
Key Points
- Invasive mechanical ventilation requires an advanced airway and is commonly delivered in full-support control modes.
- In volume control, tidal volume delivery is fixed while airway pressures vary with resistance and compliance.
- In pressure control, inspiratory pressure is fixed while delivered tidal volume varies breath to breath.
- Plateau pressure is ideally kept below 30 cm H2O, with an upper limit around 35 cm H2O, to reduce alveolar injury risk.
- Mode selection must match patient drive context: partial support for spontaneous effort versus full-control support in deeply sedated or pharmacologically paralyzed states.
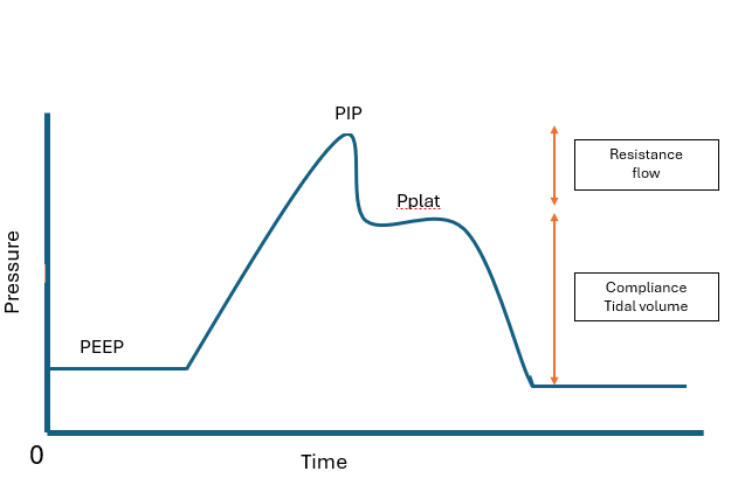 Illustration reference: OpenRN Respiratory Therapy Ch.2.1.
Illustration reference: OpenRN Respiratory Therapy Ch.2.1.
Pathophysiology
Invasive ventilation supports gas exchange when spontaneous breathing is inadequate or unsafe. Ventilator mode selection determines whether the system prioritizes consistent volume delivery or consistent pressure delivery, which directly affects oxygenation strategy, carbon dioxide clearance, and lung-protection behavior.
Operationally, invasive support may be configured to assist patient-triggered breaths or to fully provide ventilation when neurologic injury, severe fatigue, or treatment strategy requires suppression of spontaneous respiratory effort.
In volume control, minute ventilation planning is straightforward because set tidal volume and respiratory rate determine baseline delivered ventilation. However, higher airway resistance or lower compliance can increase required pressures. In pressure control, constant inspiratory pressure may improve pressure-limitation goals, but tidal volume must be trended closely because delivered volume changes with lung mechanics.
Classification
- Assist-control volume control (ACVC/VC/CMV-VC): Clinician sets tidal volume and minimum respiratory rate; pressure varies to deliver target volume.
- Assist-control pressure control (ACPC/PCV/CMV-PC): Clinician sets pressure and minimum respiratory rate; tidal volume varies based on mechanics.
- Shared settings across modes: PEEP and FiO2 are set in all modes and require continuous reassessment.
- FiO2 range context: In invasive ventilation, FiO2 can be adjusted broadly (about 21%-100%) based on oxygenation targets and injury-risk balancing.
Nursing Assessment
NCLEX Focus
Questions often test which variable is fixed versus variable in VC and PC and which pressure thresholds indicate lung-injury concern.
- Assess airway status and ventilator mode appropriateness for current lung mechanics.
- Monitor peak and plateau pressure trends and escalate when pressures rise unexpectedly.
- In VC, evaluate pressure changes as potential markers of worsening resistance/compliance.
- In PC, monitor delivered tidal volume trends to ensure ventilation remains effective and safe.
Nursing Interventions
- Verify ordered mode and core settings (RR, FiO2, PEEP, and mode-specific control parameter) at initiation and handoff.
- Coordinate frequent mode/setting reassessment with respiratory therapy and provider teams as patient condition changes.
- In VC, track flow or inspiratory-time relationship because higher flow shortens inspiratory time.
- In PC, trend exhaled tidal volumes and notify team if volumes fall outside safe/effective targets.
- Collaborate with respiratory therapy to adjust settings when pressures, volumes, or gas exchange goals are not met.
- Perform sterile in-line airway suctioning when secretion burden interferes with ventilation effectiveness.
- Escalate concern promptly when pressure thresholds suggest possible ventilator-induced lung injury risk.
Pressure-Related Lung Injury Risk
Sustained high airway/plateau pressures can damage alveoli and worsen pulmonary outcomes.
Pharmacology
| Drug Class | Examples | Key Nursing Considerations |
|---|---|---|
| oxygen-therapy | FiO2 titration context | Adjust FiO2 with team to balance oxygenation goals and oxygen-toxicity risk over time. |
| sedative-hypnotics | Ventilator synchrony context | Monitor sedation response and safety because synchrony and tolerance can influence ventilation effectiveness. |
| Neuromuscular-blocking therapy | Paralysis context for severe asynchrony | If paralysis is used, ensure adequate sedation/analgesia and continuous monitoring because patients cannot signal distress. |
Clinical Judgment Application
Clinical Scenario
A ventilated patient in volume control develops rising peak pressures without a clinician setting change.
- Recognize Cues: Pressure trend rises while target tidal volume remains fixed.
- Analyze Cues: Worsening airway resistance or reduced compliance may be increasing pressure requirement.
- Prioritize Hypotheses: Immediate priority is preventing pressure-related lung injury while maintaining ventilation.
- Generate Solutions: Reassess mode settings, evaluate lung mechanics, and consider alternative control strategy if indicated.
- Take Action: Notify team, trend plateau pressure, and support rapid ventilator reassessment.
- Evaluate Outcomes: Pressures normalize and ventilation goals remain within safe targets.
Related Concepts
- noninvasive-positive-pressure-ventilation - Noninvasive support may precede invasive ventilation escalation.
- advanced-airways-and-intubation - Invasive ventilation depends on secure advanced airway placement.
- endotracheal-intubation-procedure - Procedure-level steps for establishing invasive airway access.
- respiratory-failure - Primary indication context for full ventilatory support.
- airway-suctioning - Secretion management is essential during mechanical ventilation.
Self-Check
- Which variable is fixed in volume control versus pressure control modes?
- Why can rising pressures in volume control signal worsening lung mechanics?
- How does trending tidal volume in pressure control support patient safety?